Article
Ischemic heart disease and acute cardiac care
REC Interv Cardiol. 2019;1:21-25
Access to side branches with a sharply angulated origin: usefulness of a specific wire for chronic occlusions
Acceso a ramas laterales con origen muy angulado: utilidad de una guía específica de oclusión crónica
Servicio de Cardiología, Hospital de Cabueñes, Gijón, Asturias, España

ABSTRACT
Introduction and objectives: De-escalation from prasugrel and ticagrelor to clopidogrel in patients undergoing percutaneous coronary intervention after acute coronary syndrome (ACS) is a strategy aimed at reducing bleeding. This study evaluates whether VerifyNow (Werfen, Spain)–guided de-escalation, based on platelet aggregation measurement, provides a therapeutic benefit in ACS management.
Methods: This ongoing multicenter, prospective, randomized 1:1 trial will enroll 634 patients with ACS who underwent revascularization with a sirolimus-eluting stent and were discharged on dual antiplatelet therapy with ticagrelor or prasugrel. Only those patients with a very low platelet reactivity level (platelet reactivity units ≤ 30) based on VerifyNow 1 month after discharge will be included. The primary endpoint is a composite of cardiovascular death, nonfatal acute myocardial infarction, nonfatal stroke, and bleeding at 1-year follow-up.
Results: The EPIC17-VERONICA study (NCT04654052) will reveal the efficacy profile of the de-escalation strategy, based on the VerifyNow platelet aggregation test, and determine the role of this device in the selection of patients who are eligible to benefit from this strategy.
Conclusions: This study will determine whether platelet function testing provide clinical benefit in the management of patients with ACS.
Keywords: Acute coronary syndrome. Antiplatelet therapy. Platelet function test. Bleeding.
RESUMEN
Introducción y objetivos: La desescalada desde prasugrel y ticagrelor a clopidogrel en pacientes tras intervencionismo coronario percutáneo por síndrome coronario agudo (SCA) constituye una de las estrategias para intentar disminuir las hemorragias. El objetivo de este estudio es averiguar si dicha desescalada guiada por la prueba de agregación plaquetaria VerifyNow (Werfen, España) tiene un efecto beneficioso en el tratamiento del SCA.
Métodos: Estudio multicéntrico, prospectivo y aleatorizado 1:1, en curso. Se incluirán 634 pacientes con SCA y revascularización con stent de sirolimus que sean dados de alta con doble terapia antiagregante con ticagrelor o prasugrel. Solo se incluirán aquellos con un nivel de reactividad plaquetaria muy bajo (unidades de reactividad plaquetaria ≤ 30) basado en VerifyNow al mes del alta. El objetivo primario es un combinado de muerte por causa cardiovascular, infarto agudo de miocardio no fatal, accidente cerebrovascular no fatal y sangrado en un seguimiento a 1 año.
Resultados: El estudio EPIC17-VERONICA (NCT04654052) permitirá averiguar la eficacia de la estrategia de desescalada basada en la prueba de agregación plaquetaria VerifyNow, además de conocer el papel de este dispositivo en la selección de los pacientes candidatos a beneficiarse de esta estrategia.
Conclusiones: Este estudio determinará si las pruebas de función plaquetaria aportan beneficio en el tratamiento tras el SCA.
Palabras clave: Síndrome coronario agudo. Terapia antiagregante. Prueba de función plaquetaria. Sangrado.
Abbreviations
ACS: acute coronary syndrome. PCI: percutaneous coronary intervention. PRU: platelet reactivity units.
INTRODUCTION
Following percutaneous coronary intervention (PCI) in patients with acute coronary syndrome (ACS), a 12-month regimen of dual antiplatelet therapy with a P2Y12 receptor inhibitor and acetylsalicylic acid is recommended, regardless of the type of stent implanted, except when contraindicated.1 Although prasugrel and ticagrelor are preferred over clopidogrel in this setting, there is ongoing debate regarding the potency and duration of dual antiplatelet therapy. This controversy stems from the fact that most patients concurrently face 2 opposing and potentially fatal risks—ischemic and hemorrhagic—which must be carefully balanced on an individual basis.
The introduction of stents with reduced thrombogenicity, together with evidence that thrombotic risk is highest during the first few months after PCI while hemorrhagic risk remains relatively constant throughout time, has led to research efforts focused on minimizing bleeding complications. These strategies include shortening dual antiplatelet therapy, using P2Y12 inhibitors as monotherapy, and implementing de-escalation strategies.2,3
De-escalation consists of switching from prasugrel or ticagrelor to clopidogrel and can be guided (using genetic or platelet function testing) or unguided. Because this strategy may increase ischemic events, it is not recommended within the first month after PCI.1
In the TOPIC trial,4 the unguided de-escalation strategy initiated 1 month after ACS significantly reduced hemorrhagic events (Bleeding Academic Research Consortium [BARC] grade ≥ 2 bleeding events) at 1 year without increasing the ischemic ones. In the TROPICAL-ACS trial,5 the platelet function testing–guided de-escalation from prasugrel to clopidogrel 2 weeks after revascularization was noninferior to standard therapy, showing a trend toward fewer hemorrhages at 12 months and a similar rate of thrombotic events.1,2,6 In the TALOS-AMI trial,7 12-month event rates were lower, primarily because of fewer hemorrhagic events among patients who underwent unguided de-escalation 1 month after ACS. Table 1 summarizes these studies.
Table 1. De-escalation clinical trials in patients with acute coronary syndrome
| TOPIC (2017)4 | TROPICAL-ACS (2018)5 | TALOS-AMI (2021)12 | |
|---|---|---|---|
| Population | n = 645 | n = 2610 | n = 2697 |
| Design | Open-label, single-center, randomized, superiority trial | Open-label, multicenter, randomized, noninferiority trial | Open-label, multicenter, randomized, noninferiority trial |
| Strategy | Standard therapy vs unguided de-escalation | Standard therapy vs platelet function testing–guided therapy (Multiplate device) | Standard therapy vs unguided de-escalation |
| Control group | Continued dual antiplatelet therapy with acetylsalicylic acid and ticagrelor or prasugrel | Continued dual antiplatelet therapy with acetylsalicylic acid and prasugrel | Continued dual antiplatelet therapy with acetylsalicylic acid and ticagrelor |
| Experimental group | De-escalation to acetylsalicylic acid and clopidogrel | 1-week regimen of prasugrel, followed by 1-week regimen of clopidogrel and either prasugrel or clopidogrel from day 14 onward, according to platelet function testing results | De-escalation to acetylsalicylic acid and clopidogrel |
| Time from revascularization to de-escalation | 1 month | 2 weeks | 1 month |
| Follow-up | 1 year | 1 year | 1 year |
| Primary endpoint | Cardiac death, emergency revascularization, stroke, or BARC ≥ 2 bleeding events | Cardiac death, myocardial infarction, stroke, or BARC ≥ 2 bleeding events | Cardiac death, myocardial infarction, stroke, or BARC ≥ 2 bleeding events |
| Results | 13.4% in experimental group vs 26.3% in control group (HR, 0.48; 95%CI, 0.34–0.68; P < .01) | 7.3% in experimental group vs 9.0% in control group (HR, 0.81; 95%CI, 0.62–1.06; P = .0004) | 4.6% in experimental group vs 8.2% in control group (HR, 0.55; 95%CI, 0.42–0.76; P < .0001) |
|
95%CI, 95% confidence interval; BARC, Bleeding Academic Research Consortium; HR, hazard ratio. |
|||
After the positive results of the TOPIC trial, the VerifyNow to optimise platelet inhibition in coronary acute syndrome (EPIC17-VERONICA) trial (ClinicalTrials.gov: NCT04654052) aims to further refine this strategy by only applying de-escalation to patients with excessive antiplatelet effects from prasugrel or ticagrelor after the first month who are at theoretical risk of hemorrhage based on the VerifyNow platelet aggregation test (Werfen, Spain). Thus, patients demonstrating an adequate pharmacologic response will continue prasugrel or ticagrelor therapy for 1 year, whereas those with very low platelet reactivity after a 1-month regimen of dual antiplatelet therapy with these agents constitute the target population of this study.
METHODS
Design
We are conducting a multicenter, prospective, randomized clinical trial at 16 Spanish centers. Based on the results of the platelet aggregation test for P2Y12 inhibition (platelet reactivity units [PRU]) using the VerifyNow system, patients with very low platelet reactivity (PRU ≤ 30) are randomized in a 1:1 ratio to either continue treatment with ticagrelor or prasugrel, or to de-escalate to clopidogrel. Patients with PRU > 30 are not randomized. The study flowchart is shown in figure 1.
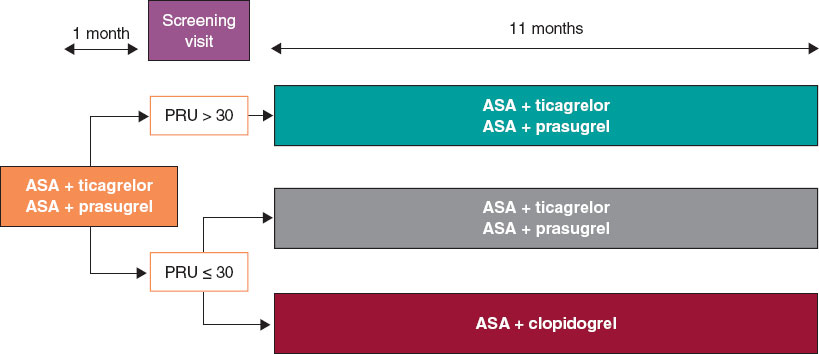
Figure 1. Study flowchart. AAS, acetylsalicylic acid; PRU, platelet reactivity units.
The study is being conducted in full compliance with the principles outlined in the Declaration of Helsinki and has been approved by the central ethics committee (Comité del Bierzo, León, Spain) and endorsed by the ethics committees of all participant centers. The appendix lists the participant centers and principal investigators.
The study sponsor (Fundación para la Educación en Procedimientos de Intervencionismo en Cardiología [EPIC]) is fully responsible, together with the principal investigators, for data management and confidentiality.
Population
Inclusion and exclusion criteria
Table 2 summarizes the inclusion and exclusion criteria. Briefly, all patients with ACS undergoing PCI with a sirolimus-eluting stent and a bioresorbable polymer during hospitalization and discharged on dual antiplatelet therapy with acetylsalicylic acid and ticagrelor or prasugrel are eligible for inclusion.
Table 2. Inclusion and exclusion criteria
| Inclusion criteria |
|---|
| Patients > 18 years |
| Patients with acute coronary syndrome undergoing percutaneous revascularization with a sirolimus-eluting stent with a bioresorbable polymer and discharged on dual antiplatelet therapy with acetylsalicylic acid and ticagrelor or prasugrel |
| Signed informed consent |
| Exclusion criteria |
| History of intracranial hemorrhage |
| Contraindication to acetylsalicylic acid, clopidogrel, prasugrel, or ticagrelor |
| Major ischemic or bleeding events during the first month of antiplatelet therapy |
| Thrombocytopenia < 50 000/µL |
| Permanent oral anticoagulation |
| Pregnancy or breastfeeding |
| Inability to complete the 1-year follow-up |
| Life expectancy < 24 months |
Written informed consent must be obtained before the platelet aggregation tes is performed.
Study protocol and randomization
Eligible patients are scheduled for P2Y12 receptor inhibition testing with the VerifyNow system between 30 and 40 days after hospital discharge. Measurements are obtained at least 6 hours after the administration of the last P2Y12 inhibitor dose. Patients with PRU ≤ 30 (very low platelet reactivity) are randomized in a 1:1 ratio using an electronic system to either continue their current treatment or de-escalate to clopidogrel, 75 mg once daily. De-escalation is preceded by a loading dose of 600 mg administered 24 hours after the last dose of ticagrelor or 75 mg 24 hours after the last dose of prasugrel, in accordance with the 2017 European Society of Cardiology clinical practice guidelines.8
The remaining patients with PRU > 30 are not randomized, and their dual antiplatelet therapy remains unchanged from discharge.
Clinical follow-up
Patients in the 2 randomized groups undergo telephone follow-up to monitor clinical events at 2, 5, 8, and 11 months after enrollment, corresponding to 3, 6, 9, and 12 months after hospital discharge.
For patients with PRU > 30 on the 1-month VerifyNow platelet aggregation test who are not randomized, only baseline characteristics are recorded, and no further follow-up is conducted.
Protocol of the VerifyNow platelet aggregation test
The VerifyNow system determines platelet activity by measuring in vitro aggregation in a blood sample exposed to specific agonists. This optical detection instrument (figure 2), which operates on a turbidimetric principle, uses single-use cartridges. In this study, PRUTest-specific kits are employed. (Werfen, Spain) to assess platelet aggregation while on P2Y12 receptor inhibitor therapy (ticagrelor, prasugrel, and clopidogrel). Each PRUTest kit contains lyophilized microbeads coated with fibrinogen, platelet activators, and a buffered solution. The test is based on the ability of activated platelets to bind fibrinogen-coated microbeads. Light transmission increases as activated platelets bind to and aggregate with the fibrinogen-coated microspheres. The kit measures this change in the optical signal and reports the results in PRU units (figure 3).

Figure 2. VerifyNow system. Reproduced with permission from Werfen.
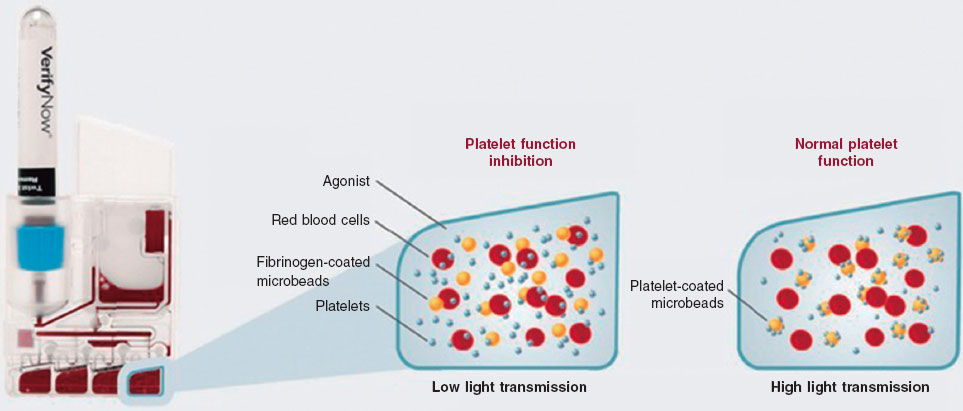
Figure 3. Performance of the VerifyNow system based on light transmission aggregometry. Light transmission increases as activated platelets bind and aggregate to the fibrinogen-coated microbeads in the kit. Therefore, high light transmission (corresponding to elevated platelet reactivity unit [PRU] values) indicates normal platelet function, whereas low light transmission (decreased PRU values) reflects platelet inhibition induced by the tested drugs.
An antiplatelet effect of the drug is considered present with PRU ≤ 180 (figure 4). Only patients with PRU ≤ 30 are randomized, as these are considered to have very low platelet reactivity while on antiplatelet therapy.
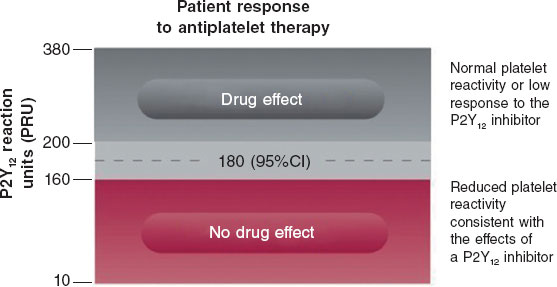
Figure 4. Reference levels for platelet reactivity units (PRU). 95%CI, 95% confidence interval.
Endpoints
The primary endpoint of the study is to compare the efficacy of de-escalation from ticagrelor or prasugrel to clopidogrel in patients undergoing PCI in the ACS setting, using the VerifyNow platelet aggregation test vs standard dual antiplatelet therapy at the 1-year follow-up. The rate of net adverse cardiovascular events is the primary endpoint of the study, defined as a composite of cardiac death, nonfatal myocardial infarction, nonfatal stroke, and hemorrhage (defined as Bleeding Academic Research Consortium [BARC] grade ≥ 2 bleeding events). The BARC scale is shown in table S1.
Furthermore, the study aims to compare several secondary endpoints (table 3), such as the occurrence of ischemic events during follow-up: cardiac death and all-cause mortality, acute myocardial infarction, stroke, stent thrombosis, and need for emergency revascularization. Moreover, the hemorrhage rate (defined as BARC grade ≥ 2 bleeding events) will be compared. The definitions of all study endpoints are shown in table S2.
Table 3. Endpoints of the study
| Primary endpoint |
|---|
| To compare the percentage of net adverse cardiovascular events between the 2 subgroups of patients with low platelet reactivity (PRU ≤ 30) who were randomized to de-escalation to clopidogrel vs standard therapy |
| Secondary endpoints |
| To compare the rate of cardiac death between the 2 randomized patient subgroups |
| To compare the rate of all-cause mortality between the 2 randomized patient subgroups |
| To compare the rate of acute myocardial infarction between the 2 randomized patient subgroups |
| To compare the rate of stroke between the 2 randomized patient subgroups |
| To compare the rate of stent thrombosis between the 2 randomized patient subgroups |
| To compare the rate of emergency revascularization between the 2 randomized patient subgroups |
| To compare the rate of bleeding events (defined as BARC ≥ 2) between the 2 randomized patient subgroups |
|
BARC, Bleeding Academic Research Consortium; PRU, platelet reactivity units. |
Statistics
Sample size calculation
Sample size was calculated for the randomized clinical trial cohort. The total number of patients (including those not randomized with PRU > 30) will depend on the total required to reach the estimated sample size for the randomized clinical trial.
We estimate a smaller difference in event rates across the groups than that observed in the TOPIC trial,4 specifically, 14% in the de-escalation group vs 22% in the standard therapy group. Assuming a significance level of 0.05, a power of 80%, a 2-tailed P-value and a 10% loss to follow-up, a total of 634 randomized patients (317 per group) will be required.
Statistical analysis plan
Quantitative variables will be expressed as mean and standard deviation if normally distributed, or as median and interquartile range otherwise. Categorical variables will be expressed as absolute values and percentages. Study data will be analyzed using one-way analysis of variance (ANOVA) for continuous variables, and Fisher’s exact or chi-square tests for categorical variables, as appropriate. Nonparametric tests will be used for variables that are not normally distributed or cannot be normalized. For the main outcome measure, Kaplan-Meier survival curves with log-rank statistics will be presented for prespecified criteria, and multivariable Cox regression will be performed to adjust for known risk factors and potential confounders. Hazard ratios and 95% confidence intervals will be reported for all statistically significant variables.
Intention-to-treat (according to randomization assignment) and per-protocol analyses (in case of crossover) will be conducted. The former will serve as the study primary analysis.
DISCUSSION
The EPIC17-VERONICA trial aims to demonstrate the efficacy of a VerifyNow platelet aggregation test-guided de-escalation strategy in reducing hemorrhagic events without increasing ischemic events in patients with ACS who have undergone percutaneous revascularization and exhibit very low platelet reactivity after the first month of treatment with prasugrel or ticagrelor.
The initial lack of expected results from platelet function testing to identify patients at risk for thrombotic events while on clopidogrel in the GRAVITAS,9 TRIGGER-PCI,10 and ARCTIC11 trials relegated its use to a class IIb recommendation in the European Society of Cardiology antiplatelet guidelines for determining the optimal timing of cardiac surgery after ACS.8 However, the 1-year results of the large-scale multicenter ADAPT-DES trial12 with 8500 PCI patients demonstrated that platelet reactivity assessed with the VerifyNow platelet aggregation test is an independent predictor of bleeding events.
In the TOPIC4 and TALOS-AMI7 trials, the unguided de-escalation strategy significantly reduced bleeding events without increasing ischemic events. In the TROPICAL-ACS5 trial, this platelet aggregation test–guided de-escalation strategy showed a trend toward fewer hemorrhages, with a similar rate of thrombotic complications.
The EPIC17-VERONICA study further seeks to improve the application of this de-escalation strategy by using the VerifyNow platelet aggregation test to identify patients with very low platelet reactivity (PRU ≤ 30) as those most likely to benefit from de-escalation.
CONCLUSIONS
The EPIC17-VERONICA trial has been designed to investigate the efficacy of de-escalating from the most potent antiplatelet agents (ticagrelor and prasugrel) to clopidogrel after the first month of therapy in patients with ACS and very low platelet reactivity, aiming to reduce bleeding events without increasing ischemic complications. Furthermore, it will provide evidence on the clinical utility of the VerifyNow platelet aggregation test for patient selection.
FUNDING
None declared.
ETHICAL CONSIDERATIONS
The study is being conducted in full compliance with the principles outlined in the Declaration of Helsinki on clinical research and has been approved by the central ethics committee (Comité del Bierzo, León, Spain) and endorsed by the ethics committees of all participant centers. Written informed consent is required prior to performing ant platelet aggregation measurements. Sex and gender bias considerations have been addressed.
STATEMENT ON THE USE OF ARTIFICIAL INTELLIGENCE
No artificial intelligence was used in the preparation of this manuscript.
AUTHORS’ CONTRIBUTIONS
C. Garilleti Cámara and I. Lozano Martínez-Luengas drafted the manuscript; the remaining authors critically revised the document and approved the final version.
CONFLICTS OF INTEREST
J.M. de la Torre-Hernández is Editor-in-Chief of REC: Interventional Cardiology; A. Pérez de Prado is Associate Editor of REC: Interventional Cardiology. In both cases, the journal’s editorial procedure to ensure impartial handling of the manuscript has been followed. The remaining authors declared no conflicts of interest whatsoever.
WHAT IS KNOWN ABOUT THE TOPIC?
- De-escalation from the most potent antiplatelet agents to clopidogrel is one of the strategies used to reduce hemorrhage after percutaneous revascularization in acute coronary syndrome. This de-escalation can be performed guided or unguided by genetic or platelet function testing.
WHAT DOES THIS STUDY ADD?
- The EPIC17-VERONICA trial is the first to use the VerifyNow platelet aggregation test to select patients eligible for de-escalation.
REFERENCES
1. Byrne RA, Rossello X, Coughlan JJ, et al. 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44:3720-3826.
2. Angiolillo DA, Galli M, Collet JP, Kastrati A, O’Donoghue MO. Antiplatelet therapy after percutaneous coronary intervention. EuroIntervention. 2022; 17:e1371-e1396.
3. Angiolillo DJ. The Evolution of Antiplatelet Therapy in the Treatment of Acute Coronary Syndromes. Drugs. 2012;72:2087-2116.
4. Cuisset T, Deharo P, Quilici J, et al. Benefit of switching dual antiplatelet therapy after acute coronary syndrome: the TOPIC (timing of platelet inhibition after acute coronary syndrome) randomized study. Eur Heart J. 2017;38:3070-3078.
5. Sibbing D, Aradi D, Jacobshagen C, et al. Guided de-escalation of antiplatelet treatment in patients with acute coronary syndrome undergoing percutaneous coronary intervention (TROPICAL-ACS): a randomised, open-label, multicentre trial. Lancet. 2017;390:1747-1757.
6. Gorog DA, Ferreiro JL, Ahrens I, et al. De-escalation or abbreviation of dual antiplatelet therapy in acute coronary syndromes and percutaneous coronary intervention: a Consensus Statement from an international expert panel on coronary thrombosis. Nat Rev Cardiol. 2023;20:830-844.
7. Kim CJ, Park MW, Kim MC, et al. Unguided de-escalation from ticagrelor to clopidogrel in stabilised patients with acute myocardial infarction undergoing percutaneous coronary intervention (TALOS-AMI): an investigator-initiated, open-label, multicentre, non-inferiority, randomised trial. Lancet. 2021;398:1305-1316.
8. Valgimigli A del G de TM, Bueno H, Byrne RA, et al. Actualización ESC 2017 sobre el tratamiento antiagregante plaquetario doble en la enfermedad coronaria, desarrollada en colaboración con la EACTS. Rev Esp Cardiol. 2018;71:42.e1-42.e58.
9. Price MJ, Berger PB, Teirstein PS, et al. Standard- vs high-dose clopidogrel based on platelet function testing after percutaneous coronary intervention: the GRAVITAS randomized trial. JAMA. 2011;305:1097-105. Erratum in: JAMA. 2011;305;2174. Stillablower, Michael E [corrected to Stillabower, Michael E]. PMID: 21406646.
10. Trenk D, Stone GW, Gawaz M, et al. A Randomized Trial of Prasugrel Versus Clopidogrel in Patients With High Platelet Reactivity on Clopidogrel After Elective Percutaneous Coronary Intervention With Implantation of Drug-Eluting Stents. J Am Coll Cardiol. 2012;59:2159-2164.
11. Collet JP, Cuisset T, Rangé G, et al. Bedside Monitoring to Adjust Antiplatelet Therapy for Coronary Stenting. N Engl J Med. 2012;367:2100-2109.
12. Sibbing D, Schulz S, Braun S, et al. Antiplatelet effects of clopidogrel and bleeding in patients undergoing coronary stent placement. J Thromb Haemost. 2010;8:250-256.

ABSTRACT
Introduction and objectives: Calcified coronary nodules (CN) are among the most challenging lesions for percutaneous coronary intervention, as drug-eluting stents (DES) frequently result in suboptimal expansion, malapposition, and recurrent adverse events. Although intravascular lithotripsy (IVL) provides effective plaque modification, the optimal definitive strategy remains unclear. Drug-eluting balloons (DEB) have demonstrated potential in the treatment of complex lesions in which stent implantation may be less desirable. This trial aims to compare the safety and efficacy profile of DEB vs DES after IVL in patients with CN.
Methods: We conducted a retrospective, investigator-initiated, multicenter, non-inferiority, randomized clinical trial.
Results: A total of 128 patients with de novo CN confirmed by intracoronary imaging in vessels measuring 2.5 mm to 4.0 mm in diameter will be enrolled across 10 high-volume percutaneous coronary intervention centers. After lesion preparation with IVL, patients will be randomized on a 1:1 ratio to receive a DEB or a DES. The co-primary endpoints are late lumen loss and net luminal gain at 9 ± 1 months of angiographic follow-up, both assessed by an independent core laboratory. Secondary endpoints include procedural, angiographic, and clinical outcomes, adjudicated by a blinded clinical events committee. Clinical follow-up will be conducted at 1 month, 1 year, and 2 years.
Conclusions: The DEBSCAN-IVL trial will provide the first randomized evidence comparing DEB and DES after IVL for CN.
Registered at ClinicalTrials.gov: NCT06657833.
Keywords: Calcified nodule. Intravascular lithotripsy. Drug-eluting balloons. Drug-eluting stents. Complex percutaneous coronary intervention.
RESUMEN
Introducción y objetivos: Los nódulos coronarios calcificados (NC) se encuentran entre las lesiones más desafiantes para la intervención coronaria percutánea, ya que los stents farmacoactivos (SFA) con frecuencia presentan expansión subóptima, mala aposición y eventos adversos recurrentes. La litotricia intravascular (LIV) permite una modificación eficaz de la placa, pero la estrategia definitiva óptima sigue sin estar clara. Los balones farmacoactivos (BFA) han mostrado resultados prometedores en lesiones complejas en las que la implantación de stents podría ser menos favorable. Este ensayo tiene como objetivo comparar la seguridad y la eficacia del BFA frente al SFA después de la LIV en pacientes con NC.
Métodos: Ensayo clínico prospectivo, por iniciativa del investigador, multicéntrico, de no inferioridad y aleatorizado.
Resultados: Un total de 128 pacientes con NC de novo confirmados mediante imagen intracoronaria en vasos de 2,5-4,0 mm de diámetro serán incluidos en 10 centros de intervencionismo coronario percutáneo de alto volumen. Tras la preparación de la lesión con LIV, los pacientes serán aleatorizados 1:1 para ser tratados con BFA o SFA. Los criterios de valoración coprimarios son la pérdida luminal tardía y la ganancia luminal neta en el seguimiento angiográfico a 9 ± 1 meses, evaluadas por un laboratorio central independiente. Los criterios secundarios incluyen resultados procedimentales, angiográficos y clínicos, adjudicados por un comité de eventos clínicos enmascarado. El seguimiento clínico se realizará a 1 mes, 1 año y 2 años.
Conclusiones: El ensayo DEBSCAN-IVL proporcionará la primera evidencia de comparación de BFA y SFA aleatorizados después de IVL en NC.
Registrado en ClinicalTrials.gov: NCT06657833.
Palabras clave: Nódulo calcificado. Litotricia intravascular. Balón farmacoactivo. Stent farmacoactivo. Intervención coronaria percutánea compleja.
Abreviaturas
CN: calcified coronary nodule. DEB: drug-eluting balloon. DES: drug-eluting stent. IVL: intravascular lithotripsy. OCT: optical coherence tomography. PCI: percutaneous coronary intervention.
INTRODUCTION
Calcified coronary nodules (CN) represent the most complex type of calcified lesion for percutaneous coronary intervention (PCI), as they are associated with worse angiographic and clinical outcomes after drug-eluting stent (DES) implantation.1-8
Intravascular lithotripsy (IVL) has shown favorable results in this context.9 However, stent implantation after IVL may not always be the best treatment option due to suboptimal stent expansion and severe malapposition in a non-negligible percentage of patients which, along with possible nodule protrusion through the stent struts, may be associated with an increased need for new target lesion revascularization (TLR), and a higher rate of major adverse cardiovascular events (MACE).10-12
Drug-eluting balloons (DEB) have demonstrated to be a safe and effective alternative to DES in various settings, especially in those in which stenting is associated with worse outcomes, such as small vessel disease and in-stent restenosis.13 Therefore, their use has increased exponentially in recent years and has expanded to other lesion types.14
In the specific setting of calcified lesions, there are some data on the safety and efficacy profile of DEB after an adequate plaque modification.15-19 Moreover, in this setting, DEB have shown similar clinical outcomes with favorable late lumen loss rate compared with DES.20-23
Despite the increasing use of DEB in calcified lesions, evidence on the safety and efficacy profile of CN treatment is lacking. In this setting, where the risj of suboptimal stent expansion and apposition—and the consequent likelihood of MACE— is higher,24 a leave-nothing-behind strategy using DEB following optimal plaque modification technique may be a more appealing approach.Therefore, our aim is to compare the safety and efficacy profile of the use of DEB or DES after IVL in CN within the context of a randomized controlled trial.
METHODS
Patients and study design
The DEBSCAN-IVL trial is an investigator-initiated, multicenter, open-label, prospective, randomized, controlled clinical trial including 10 high-volume centers.
Patients will be randomized to receive a DEB or a DES after optimal treatment with IVL if they meet all the inclusion criteria and have no exclusion criteria. Inclusion criteria are age ≥ 18 years with a clinical indication for PCI (presenting with chronic or acute coronary syndromes) in a CN-induced de novo severe coronary lesion (confirmed via intracoronary imaging) in vessels with a reference diameter between 2.5 mm and 4.0 mm. Patients who meet at least 1 of the following conditions will be excluded: inability to provide oral and written informed consent or unwillingness to return for systematic angiographic follow-up; pregnant or breastfeeding patients; cardiogenic shock or cardiac arrest at the time of the index procedure; inability to maintain dual antiplatelet therapy for at least 1 month; life expectancy < 1 year; index lesion located at the left main coronary artery or in an aorto-ostial location; target lesion previously treated with stents or DEB or with high thrombus burden at the time of PCI (Thrombolysis In Myocardial Infarction [TIMI] thrombus grade ≥ 3).
Patients who meet all the inclusion criteria and none of the exclusion criteria will be treated with IVL and randomized to receive final therapy with DEB or DES. Randomization will occur via a web-based system. The complete inclusion and exclusion criteria are shown in table 1, and the study flowchart in figure 1.
Table 1. Inclusion and exclusion criteria
| Inclusion criteria | Exclusion criteria |
|---|---|
Patients must meet all inclusion criteria:
|
Patients must not meet any criteria:
|
|
DEB, drug-eluting balloon; IVUS, intravascular ultrasound; OCT, optical coherence tomography; PCI, percutaneous coronary intervention; TIMI, Thrombolysis in Myocardial Infarction. |
|
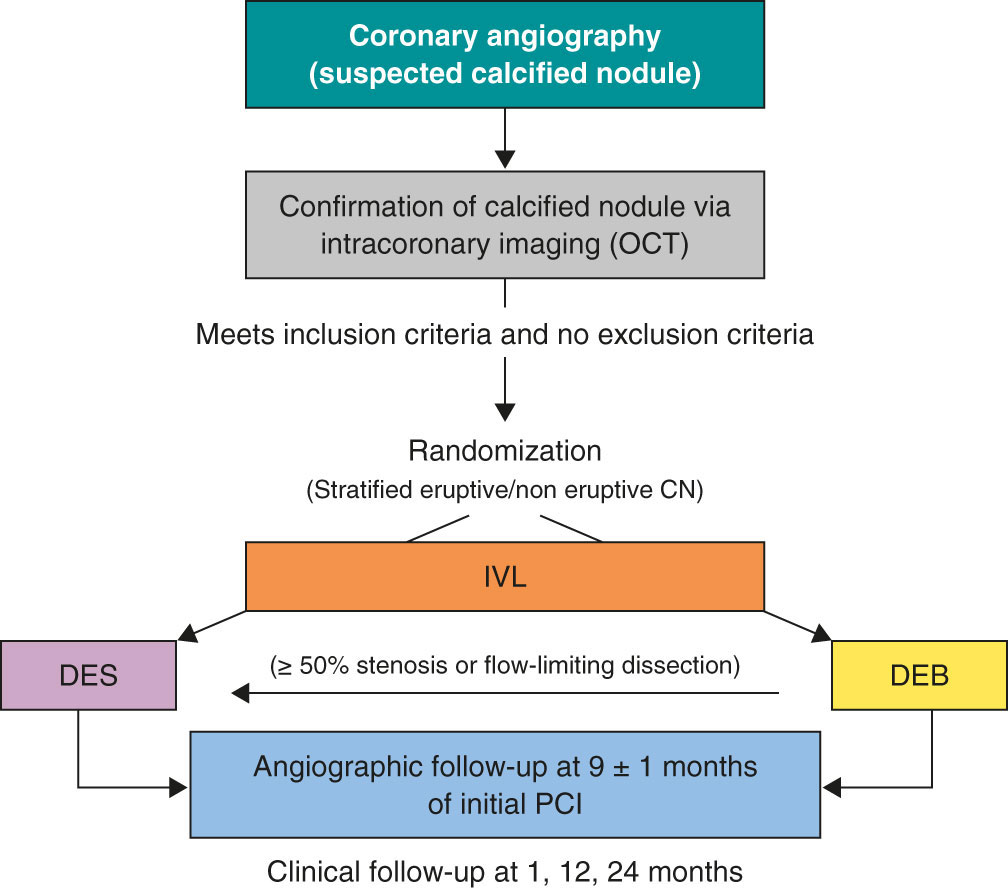
Figure 1. Central illustration. Study design flowchart. CN, calcified coronary nodule; DEB, drug-eluting balloons; DES, drug-eluting stents; IVL, intravascular lithotripsy; OCT, optical coherence tomography; PCI, percutaneous coronary intervention.
Primary and secondary endpoints
The endpoint of this study is to evaluate and compare the safety and efficacy profile of DEB or DES as final treatment strategies for CN previously modified by IVL.
Co-primary endpoints will be the late lumen loss (LLL) and net luminal gain at 9 ± 1 months of angiographic follow-up, as assessed by an independent core laboratory, with a non-inferiority hypothesis between the 2 groups. LLL is defined as the difference between postoperative and follow-up minimal lumen diameter, whereas net gain is defined as the difference between follow-up and preoperative minimal lumen diameter, according to the latest Drug Coated Balloon Academic Research Consortium Consensus Document.25
Secondary endpoints of the study will include procedural, angiographic and clinical outcomes. Procedural endpoints will include the rate of crossover between treatment groups, angiographic success (defined as final TIMI grade-3 flow and a residual final percent diameter stenosis < 30% in the DEB group or < 20% in the DES group), device success (defined as angiographic success without crossover between treatment group), procedural success (defined as angiographic success without the occurrence of severe procedural complications, including cardiac death, target vessel perioperative myocardial infarction [MI], need for new clinically driven TLR, stent thrombosis [ST], stroke, flow-limiting dissection or vessel perforation). Angiographic endpoints will include the minimal lumen diameter measured immediately after the intervention and at the time of angiographic follow-up, the residual percent diameter stenosis at both timeframes, and the rate of binary restenosis, defined as a luminal diameter reduction o≥ 50% during follow-up.25 Secondary endpoints will include procedural adverse events (such as dissection, perforation, acute vessel occlusion, slow flow or no-reflow, and intraoperative thrombosis), major hemorrhagic events (classified as Bleeding Academic Research Consortium [BARC] type ≥ 3),26 and hemodynamic instability (requiring unplanned administration of vasopressors, inotropes, or ventricular support devices), cardiac death, target lesion-related MI (TL-MI), need for TLR, and ST, and MACE (defined as a composite of cardiac death, TL-MI, and TLR). TLR and ST are defined according to the Academic Research Consortium criteria.27 MACE and its components will be assessed during the index hospitalization and at 6-month, 1-year, and 2-year follow-up visits. Detailed endpoints definitions are shown in appendix S1.
Primary outcome assessment will be conducted by a central independent core laboratory. All medical data will be anonymized and stored, and confidentiality will be protected at any time in full compliance with the current legislation. The clinical events committee (CEC) and the independent core laboratory will be blinded to the treatment group. Secondary outcomes will be assessed via centralized angiographic analysis and structured clinical follow-up, either in person or via telephone, at scheduled time points.
Devices
- – IVL: Shockwave Balloon (Shockwave Medical, United States).
- – Optical coherence tomography (OCT) or intracoronary ultrasound (IVUS) system, based on availability at each participating center.
- – DEB: paclitaxel-eluting balloon (Pantera Lux, Biotronik, Switzerland).
- – DES: new-generation zotarolimus eluting stent (Onyx Frontier, Medtronic, United States).
Procedure
When a CN is suspected on coronary angiography, intracoronary imaging—preferably OCT, with IVUS as an alternative—will be performed to confirm the diagnosis. After confirmation of a CN in the target lesion, patients will be randomized on a 1:1 ratio to receive a DEB or a DES. Randomization will be stratified to ensure a balanced distribution of eruptive and non-eruptive nodules across both treatment groups. A CN (figure 2) will be defined as a calcified segment with an accumulation of protruding nodular calcification (small calcium deposits) with disruption of the fibrous cap (eruptive CN) or an intact thick fibrous cap (non-eruptive CN).28-30
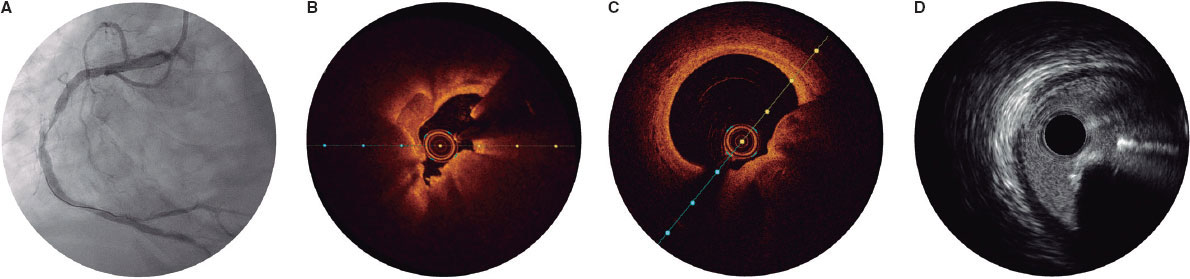
Figure 2. Calcified nodule appearance on angiography (A), optical coherence tomography (eruptive [B] and non-eruptive [C]) and intravascular ultrasound (D).
All patients will be treated with IVL, using a balloon sized 1:1 to the vessel reference diameter. A minimum of 80 pulses per lesion is recommended. If the IVL balloon cannot cross the lesion, predilation with smaller balloons is permitted. Additionally, the use of adjuvant techniques such as rotational atherectomy or excimer laser coronary atherectomy will be allowed only when deemed necessary to facilitate IVL balloon crossing. Postdilation with a non-compliant balloon after IVL is recommended before proceeding with the final assigned treatment modality.
Once optimal lesion preparation has been achieved, defined as > 80% balloon expansion in 2 orthogonal projections with a balloon sized 1:1 to the vessel, patients will receive a DEB or a DES, according to their initial randomization. If a patient randomized to the DEB group experiences a flow-limiting dissection or exhibits a percent diameter stenosis > 50%, conversion to DES implantation will be permitted at the operator’s discretion. Similarly, any crossover from DES to DEB will be documented, along with the reasons for these procedural decisions.
It is recommended that the DEB reach the target lesion within 2 minutes, as drug loss may occur during transit.13 Thus, operators need to anticipate difficulties in reaching the target lesion (proximal coronary disease or tortuosity) and ensure optimal support prior to using the DEB. If difficulties in reaching the target lesion are anticipated, the use of guide extension catheters is recommended. The recommended DEB inflation time is 60 seconds.
The PCI will be performed according to current European Society of Cardiology (ESC) guidelines, including perio- and postoperative antithrombotic management.31,32 Patients should ideally receive dual antiplatelet therapy at least 2 to 4 hours prior to the PCI to ensure optimal platelet inhibition. In cases where this is not feasible, administration of IV antiplatelet agents, such as acetylsalicylic acid with or without cangrelor, immediately before the procedure is recommended.
Intracoronary imaging with either OCT or IVUS (the same imaging modality that was initially used) is recommended at the end of the procedure.
Angiographic analysis
Quantitative coronary imaging and intracoronary analysis of baseline and follow-up angiographies will be conducted by an independent central laboratory (Barcicore, Spain). At least 2 well-selected orthogonal views—free of foreshortening and side-branch overlap—focused on the target lesion are required after intracoronary nitroglycerine administration. These views should be obtained before treatment, after the intervention, and during follow-up angiography to ensure consistent angulation and enable accurate, reproducible measurements.
Follow-up
Post-PCI antithrombotic therapy will abide by the latest ESC clinical practice guidelines, considering the individual ischemic and bleeding risk profile of each patient.31,32 Regardless of the assigned treatment group (DEB or DES), a 6-month regimen of dual antiplatelet therapy (aspirin and clopidogrel) is recommended in patients with stable coronary artery disease, and a 12-month regimen of dual antiplatelet therapy (preferably using prasugrel or ticagrelor as a P2Y12 inhibitor) in patients with acute coronary syndrome. For patients requiring chronic oral anticoagulation, the choice and duration of antithrombotic therapy will follow current guideline recommendations, with triple therapy (oral anticoagulant + aspirin + clopidogrel) limited to 1 month, whenever feasible. Electrocardiogram and troponin assessment will be performed 24 hours after the PCI. All patients will be discharged with a scheduled angiographic follow-up at 9 ± 1 months. OCT is recommended during this follow-up, especially if angiography suggests progression of coronary artery disease in the target lesion. In cases where angiography or intracoronary imaging indicates disease progression, but the percent diameter stenosis is < 90%, revascularization should be guided by ischemia and confirmed with a pressure guidewire. Clinical follow-up visits are scheduled at 12 and 24 months. Schedule of visits and data assessment throughout the study are shown in table S1.
Statistical analysis
The primary endpoint analysis will be performed by lesion and by intention-to-treat with a 1-sided Student t test with an alfa of 0.05 between the DES and the DEB group. A per-protocol analysis, including crossover cases, will also be conducted for sensitivity purposes. If the hypothesis of non-inferiority is confirmed, a superiority 2-sided analysis will be performed. Clinical endpoints will be analyzed on a per-patient basis.
Quantitative variables will be expressed as mean ± standard deviation if normally distributed, and as median with minimum and maximum values if they do not follow a normal distribution. Normality will be assessed using the Kolmogorov-Smirnov test. Qualitative variables will be described by their absolute values and frequencies, and will be expressed as absolute counts and percentages. A P < .05 will be considered statistically significant, and 95% confidence intervals (95%CI) will be reported for all main analyses. For comparisons of continuous variables between the 2 groups, the Student t test will be used if normality is confirmed, or the Mann-Whitney U test if non-parametric. For comparisons across > 2 groups, the ANOVA test or the Kruskal-Wallis test will be applied, as appropriate. Associations across categorical variables will be analyzed using the chi-square test or Fisher’s exact test when expected frequencies are small. Correlations between continuous variables will be explored using Pearson’s or Spearman’s correlation coefficient, depending on their distribution.
A multivariate analysis will be conducted using Cox proportional hazards regression with forward stepwise selection, including variables that are significantly associated with outcomes (or show a trend) in the univariate analysis. Kaplan-Meier curves will be generated for event-free survival, and differences will be assessed using the log-rank test.
Prespecified subgroup analysis
Subgroup analysis will be performed according to the following prespecified categories: type of calcified nodule (eruptive vs non-eruptive), age (< 75 vs ≥ 75 years), sex (male vs female), presence of diabetes mellitus (yes vs no), location of the calcified nodule within a true bifurcation lesion involving a side branch ≥ 2.5 mm (yes vs no), and clinical presentation (acute coronary syndrome vs chronic coronary syndrome). In addition, a prespecified OCT subgroup analysis will be performed in patients with available OCT imaging at both the end of the procedure and follow, including assessments of minimal lumen area (or minimal stent area in stented segments) and minimal lumen diameter.
Sample size calculation
The hypothesis is that DEB-PCI for CN is not inferior to state-of-the-art DES-PCI in terms of LLL and net luminal gain at the lesion. The sample size calculation was based on an expected LLL of 0.20 mm in the DES group, with a non-inferiority margin (delta) of 0.30 mm, a significance level (alpha) of 5%, and a statistical power of 80%. The estimate of LLL in the control group was derived from previous studies evaluating the same DES platform.33-35 Assuming a 20% attrition rate for angiographic follow-up, 64 patients per group (128 patients in total) will be required to provide adequate statistical power. The study is not powered for clinical endpoints, which will be considered exploratory and hypothesis-generating.
Organization and ethical concerns
The study protocol has been approved by the local ethics committees of all participant centers. Written informed consent will be obtained from all patients prior to enrollment. The DEBSCAN-IVL trial is an investigator-initiated study conducted in full compliance with Good Clinical Practice guidelines applicable to interventional and epidemiological research. The rights, safety, and well-being of all participants will be protected full compliance with the principles set forth in the Declaration of Helsinki, applicable EU legislation, and local legal requirements. Participant data will be handled confidentially and anonymously. The trial is registered at ClinicalTrials.gov (NCT06657833). The sponsor of the study is Fundación EPIC. The study is supported by unrestricted research grants from Fundación EPIC, Shockwave Medical, Biotronik, and Medtronic.
The steering committee serves as the primary decision-making body of the trial and bears full responsibility for its scientific and clinical conduct. A clinical events committee (CEC), composed of independent interventional cardiologists not participating in the study and blinded to treatment allocation, will adjudicate all clinical events and endpoints. The CEC will operate according to pre-specified definitions outlined in the study protocol and will remain blinded to the overall trial outcomes.
DISCUSSION
CN represent the most complex type of calcified lesion for PCI, as they are associated with the worst angiographic and clinical outcomes after DES implantation.1-8 Three main factors may contribute to these unfavorable results: the nature of the nodule per se, the plaque modification technique used, and the final revascularization strategy (DES or DEB). Although our understanding of the origin and behavior of calcified nodules has grown, it remains unclear which lesions are likely to respond favorably to PCI, and which are not. Eruptive CN, for instance, may be more amenable to initial modification, yet paradoxically, they have also been associated with higher rates of adverse clinical events during follow-up.29,36
Regarding plaque modification techniques, current evidence is limited. Rotational atherectomy (RA), while commonly used, is constrained by wire bias and frequently requires large burr sizes.2 Although orbital atherectomy might overcome some of these limitations, randomized data comparing it with other advanced plaque modification techniques are lacking.37 Balloon-based techniques, in contrast, may fail to cross severely stenotic nodular lesions but have the advantage of avoiding the wire bias inherent to atherectomy.
However, conventional or scoring/cutting balloons often prove insufficient to fully modify the depth of nodular calcium, and very high-pressure special balloons carry the risk of overstretching the usually normal opposite vessel wall causing perforation. In this context, IVL has emerged as a promising alternative, offering the most robust evidence to date for nodular plaque modification.29,38
Traditionally, stent implantation has been the standard definitive treatment for CN.23 However, stenting in nodular lesions frequently leads to suboptimal expansion and incomplete apposition, particularly at the shoulders of the nodule. Moreover, In these patients, TLR is often driven not by classic in-stent restenosis, but by late protrusion of the calcified nodule through the stent struts.10,11,39 These limitations have generated interest in a “leave nothing behind” strategy after effective plaque modification.
DEB have demonstrated to be safe and effective in various settings, particularly small vessel disease and in-stent restenosis, where DES implantation may be less favorable.13 Therefore, their use has grown significantly in recent years.14 In the context of calcified lesions, there are concerns that adequate drug-uptake may be compromised, but preliminary evidence suggests DEB may offer good outcomes after adequate plaque preparation.15-17 For instance, Ito et al.18 evaluated a total of 81 patients with de novo lesions treated with DEB, including 46 with calcified lesions. While LLL and restenosis appeared slightly higher in the calcified group, these differences were not statistically significant and did not translate into worse clinical outcomes at 2 years. Notably, 82% of these lesions were pre-treated with RA. Similarly, Nagai et al. reported a TLR rate of 16.3% in 190 severely calcified lesions treated with RA followed by DEB.19 Rissanen et al. found MACE rates of 14% and 20% at 12 and 24 months, respectively, in 82 complex de novo calcified lesions treated with DEB after RA and balloon predilation, with very low rates of clinically driven TLR.20 Furthermore, favorable findings have been reported by Shiraishi et al., including a subset of calcified nodules.16
Comparative studies have further explored DEB vs DES in calcified lesions. Ueno et al.21 conducted a single-center cohort study comparing the clinical outcomes of 166 severe calcified lesions treated with either DEB or DES after RA at a median follow-up of 3 years. The TLR rates were similar across the groups (15.6% vs 16.3%; P = .99), while LLL was significantly lower in the DEB group (0.09 mm vs 0.52 mm; P =.009). Iwasaki et al.22 compared 194 patients with de novo calcified lesions in non-small vessels the RA + DEB vs RA + DES strategies. There were no significant differences at 1 year in terms of MACE, cardiac death, myocardial infarction, TLR or hemorrhage.
Despite this data on the performance of DEB in calcified lesions, evidence on the safety and efficacy profile in the CN setting is lacking. However, given the high likelihood of suboptimal stent expansion and malapposition in this setting, which may lead to increased MACE risk,24 a metal-free strategy using DEB following optimal plaque modification seems to be an attractive and feasible approach.
Intracoronary imaging-guided PCI has been consistently associated with improved procedural outcomes and a reduction in major adverse cardiovascular events, including mortality, particularly in complex lesions.40 Intracoronary imaging plays a pivotal role in this context. Compared with conventional angiography, it provides a far more accurate assessment of coronary disease severity and plaque morphology.1 This is particularly relevant in calcified and complex lesions, where procedural planning and outcomes are significantly impacted by the detailed anatomical insights obtained. OCT, in particular, offers superior spatial resolution compared to IVUS, allowing for precise quantification of the calcium burden.28,41
In the case of CN, OCT enables accurate assessment of the plaque substrate and procedural results, including stent expansion and apposition, or in DEB-treated lesions, the extent of plaque modification.
The DEBSCAN-IVL trial will be comparing the safety and efficacy profile of DEB vs DES after lesion preparation with IVL in patients with CN, assessing both angiographic and clinical outcomes. Moreover, the trial will provide valuable information on the underlying plaque morphology and the response to different PCI strategies following the systematic use of intracoronary imaging. The central hypothesis of the study is that a DEB strategy, after IVL-based plaque modification in calcified nodules, is not inferior to DES implantation in terms of LLL and net gain, while potentially reducing the risk of long-term adverse events through improved biocompatibility and vessel healing. In addition, the analysis will be stratified according to nodule morphology, specifically differentiating eruptive vs non-eruptive CN, 2 entities that are thought to have distinct biological behavior and potentially different response to plaque modification and PCI.6,7,29,36 This stratified analysis may provide novel insights into the prognostic and therapeutic implications of nodule subtype and guide future individualized interventional strategies.
CONCLUSIONS
The DEBSCAN-IVL trial is an investigator-initiated, multicenter, open-label, prospective, randomized, controlled clinical trial designed to compare the safety and efficacy profile of the use of DEB or DES after IVL in CN. The co-primary endpoints are LLL and net gain at 9 ± 1 months of angiographic follow-up. The findings are expected to inform clinical decision-making and support a more individualized approach on the management of this specific type of calcified coronary disease.
DATA AVAILABILITY
This manuscript refers to the protocol of a study, therefore there is not available data related to this manuscript.
FUNDING
The DEBSCAN-IVL study was supported by non-restricted grants from Shockwave, Biotronik and Medtronic.
ETHICAL CONSIDERATIONS
The study was conducted in full compliance with the principles set forth in the Declaration of Helsinki. Institutional Ethics Committee approval was obtained, and all participants gave their written informed consent prior to enrollment. The confidentiality and anonymity of participants were strictly preserved throughout the study. Sex and gender considerations were addressed following the recommendations of the SAGER guidelines to ensure accurate and equitable reporting.
STATEMENT ON THE USE OF ARTIFICIAL INTELLIGENCE
Artificial intelligence assisted technologies were used exclusively to support language editing and improvement of style. No artificial intelligence tools were employed to generate, analyze, or interpret the data. The authors take full responsibility for the integrity, accuracy, and originality of the manuscript content.
AUTHORS’ CONTRIBUTIONS
A. Jurado-Román, M. Basile and R. Moreno drafted the manuscript. The remaining authors performed a critical review, and all authors approved the final version for publication.
CONFLICTS OF INTEREST
A. Jurado-Román is a proctor for Abbott, Boston Scientific, World Medica, and Philips; has received consulting fees from Boston Scientific and Philips; and has received speaker fees from Abbott, Boston Scientific, Shockwave Medical, Philips, and World Medica. J.M. Montero-Cabezas received a research grant from Shockwave Medical and speaker fees from Abiomed, Boston Scientific, and Penumbra Inc. A. Pérez de Prado reports receiving institutional research grants from Abbott and Shockwave Medical and speaker honoraria and consulting fees from iVascular, Boston Scientific, Terumo, B. Braun, and Abbott Vascular. I.J. Amat-Santos is proctor for Boston Scientific. A. Pérez de Prado, F. Alfonso and R. Moreno are associate editors of REC: Interventional Cardiology; the journal’s editorial procedure to ensure impartial handling of the manuscript has been followed. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose.
WHAT IS KNOWN ABOUT THE TOPIC?
- CN are among the most complex calcified lesions for PCI, as DES often result in suboptimal expansion, malapposition, and long-term adverse events. IVL is an effective and safe technique for modifying nodular calcium. DEB have proven effective in complex lesions such as small vessel disease and in-stent restenosis, suggesting potential utility where stent implantation might be suboptimal. However, robust evidence on the safety and efficacy of DEB specifically for CN after IVL is currently lacking.
WHAT DOES THIS STUDY ADD?
- The DEBSCAN-IVL trial will be the first randomized study to compare DEB and DES after IVL in patients with CN. It will evaluate angiographic endpoints such as late lumen loss and net luminal gain, as well as procedural and clinical outcomes. The study is expected to provide crucial insights into whether a “leave-nothing-behind“ approach with DEB can achieve comparable efficacy to DES while potentially improving vessel healing and reducing longterm complications in this challenging patient population.
REFERENCES
1. Jurado-Román A, Gómez-Menchero A, Gonzalo N, et al. Plaque modification techniques to treat calcified coronary lesions. Position paper from the ACI-SEC. REC Interv Cardiol. 2023;5:46-61.
2. Morofuji T, Kuramitsu S, Shinozaki T, et al. Clinical impact of calcified nodule in patients with heavily calcified lesions requiring rotational atherectomy. Catheter Cardiovasc Interv. 2021;97:10-19.
3. Lee T, Mintz GS, Matsumura M, et al. Prevalence, Predictors, and Clinical Presentation of a Calcified Nodule as Assessed by Optical Coherence Tomography. JACC Cardiovasc Imaging. 2017;10:883-891.
4. Lei F, Yin Y, Liu X, et al. Clinical Outcomes of Different Calcified Culprit Plaques in Patients with Acute Coronary Syndrome. J Clin Med. 2022;11:4018.
5. Mintz GS. Intravascular Imaging of Coronary Calcification and Its Clinical Implications. JACC Cardiovasc Imaging. 2015;8:461-471.
6. Torii S, Sato Y, Otsuka F, et al. Eruptive Calcified Nodules as a Potential Mechanism of Acute Coronary Thrombosis and Sudden Death. J Am Coll Cardiol. 2021;77:1599-1611.
7. Sato T, Matsumura M, Yamamoto K, et al. Impact of Eruptive vs Noneruptive Calcified Nodule Morphology on Acute and Long-Term Outcomes After Stenting. JACC Cardiovasc Interv. 2023;16:1024-1035.
8. Nagata T, Minami Y, Katsura A, et al. Optical coherence tomography factors for adverse events in patients with severe coronary calcification. Int J Cardiol. 2023;376:28-34.
9. Ali ZA, Nef H, Escaned J, et al. Safety and Effectiveness of Coronary Intravascular Lithotripsy for Treatment of Severely Calcified Coronary Stenoses:The Disrupt CAD II Study. Circ Cardiovasc Interv. 2019;12:e008434.
10. Kaihara T, Higuma T, Kotoku N, et al. Calcified Nodule Protruding Into the Lumen Through Stent Struts:An In Vivo OCT Analysis. Cardiovasc Revasc Med. 2020;21:116-118.
11. Kawai K, Akahori H, Imanaka T, et al. Coronary restenosis of in-stent protruding bump with rapid progression:Optical frequency domain imaging and angioscopic observation. J Cardiol Cases. 2019;19:12-14.
12. Isodono K, Fujii K, Fujimoto T, et al. The frequency and clinical characteristics of in-stent restenosis due to calcified nodule development after coronary stent implantation. Int J Cardiovasc Imaging. 2021;37:15-23.
13. Jeger RV, Eccleshall S, Wan Ahmad WA, et al. Drug-Coated Balloons for Coronary Artery Disease. JACC Cardiovasc Interv. 2020;13:1391-1402.
14. Jurado-Román A, Freixa X, Cid B, et al. Spanish cardiac catheterization and coronary intervention registry. 32nd official report of the Interventional Cardiology Association of the Spanish Society of Cardiology (1990-2022). Rev Esp Cardiol. 2023;76:1021-1031.
15. Basavarajaiah S, Loku Waduge BH, Watkin R, Athukorala S. Is a high calcific burden an indication, or a contraindication for Drug Coated Balloon?Rev Cardiovasc Med. 2021;22:1087-1093.
16. Shiraishi J, Kataoka E, Ozawa T, et al. Angiographic and Clinical Outcomes After Stent-less Coronary Intervention Using Rotational Atherectomy and Drug-Coated Balloon in Patients with De Novo Lesions. Cardiovasc Revasc Med. 2020;21:647-653.
17. Ho HH, Lee JH, Khoo DZL, Hpone KKS, Li KFC. Shockwave intravascular lithotripsy and drug-coated balloon angioplasty in calcified coronary arteries:preliminary experience in two cases. J Geriatr Cardiol. 2021;18:689-691.
18. Ito R, Ueno K, Yoshida T, et al. Outcomes after drug?coated balloon treatment for patients with calcified coronary lesions. J Intervent Cardiol. 2018;31:436-441.
19. Nagai T, Mizobuchi M, Funatsu A, Kobayashi T, Nakamura S. Acute and mid-term outcomes of drug-coated balloon following rotational atherectomy. Cardiovasc Interv Ther. 2020;35:242-249.
20. Rissanen TT, Uskela S, Siljander A, et al. Percutaneous Coronary Intervention of Complex Calcified Lesions With Drug?Coated Balloon After Rotational Atherectomy. J Intervent Cardiol. 2017;30:139-146.
21. Ueno K, Morita N, Kojima Y, et al. Safety and Long-Term Efficacy of Drug-Coated Balloon Angioplasty following Rotational Atherectomy for Severely Calcified Coronary Lesions Compared with New Generation Drug-Eluting Stents. J Intervent Cardiol. 2019;2019:1-10.
22. Iwasaki Y, Koike J, Ko T, et al. Comparison of drug-eluting stents vs drug-coated balloon after rotational atherectomy for severely calcified lesions of nonsmall vessels. Heart Vessels. 2021;36:189-199.
23. Rivero-Santana B, Jurado-Roman A, Galeote G, et al. Drug-eluting balloons in Calcified Coronary Lesions:A Meta-Analysis of Clinical and Angiographic Outcomes. J Clin Med. 2024;13:2779.
24. Muramatsu T, Kozuma K, Tanabe K, et al. Clinical expert consensus document on drug-coated balloon for coronary artery disease from the Japanese Association of Cardiovascular Intervention and Therapeutics. Cardiovasc Interv Ther. 2023;38:166-176.
25. Fezzi S, Scheller B, Cortese B, et al. Definitions and standardized endpoints for the use of drug-coated balloon in coronary artery disease:consensus document of the Drug Coated Balloon Academic Research Consortium. EuroIntervention. 2025;21:e1116-e1136.
26. Mehran R, Rao SV, Bhatt DL, et al. Standardized Bleeding Definitions for Cardiovascular Clinical Trials:A Consensus Report From the Bleeding Academic Research Consortium. Circulation. 2011;123:2736-2747.
27. Garcia-Garcia HM, McFadden EP, Farb A, et al. Standardized End Point Definitions for Coronary Intervention Trials:The Academic Research Consortium-2 Consensus Document. Circulation. 2018;137:2635-2650.
28. Johnson TW, Räber L, Di Mario C, et al. Clinical use of intracoronary imaging. Part 2:acute coronary syndromes, ambiguous coronary angiography findings, and guiding interventional decision-making:an expert consensus document of the European Association of Percutaneous Cardiovascular Interventions. Eur Heart J. 2019;40:2566-2584.
29. Fernández-Cordón C, Brilakis ES, García-Gómez M, et al. Calcified nodules in the coronary arteries:systematic review on incidence and percutaneous coronary intervention outcomes. Rev Esp Cardiol. 2025;78:977-991.
30. Guagliumi G, Pellegrini D, Maehara A, Mintz GS. All calcified nodules are made equal and require the same approach:pros and cons. EuroIntervention. 2023;19:e110-e112.
31. Byrne RA, Rossello X, Coughlan JJ, et al. 2023 ESC Guidelines for the management of acute coronary syndromes:Developed by the task force on the management of acute coronary syndromes of the European Society of Cardiology (ESC). Eur Heart J. 2023;44:3720-3826.
32. Vrints C, Andreotti F, Koskinas KC, et al. 2024 ESC Guidelines for the management of chronic coronary syndromes:Developed by the task force for the management of chronic coronary syndromes of the European Society of Cardiology (ESC) Endorsed by the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J. 2024;45:3415-3537.
33. Latib A, Colombo A, Castriota F, et al. A Randomized Multicenter Study Comparing a Paclitaxel Drug-eluting balloon With a Paclitaxel-Eluting Stent in Small Coronary Vessels. J Am Coll Cardiol. 2012;60:2473-2480.
34. Cannon LA, Simon DI, Kereiakes D, et al. The XIENCE nanoTM everolimus eluting coronary stent system for the treatment of small coronary arteries:The SPIRIT small vessel trial. Catheter Cardiovasc Interv. 2012;80:546-553.
35. Cortese B, Di Palma G, Guimaraes MG, et al. Drug-Coated Balloon Versus Drug-Eluting Stent for Small Coronary Vessel Disease. JACC Cardiovasc Interv. 2020;13:2840-2849.
36. Prati F, Gatto L, Fabbiocchi F, et al. Clinical outcomes of calcified nodules detected by optical coherence tomography:a sub-analysis of the CLIMA study. EuroIntervention. 2020;16:380-386.
37. Shin D, Dakroub A, Singh M, et al. Debulking Effect of Orbital Atherectomy for Calcified Nodule Assessed by Optical Coherence Tomography. Circ Cardiovasc Interv. 2024;17.
38. Ali ZA, Kereiakes D, Hill J, et al. Safety and Effectiveness of Coronary Intravascular Lithotripsy for Treatment of Calcified Nodules. JACC Cardiovasc Interv. 2023;16(9):1122-1124.
39. Madhavan MV, Alsaloum M, Maehara A, et al. Recurrent Calcified Nodule Protrusion Through Stent Struts After Percutaneous Coronary Intervention of the RCA. JACC Cardiovasc Interv. 2023;16:2463-2465.
40. Stone GW, Christiansen EH, Ali ZA, et al. Intravascular imaging-guided coronary drug-eluting stent implantation:an updated network meta-analysis. Lancet. 2024;403:824-837.
41. Amabile N, RangéG, Landolff Q, et al. OCT vs Angiography for Guidance of Percutaneous Coronary Intervention of Calcified Lesions:The CALIPSO Randomized Clinical Trial. JAMA Cardiol. 2025;10:666.
ABSTRACT
Introduction and objectives: Thrombus removal in patients with ST-segment elevation myocardial infarction (STEMI) undergoing percutaneous coronary intervention (PCI) can be challenging in the presence of a large thrombus burden. Excimer laser coronary angioplasty (ELCA) is an adjuvant device capable of vaporizing thrombus. This study aimed to evaluate the safety and efficacy profile of ELCA in PCI.
Methods: Patients with STEMI undergoing PCI with concomitant use of ELCA for thrombus removal were retrospectively identified at our center. Data were collected on the device efficacy and its contribution to overall procedural success. Additionally, ELCA-related complications and major adverse cardiovascular events were recorded at a 2-year follow-up.
Results: ELCA was used in 130 STEMI patients, 124 (95.4%) of whom had a large thrombus burden. TIMI grade flow improved significantly after ELCA: before laser application, TIMI grade-0 flow was reported in 79 (60.8%) cases and TIMI grade-1 flow in 32 (24.6%) cases. After ELCA, TIMI grade-2 and 3 flows were achieved in 45 (34.6%) and 66 (50.8%) cases, respectively (P < .001). Technical and procedural success were achieved in 128 (98.5%) and 124 (95.4%) cases, respectively. The complications included 1 death at the cath lab (0.8%), 1 coronary perforation (0.8%), and 3 distal embolizations (2.3%). At the 2-years follow-up, major adverse cardiovascular events occurred in 18.3% of the population.
Conclusions: In the context of STEMI, ELCA seems to be an effective device for thrombus dissolution, with adequate technical and procedural success rates. In the present cohort, ELCA use was associated with a low complication rate and favorable long-term outcomes.
Keywords: Acute coronary syndrome. Thrombectomy. Excimer laser coronary angioplasty.
RESUMEN
Introducción y objetivos: La eliminación de trombos durante la intervención coronaria percutánea primaria (ICPp) en el infarto agudo de miocardio con elevación del segmento ST (IAMCEST) es un desafío en presencia de una carga trombótica elevada. La angioplastia coronaria con láser de excímeros (ELCA) es una técnica complementaria que permite vaporizar el trombo. Este estudio evaluó la eficacia y la seguridad de la ELCA en el contexto de la ICPp.
Métodos: Análisis retrospectivo unicéntrico de pacientes con IAMCEST sometidos a ICPp con ELCA. Se evaluaron la eficacia en la disolución del trombo, la mejoría del flujo, el éxito del procedimiento, las complicaciones asociadas y los acontecimientos cardiovasculares adversos mayores durante un seguimiento de 2 años.
Resultados: Se realizó ELCA en 130 pacientes con IAMCEST, de los cuales 124 (95,4%) tenían carga trombótica elevada. El flujo TIMI mejoró significativamente tras la ELCA: previamente era 0 en 79 casos (60,8%) y 1 en 32 casos (24,6%), y se lograron flujos TIMI 2 y 3 en 45 casos (34,6%) y 66 casos (50,8%), respectivamente (p < 0,001). Las tasas de éxito técnico y del procedimiento fueron del 98,5% y el 95,4%, respectivamente. Las complicaciones incluyeron 1 muerte intraprocedimiento (0,8%), 1 perforación coronaria (0,8%) y 3 embolizaciones distales (2,3%). A los 2 años, la tasa de acontecimientos cardiovasculares adversos mayores fue del 18,3%.
Conclusiones: La ELCA parece ser una técnica eficaz y segura en el IAMCEST para la disolución del trombo, con altas tasas de éxito técnico y procedimental, baja incidencia de complicaciones y resultados favorables a largo plazo.
Palabras clave: Síndrome coronario agudo. Trombectomía. Angioplastia coronaria con láser de excímeros.
Abbreviations
ELCA: excimer laser coronary angioplasty. LTB: large thrombus burden. MACE: major adverse cardiovascular events. PCI: percutaneous coronary intervention. STEMI: ST-segment elevation myocardial infarction. TIMI: Thrombolysis in Myocardial Infarction.
INTRODUCTION
In patients with ST-segment elevation myocardial infarction (STEMI), percutaneous coronary intervention (PCI) is the preferred reperfusion strategy, as long as it can be performed within 120 minutes of the electrocardiogram-based diagnosis.1 Many patients with STEMI present with thrombotic occlusion of the infarct-related artery. Therefore, the use of devices aimed at reducing thrombus burden is a reasonable consideration to minimize distal embolization and no-reflow. Persistent no-reflow in patients with STEMI undergoing PCI is associated with the worst in-hospital outcomes and increased long-term mortality.2
While early studies on manual thrombus aspiration suggested benefits in terms of improved myocardial blush grades and ST-segment elevation resolution,3 larger trials comparing manual thrombus aspiration with PCI alone showed no significant reduction in cardiovascular death, recurrent myocardial infarction, cardiogenic shock, or a New York Heart Association FC IV heart failure within 180 days.4 Consequently, routine aspiration thrombectomy is no longer recommended in patients with STEMI.5
Thrombus removal, particularly when dealing with a large thrombus burden (LTB) in the context of STEMI, remains a critical and sometimes challenging aspect of PCI. Excimer laser coronary angioplasty (ELCA Coronary Laser Atherectomy Catheter, Koninklijke Philips N.V., The Netherlands) is a well-established adjuvant therapy for coronary interventions. ELCA uses xenon-chloride gas as the lasing medium to produce UV light energy, which is delivered to the target site through an optical fiber. This energy has the ability to ablate inorganic material through photochemical, photothermal, and photomechanical mechanisms.6,7 The microparticles released during laser ablation measure < 10 µm and are absorbed by the reticuloendothelial system, theoretically reducing the risk of microvasculature obstruction.8 These unique characteristics of ELCA have facilitated its use as an adjuvant therapy in patients with STEMI to ablate and remove thrombus.
Although ELCA is part of the therapeutic armamentarium in some PCI-capable centers, literature data is limited on its safety and efficacy profile in this specific scenario. The aim of this study was to evaluate the contribution of ELCA, focusing on its safety and efficacy profile as an adjuvant therapy in patients with STEMI undergoing PCI in our center.
METHODS
Data from all patients undergoing PCI with the simultaneous use of ELCA as an adjuvant technique were retrospectively recorded in a dedicated database after each procedure, starting from the introduction of the device in our center. ELCA procedures were performed by 5 interventional cardiologists with dedicated training in the use of the device.
This study was approved by Parque Sanitario Pere Virgili ethics committee (Barcelona, Spain) (reference No.: CEIM 003/2025). For the purposes of this study, we selected the subgroup of patients with STEMI who underwent PCI in which ELCA was used to facilitate thrombus removal.
Thrombus burden was assessed using the thrombus grading classification9 as defined by the Thrombolysis in Myocardial Infarction (TIMI) study group, ranging from 0 to 5. A LTB was defined as a thrombus score ≥ 3. According to our internal protocol, ELCA was considered in STEMI patients in the presence of angiographic evidence of LTB, defined as TIMI thrombus grade ≥ 3, particularly if TIMI grade-0–1 flow or, poor visualization of the distal vessel, or as a bailout strategy after unsuccessful manual thrombectomy. Clinical variables were meticulously refined, and follow-up details were obtained through a thorough review of the patients’ health records. Following coronary angiography and successful guidewire crossing of the culprit lesion, ELCA was left at the operator’s discretion. It was used either as a primary device for thrombus removal or as a bailout strategy when manual thrombus aspiration did not improve TIMI grade flow. The selection of catheter size was mainly based on the target vessel diameter and on the characteristics of the vessel and the lesion; a 0.9 mm ELCA catheter is usually used in tortuous anatomies due to its better navigability and in small-caliber vessels, whereas a 1.4 mm catheter is used in selected cases involving larger proximal vessels with straight segments. Catheter size (0.9 mm or 1.4 mm) was selected based on vessel diameter and lesion characteristics. Laser fluence (45-60 mJ/mm²) and pulse repetition rate (25-40 Hz) were chosen as per manufacturer’s recommendations.
Before laser application, the target vessel was flushed with saline solution to prevent interaction between the laser and blood or contrast medium. In all cases, continuous saline infusion was administered during laser delivery to avoid coronary artery wall heating. Laser energy was delivered using an ‘on-off’ technique, consisting of 10-s laser activation cycles interspersed with 5-s pauses. The laser catheter was advanced at a rate of approximately 1 mm/s over a 0.014-in coronary guidewire through the target lesion, following the manufacturer’s recommendations.7,10 After 2–3 laser catheter passes, a follow-up coronary angiography was performed to evaluate the efficacy of laser application and assess the feasibility of stent implantation. TIMI grade flow was recorded after the ELCA procedure (Post-ELCA TIMI grade flow) and once the PCI would have been completed (final TIMI grade flow). Technical success was defined as the ability to advance the laser catheter through the entire target lesion and deliver laser energy successfully. Procedural success was defined as achieving a final TIMI grade ≥ 2 flow without any major cath lab-related complications, such as death, coronary perforation, or emergency bypass surgery after PCI completion. All procedural complications, including death, coronary perforation,11 emergency bypass surgery, distal embolization, ventricular arrhythmia, and no-reflow were carefully documented and reported. Follow-up was conducted via retrospective review of health records, and major adverse cardiovascular events (MACE) defined as a composite endpoint of all-cause mortality, new myocardial infarction, and target lesion revascularization were recorded at the follow-up.
Statistical analysis
Continuous variables are expressed as mean ± standard deviation for normally distributed data or as the median (interquartile range) for non-normally distributed data. Inter-group comparisons were performed using an unpaired Student’s t-test for normally distributed variables and the Mann–Whitney U test for non-normally distributed variables. Categorical variables are expressed as counts and percentages and were analyzed using the chi-square test or Fisher’s exact test, as appropriate.
The composite endpoint of MACE was analyzed as time-to-event data at the follow-up. Kaplan–Meier survival analysis was performed to estimate the event-free survival rates. All statistical analyses were conducted using SPSS Statistics (version 23.0, IBM Corp., United States). A 2-tailed P value < .05 was considered statistically significant.
RESULTS
Between July 2015 and August 2024, a total of 130 PCI s were performed in patients with STEMI using ELCA as an adjuvant therapy for thrombus removal. The patients’ mean age was 61.8 ± 11.7 years, with 18 (13.8%) being women and 18 (13.8%) diagnosed with diabetes mellitus. ELCA was employed as the primary device for thrombus dissolution in 66 cases (50.8%) and as a bailout strategy in 64 cases (49.2%). Within the bailout group, manual thrombus aspiration was performed in 47 cases (36.2%), balloon dilation in 6 cases (4.6%), and thrombus debulking using the dotter effect in 11 cases (8.5%).
In the overall cohort, 124 patients (95.4%) presented with culprit lesions with a LTB. Before laser energy application, TIMI grade-0 flow was reported in 79 (60.8%) cases TIMI grade-1 flow in 32 (24.6%). After ELCA, TIMI grade-2 and 3 flows were achieved in 45 (34.6%) and 66 (50.8%) cases, respectively; P < .001 (figure 1).

Figure 1. TIMI grade flow distribution before and after ELCA application. Stacked bar graph showing the distribution of TIMI grade 0-3 flows at 3 different time points: initial angiography, post-ELCA, and final angiographic result after PCI. A marked improvement in coronary flow is observed following ELCA, with a progressive increase in TIMI grade-3 flow from 6.2% to 74.6%. ELCA, excimer laser coronary angioplasty; TIMI, Thrombolysis in Myocardial Infarction.
Technical success was achieved in 128 (98.5%) cases, and procedural success in 124 (95.4%) (table 1). Procedural success was significantly higher when ELCA was used as the initial strategy vs when it was used as the bailout strategy (100% vs 90.6%; P = .013). However, procedural time was significantly longer in the bailout vs the initial strategy group (69.81 vs 48.50 min, respectively) (table 2).
Table 1. Baseline characteristics of patients
| Variable (n = 130) | Value |
|---|---|
| Age, yr | 61.8 ± 11.7 |
| Female | 18 (13.8) |
| Hypertension | 59 (45,4%) |
| Hypercholesterolemia | 57 (43,8%) |
| Tobacco use | 78 (60%) |
| Diabetes mellitus | 18 (13.8) |
| Killip classification | |
| I | 98 (75.4) |
| II | 18 (13.8) |
| III | 3 (2.3) |
| IV | 11 (8.5) |
| Radial access | 118 (90,7%) |
| Femoral access | 12 (9,3%) |
| Lesion localization | |
| LMCA | 3 (2,3%) |
| LAD | 55 (42,3%) |
| LCX | 8 (6,2%) |
| RCA | 64 (49,2 %) |
| Primary device | 66 (50.8) |
| Bailout strategy | 64 (49.2) |
| Large thrombus burden | 124 (95.4) |
| Laser catheter size, Fr | |
| 0.9 | 114 (87.7) |
| 1.4 | 16 (12.3%) |
| Procedural time, min | 60 (43–86) |
| Fluoroscopy time, min | 22.2 ±12.2 |
| Laser frequency, Hz | 31 ± 10.4 |
| Laser fluency, mJ/mm2 | 46.5 ± 9.17 |
| Laser delivery time, s | 125.9 ± 83.4 |
| Technical success | 128 (98.5) |
| Procedural success | 124 (95.4) |
|
LAD: left anterior descending coronary artery; LCX: left circumflex artery; LMCA: left main coronary artery; RCA: right coronary artery. Categorical data are presented as absolute value and percentage, n (%); and continuous variables as mean ± standard deviation or first and third quartiles. |
|
Table 2. Difference in variables between the initial and bailout strategy groups
| Variable | ELCA as the initial strategy (n = 66) | ELCA as the bailout strategy (n = 64) | P-value |
|---|---|---|---|
| Complications | 8 (12.1%) | 3 (4.7%) | .100 |
| Large thrombus burden | 64 (97%) | 60 (93.8%) | .440 |
| Technical success | 65 (98.5%) | 63 (98.4%) | 1.000 |
| Procedural success | 66 (100%) | 58 (90.6%) | .013 |
| Procedural time, median | 48.50 (38.83–66.61) | 69.81 (55.36–101) | < .001 |
|
ELCA, excimer laser coronary angioplasty. Categorical data are presented as absolute value and percentage, n (%); and continuous variables as mean ± standard deviation or first and third quartiles. |
|||
One case of type IV coronary perforation, according to the modified Ellis classification, occurred in an octogenarian patient with an ecstatic and tortuous right coronary artery. Perforation sealing was achieved with the implantation of a covered stent. One cath lab-related death occurred in a patient with an uncrossable mid-segment of a left anterior descending coronary artery lesion and initial TIMI grade-3 flow. Following balloon dilation and partial advancement of the laser probe, complete vessel occlusion and suspected left main coronary artery dissection resulted in cardiac arrest and cath lab-related death.
Other procedural complications included distal embolization in 3 (2.3%) cases and slow flow or no-reflow in 4 (3.1%). Among the slow/no-reflow cases, 1 occurred after laser application, and 3 following stent implantation and/or post-dilation. All were successfully managed with optimal medical therapy, achieving final TIMI grade-2 flow. One episode of ventricular arrhythmia occurred during saline washout of the target vessel, requiring electrical cardioversion. Additionally, 1 case of stent thrombosis (0.8%) occurred intraoperatively (figure 2).
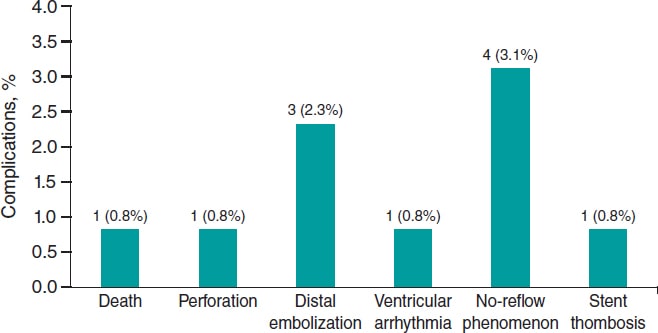
Figure 2. ELCA-related procedural complications. Bar chart showing the frequency and percentage of major complications during or immediately after ELCA. The most common was no-reflow (3.1%), followed by distal embolization (2.3%). Other events (death, perforation, ventricular arrhythmia, and stent thrombosis) were rare (0.8% each). ELCA, excimer laser coronary angioplasty.
Long-term follow-up data were missing for 6 patients (4.6%). At the 2-year follow-up, the event-free rate for combined MACE was 0.80 (95%CI, 0.73–0.88) as determined by the Kaplan–Meier estimator (table 3 and figure 3).
Table 3. List of adverse clinical events
| Patient No. | Event | Date |
|---|---|---|
| 6 | Death | 1 |
| 13 | Death | 493 |
| 15 | Death | 148 |
| 23 | Death | 11 |
| 33 | Death | 170 |
| 36 | Death | 4 |
| 43 | New myocardial infarction associated with TLR | 39 |
| 50 | New myocardial infarction | 213 |
| 61 | Death | 16 |
| 77 | Death | 1 |
| 83 | New myocardial infarction associated with TLR | 119 |
| 84 | Death | 4 |
| 92 | Death | 1 |
| 98 | Death | 0 |
| 101 | Death | 37 |
| 110 | Death | 0 |
| 113 | Death | 12 |
| 118 | Death | 253 |
| 121 | Death | 139 |
| 124 | New myocardial infarction associated with TLR | 291 |
| 128 | Death | 10 |
|
TLR, target lesion revascularization. Lost to follow-up: 6 patients (4.6%). |
||
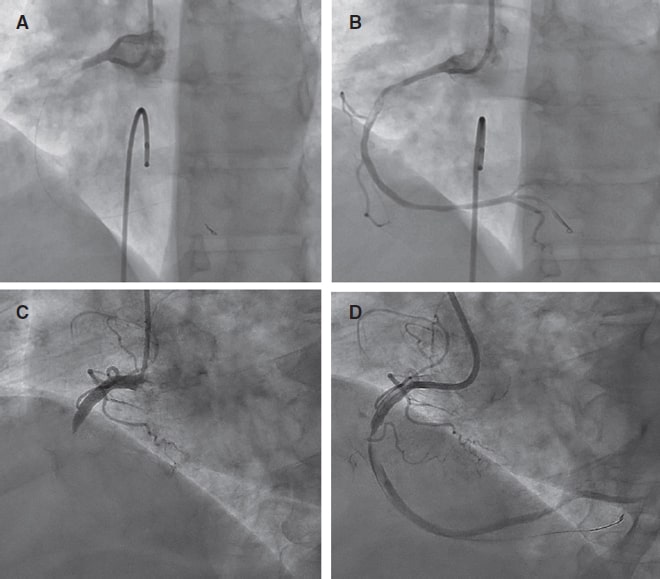
Figure 3. Pre- and post-ELCA findings in 2 typical cases of right coronary artery with large thrombus burden. ELCA, excimer laser coronary angioplasty.
DISCUSSION
The main finding of this single-center study is that coronary laser angioplasty is a feasible, safe, and effective adjuvant therapy in the context of PCI (videos 1-4 of the supplementary data), demonstrating a low rate of complications and an acceptable long-term rate of MACE.
Data on the use of ELCA in acute myocardial infarction remain limited, with most evidence coming from non-randomized clinical trials. The CARMEL trial,12 the largest multicenter study to date, evaluated the safety, feasibility, and acute outcomes of ELCA in patients with acute myocardial infarction within 24 h of symptom onset requiring urgent PCI. TIMI grade flow significantly improved after laser application, increasing from 1.2 to 2.8, with an overall procedural success rate of 91% and a low distal embolization rate of 2%, even though 65% of cases had a LTB. In our study, 95.4% of the patients had culprit lesions with a LTB, and laser delivery significantly improved the mean TIMI grade flow from 0.6 to 2.29, with a comparable distal embolization rate of 2.3%.
Arai et al.13 retrospectively analyzed 113 consecutive acute coronary syndrome cases undergoing PCI comparing an ELCA group (n = 48) with a thrombus aspiration group (n = 50). They found that ELCA was associated with a significantly shorter door-to-reperfusion time, a better myocardial blush grade, and fewer MACE vs thrombus aspiration. These favorable outcomes are likely attributable to ELCA’s ability to vaporize thrombi through acoustic shockwave propagation and dissolution mechanisms,12 as well as its capacity to suppress platelet aggregation kinetics (a phenomenon known as the ‘stunned platelet’ effect).14
Reperfusion injury to the coronary microcirculation is a critical concern during PCI in STEMI patients. While manual thrombus aspiration can reduce the rate of no-reflow in patients with a LTB, residual thrombi and decreased coronary flow following thrombectomy have been associated with a higher risk of no-reflow.15 In a study of 812 patients with STEMI and a LTB undergoing PCI, Jeon et al.16 reported that 34.4% experienced failed thrombus aspiration, defined as no thrombus retrieval, remnant thrombus grade ≥ 2, or distal embolization. This failure was associated with an increased risk of impaired myocardial perfusion and microvascular obstruction.
ELCA’s ability to vaporize thrombi (with a low rate of distal embolization) and mitigate platelet activation, key cofactors in myocardial reperfusion damage,17 can potentially reduce this undesirable effect. Although the direct impact of ELCA on coronary microcirculation in PCI has not been well documented, evidence from smaller studies suggests potential benefits. For example, Ambrosini et al.18 investigated ELCA in 66 patients with acute myocardial infarction and complete thrombotic occlusion of the infarcted related artery, demonstrating excellent acute coronary and myocardial reperfusion outcomes (as assessed by the myocardial blush score and the corrected TIMI frame count), as well as a low rate of long-term left ventricular remodeling (8%). The significant improvement in mean TIMI grade flow observed immediately after ELCA application in our cohort may indirectly suggest a protective effect of this technique on coronary microcirculation. However, the lack of large studies comparing ELCA with conventional STEMI treatment limits the ability to definitively confirm the benefits of coronary laser therapy in this setting. Shibata et al.19 explored the impact of ELCA on myocardial salvage using nuclear scintigraphy in 72 STEMI patients and an onset-to-balloon time < 6 h, comparing ELCA (n = 32) and non-ELCA (n = 40) groups. Their findings indicated a trend towards a higher myocardial salvage index in the ELCA vs the non-ELCA group (57.6% vs 45.6%).
Limitations
This study has several limitations. It is a retrospective analysis, which inherently introduces biases related to data collection, interpretation and application of inclusion and exclusion criteria. Besides, the absence of a comparative group limits the ability to establish the definitive clinical benefit of ELCA and its potential superiority over other strategies in the context of STEMI patients undergoing PCI. Furthermore, while the significant improvement of TIMI grade flow observed after laser application suggests potential benefits for coronary microcirculation, we did not directly assess this effect or thrombus burden reduction since post-ELCA thrombus grading was not systematically recorded. Unfortunately, in our retrospective database, PCI details (segmental analysis of coronary arteries and classification), the use of intravascular imaging modalities, dual antiplatelet therapy regimens (aspirin in addition to a potent P2Y12 inhibitor, or clopidogrel when prasugrel or ticagrelor were contraindicated, was routinely prescribed following current guidelines recommendations) or post-PCI echocardiography or cardiac magnetic resonance parameters were not systematically collected (unavailable in the health reports we revised) and follow-up data were missing for 4.6% of patients, all of which limited our ability to assess their potential impact on clinical outcomes. Last, our findings represent the experience of a single center, the percentage of women and patients with diabetes is relatively low, and procedures were performed by 5 trained operators, which may limit the external validity of the results.
CONCLUSIONS
ELCA seems to be an effective device for thrombus dissolution in the STEMI scenario, with excellent technical and procedural success rates. Besides, a low complication rate and favorable long-term outcomes with an acceptable event-free survival rate was observed in the present cohort.
DATA AVAILABILITY
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
FUNDING
None declared.
ETHICAL CONSIDERATIONS
This study was approved by the center Ethics Committee (waiving the need for informed consent due to the retrospective nature of the investigation) in full compliance with national legislation and the principles set forth in the Declaration of Helsinki. Sex was reported as per biological attributes (SAGER guidelines).
STATEMENT ON THE USE OF ARTIFICIAL INTELLIGENCE
The authors state that no generative artificial intelligence technologies were used in the preparation or revision of this article.
AUTHORS’ CONTRIBUTIONS
A. Pernigotti and M. Mohandes were responsible for the conceptualization and study design and contributed equally as co-first authors. M. Mohandes, A. Pernigotti, R. Bejarano, H. Coimbra, F. Fernández, C. Moreno, M. Torres, J. Guarinos were involved in data collection and statistical analysis. M. Mohandes, A. Pernigotti, and J.L. Ferreiro were involved in manuscript drafting and critical revision and were responsible for the supervision and final approval. All authors have accepted responsibility for the entire content of this manuscript and consented to its submission to the journal. Each author reviewed all results and approved the final version of the manuscript.
CONFLICTS OF INTEREST
The authors declared no conflicts of interest related to this manuscript. J.L. Ferreiro declared having received speaker’s fees from Eli Lilly Co, Daiichi Sankyo, Inc., AstraZeneca, Pfizer, Abbott, Boehringer Ingelheim, Bristol-Myers Squibb, Rovi, Terumo and Ferrer; consulting fees from AstraZeneca, Eli Lilly Co., Ferrer, Boston Scientific, Pfizer, Boehringer Ingelheim, Daiichi Sankyo, Inc., Bristol-Myers Squibb and Biotronik; and research grants from AstraZeneca, not related to this manuscript.
WHAT IS KNOWN ABOUT THE TOPIC?
- ELCA is a specialized technique used as adjuvant therapy during PCI for STEMI, particularly in patients with LTB.
- Although former studies have shown that ELCA can improve coronary flow and potentially reduce thrombotic material, data in the setting of acute myocardial infarction remain limited.
- ELCA is mostly used in high-volume centers by experienced operators, and standardized criteria for use in STEMI patients are not consistently reported in the literature.
WHAT DOES THIS STUDY ADD?
- This is one of the largest retrospective single-center series (130 patients) ever reported on the use of ELCA in STEMI patients with angiographically defined LTB.
- The study shows a high rate of technical and procedural success, significant improvement in TIMI flow, low rate of complication, and acceptable long-term outcomes.
- It provides detailed information on operator training, device selection, and laser settings, contributing to transparency and reproducibility.
- It also identifies current limitations in data reporting (eg, lack of systematic thrombus grading or dual antiplatelet therapy regimen documentation), underscoring the need for standardization in future studies.
SUPPLEMENTARY DATA
Vídeo 1. Mohandes M. DOI: 10.24875/RECICE.M25000537
Vídeo 2. Mohandes M. DOI: 10.24875/RECICE.M25000537
Vídeo 3. Mohandes M. DOI: 10.24875/RECICE.M25000537
Vídeo 4. Mohandes M. DOI: 10.24875/RECICE.M25000537
REFERENCES
1. Byrne RA, Rossello X, Coughlan JJ, et al. 2023 ESC guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44:3720-3826.
2. Kim MC, Cho JY, Jeong HC, et al. Long-term clinical outcomes of transient and persistent no reflow phenomena following percutaneous coronary intervention in patients with acute myocardial infarction. Korean Circ J. 2016;46:490-498.
3. Sardella G, Mancone M, Bucciarelli-Ducci C, et al. Thrombus aspiration during primary percutaneous coronary intervention improves myocardial reperfusion and reduces infarct size:the EXPIRA prospective, randomized trial. J Am Coll Cardiol. 2009;53:309-315.
4. Jolly SS, Cairns JA, Yusuf S, et al. Randomized trial of primary PCI with or without routine manual thrombectomy. N Engl J Med. 2015;372:1389-1398.
5. Lawton JS, Tamis-Holland JE, Bangalore S, et al. 2021 ACC/AHA/SCAI guideline for coronary artery revascularization:Executive summary. Circulation. 2022;145:e4-e17.
6. Grundfest WS, Litvack F, Forrester JS, et al. Laser ablation of human atherosclerotic plaque without adjacent tissue injury. J Am Coll Cardiol. 1985;5:929-933.
7. Mohandes M, Fernández L, Rojas S, et al. Safety and efficacy of coronary laser ablation as an adjuvant therapy in percutaneous coronary intervention:a single-centre experience. Coron Artery Dis. 2021;32:241-246.
8. Rawlins J, Din JN, Talwar S, O'Kane P. Coronary intervention with the excimer laser:review of the technology and outcome data. Interv Cardiol Rev. 2016;11:27-32.
9. Gibson CM, de Lemos JA, Murphy SA, et al. Combination therapy with abciximab reduces angiographically evident thrombus in acute myocardial infarction:a TIMI 14 substudy. Circulation. 2001;103:2550-2554.
10. Topaz O, Das T, Dahm J, et al. Excimer laser revascularisation:current indications, applications and techniques. Lasers Med Sci. 2001;16:72-77.
11. Ellis SG, Ajluni S, Arnold AZ, et al. Increased coronary perforation in the new device era. Incidence, classification, management, and outcome. Circulation. 1994;90:2725-2730.
12. Topaz O, Ebersole D, Das T, et al. Excimer laser angioplasty in acute myocardial infarction (the CARMEL multicenter trial). Am J Cardiol. 2004;93:694-701.
13. Arai T, Tsuchiyama T, Inagaki D, et al. Benefits of excimer laser coronary angioplasty over thrombus aspiration therapy for patients with acute coronary syndrome and thrombolysis in myocardial infarction flow grade 0. Lasers Med Sci. 2022;38:13.
14. Topaz O, Minisi AJ, Bernardo NL, et al. Alterations of platelet aggregation kinetics with ultraviolet laser emission:the “stunned platelet“phenomenon. Thromb Haemost. 2001;86:1087-1093.
15. Ahn SG, Choi HH, Lee JH, et al. The impact of initial and residual thrombus burden on the no-reflow phenomenon in patients with ST-segment elevation myocardial infarction. Coron Artery Dis. 2015;26:245-253.
16. Jeon HS, Kim YI, Lee JH, et al. Failed thrombus aspiration and reduced myocardial perfusion in patients with STEMI and large thrombus burden. JACC Cardiovasc Interv. 2024;17:2216-2225.
17. Rezkalla SH, Kloner RA. No-reflow phenomenon. Circulation. 2002;105:656-662.
18. Ambrosini V, Cioppa A, Salemme L, et al. Excimer laser in acute myocardial infarction:single centre experience on 66 patients. Int J Cardiol. 2008;127:98-102.
19. Shibata N, Takagi K, Morishima I, et al. The impact of the excimer laser on myocardial salvage in ST-elevation acute myocardial infarction via nuclear scintigraphy. Int J Cardiovasc Imaging. 2020;36:161-170.
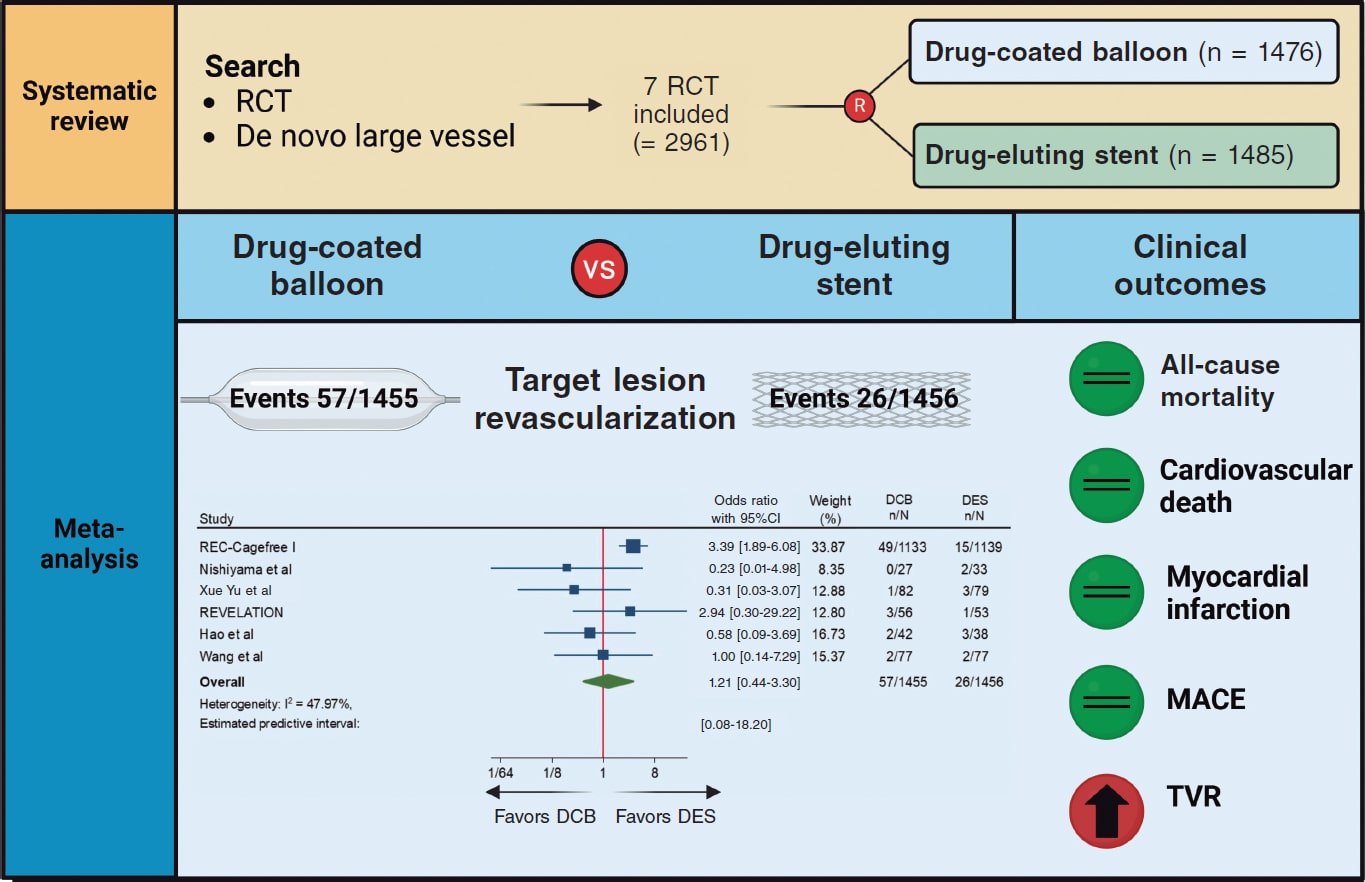
ABSTRACT
Introduction and objectives: To compare the effects of drug-coated balloon (DCB) vs drug-eluting stent (DES) in patients presenting with de novo large vessel coronary artery disease (CAD).
Methods: We conducted a systematic research of randomized controlled trials comparing DCB vs DES in patients with de novo large vessel CAD. Data were pooled by meta-analysis using a random-effects model. The prespecified primary endpoint was target lesion revascularization (TLR).
Results: A total of 7 trials enrolling 2961 patients were included. The use of DCB vs DES was associated with a similar risk of TLR (OR, 1.21; 95%CI, 0.44-3.30; I2 = 48%), all-cause mortality (OR, 1.56; 95%CI, 0.94- 2.57; I2 = 0%), cardiac death (OR, 1.65; 95%CI, 0.90-3.05; I2=0%), myocardial infarction (OR, 0.97; 95%CI, 0.58-1.61; I2 = 0%), major adverse cardiovascular adverse (OR, 1.19; 95%CI, 0.74-1.90; I2 = 13.5%) and late lumen loss (standardized mean difference [SMD], −0.35; 95%CI, −0.74 to 0.04; I2 = 81.4%). However, the DCB was associated with a higher risk of target vessel revascularization (OR, 2.47; 95%CI, 1.52-4.03; I2 = 0%) and smaller minimal lumen diameter during late follow-up (SMD, −0.36; 95%CI, −0.56 to −0.15; I2 = 34.5%). Nevertheless, prediction intervals included the value of no difference for both outcomes.
Conclusions: In patients with de novo large vessel CAD the use of DCB vs DES is associated with a similar risk of TLR. However, the DES achieves better late angiographic results.
Keywords: Drug-coated balloon. Drug-eluting stent. Coronary artery disease.
RESUMEN
Introducción y objetivos: Comparar los efectos del balón farmacoactivo (BFA) frente al stent farmacoactivo (SFA) en pacientes con enfermedad arterial coronaria (EAC) de vaso grande de novo.
Métodos: Se realizó una búsqueda sistemática de ensayos clínicos aleatorizados comparando BFA frente a SFA en pacientes con EAC de vaso grande de novo. Los datos se agruparon mediante un metanálisis de efectos aleatorios. El objetivo primario fue la necesidad de revascularización de la lesión diana (RLD).
Resultados: Se incluyeron 7 ensayos con 2.961 pacientes. El uso de BFA, en comparación con SFA, se asoció con un riesgo similar de RLD (OR = 1,21; IC95%, 0,44-3,30; I2 = 48%), muerte por todas las causas (OR = 1,56; IC95%, 0,94-2,57; I2 = 0%), muerte de causa cardiovascular (OR = 1,65; IC95%, 0,90-3,05; I2 = 0%), infarto de miocardio (OR = 0,97; IC95%, 0,58-1,61; I2 = 0%), acontecimientos adversos cardiacos mayores (OR = 1,19; IC95%, 0,74-1,90; I2 = 13,5%) y pérdida luminal tardía (DME = −0,35; IC95%, −0,74 a 0.04; I2 = 81,4%). Sin embargo, el BFA se asoció a un mayor riesgo de revascularización del vaso diana (OR = 2,47; IC95%, 1,52-4,03; I2 = 0%) y a un menor diámetro luminal mínimo en el seguimiento (DME: −0,36; IC95%, −0,56 a −0,15; I2 = 34,5%), aunque los intervalos de predicción incluyeron el valor nulo para ambos resultados.
Conclusiones: En los pacientes con EAC de vaso grande de novo, el BFA comparado con el SFA se asoció a un riesgo similar de RLD, obteniendo el SFA mejores resultados angiográficos.
Palabras clave: Balón farmacoactivo. Stent farmacoactivo. Enfermedad arterial coronaria.
Abbreviations
CAD: coronary artery disease. DCB: drug-coated balloon. DES: drug-eluting stent. MI: myocardial infarction. MLD: minimum lumen diameter. TLR: target lesion revascularization.
INTRODUCTION
Drug-eluting stents (DES) remain the standard of treatment for patients undergoing percutaneous coronary intervention (PCI).1,2 However, DES are associated with a gradually and permanent increased risk of adverse events, particularly due to late stent thrombosis and in-stent restenosis, with a 2% incidence rate per year with no plateau observed.1 This risk is even higher when complex and long lesions are treated.3 In recent years, drug-coated balloons (DCB) have emerged as a potential alternative treatment option to DES. Following adequate lesion preparation, unlike traditional stents, DCBs can release an antiproliferative drug into the vessel wall without leaving behind a permanent metal scaffold. Notably, permanent scaffolding can distort and constrain the coronary vessel, thus impairing vasomotion and adaptive remodelling, while also promoting chronic inflammation.4 DCB-PCI is a well-established treatment for in-stent restenosis and small-vessel coronary artery disease (CAD).5,6 However, its role in de novo large vessel CAD remains controversial. In a recent randomized clinical trial (RCT) with patients undergoing de novo CAD revascularization, a strategy of DCB-PCI did not achieve non-inferiority vs DES in terms of device-oriented composite endpoint driven by higher rates of target lesion revascularization (TLR).7 Contrary to prior published research, our findings did not support similar clinical outcomes for DCB vs DES in patients with de novo large vessel CAD.8,9 A recent meta-analysis of 15 studies compared DCB-PCI or hybrid angioplasty vs DES-PCI in patients with vessels > 2.75 mm in diameter showing no significant differences in the clinical endpoints of TLR, cardiac death, and MI.10 However, 14 of the 15 included studies were non-RCT, and the recent previously reported RCT was not included. Nevertheless, individual non-inferiority studies often lack the statistical power needed to definitively compare these technologies, underscoring the need for a systematic appraisal of treatment effects and evidence quality. Therefore, we conducted a systematic review and meta-analysis of available RCT to provide a comprehensive and quantitative assessment of evidence on the efficacy of DCB vs the current-generation DES in de novo large vessel CAD in terms of adverse events at longest available follow-up.
METHODS
Search strategy and selection criteria
We conducted a meta-analysis of RCT according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2009 guidelines.11 Two reviewers independently identified the relevant studies through an electronic search across the MEDLINE and Embase databases (from inception to October 2024). In addition, we employed backward snowballing (eg, reference review from identified articles and pertinent reviews). No language, publication date or publication status restrictions were imposed. This study is registered with PROSPERO and the search strategy is available in the supplementary data.
Study selection
Two reviewers independently assessed trial eligibility based on titles, abstracts, and full-text reports. Discrepancies in study selection were discussed and resolved with a third investigator. Eligible studies needed to meet the following pre-specified criteria: a) RCT comparing PCI with DCB and PCI with DES; b) study population including patients with de novo large vessel CAD (eg, defined as vessel diameter ≥ 2.5 mm);12 c) availability of clinical outcome data (without restriction as to follow-up time). Exclusion criteria were a) lack of a randomized design; b) studies including patients undergoing treatment for in-stent restenosis; c) studies including patients with de novo small vessel CAD; d) lack of any clinical outcome data.
A reference vessel diameter ≥ 2.5 mm was established as the cut-off value to define large vessel based on a recent proposed standardized definition.12
Data extraction
Three investigators (J. Llau García, S. Huélamo Montoro and J. A. Sorolla Romero) independently assessed studies for possible inclusion, with the senior investigator (J. Sanz-Sánchez) resolving discrepancies. Non-relevant articles were excluded based on title and abstract. The same investigators independently extracted data on study design, measurements, patient characteristics, and outcomes using a standardized data-extraction form. Data extraction conflicts were discussed and resolved with the senior investigator.
Data on authors, year of publication, inclusion and exclusion criteria, sample size, patients’ baseline patients, endpoint definitions, effect estimates, and follow-up time were collected.
Endpoints
The prespecified primary endpoint was TLR. Secondary clinical endpoints were all-cause mortality, cardiac death, myocardial infarction (MI), target vessel revascularization (TVR) and major adverse cardiovascular events (MACE). Secondary angiographic endpoints were minimum lumen diameter (MLD) and late lumen loss (LLL). Each endpoint was assessed according to the definitions reported in the original study protocols, as summarized in table 1 of the supplementary data. All the endpoints were assessed at the maximum follow-up available.
Table 1. Main features of included studies
| Study | Year of publication | No. of patients | Type of Device | Reference vessel diameter (mean ± SD) (mm) | Multicenter | Clinical follow up (months) | Angiographic follow-up (months) | |
|---|---|---|---|---|---|---|---|---|
| DCB | DES | |||||||
| REC-CAGEFREE I7 | 2024 | 1133 | 1139 | Paclitaxel-DCB Sirolimus-DES |
3.00 ± 0.55 | YES | 24 | NO |
| Nishiyama et al.13 | 2016 | 30 | 30 | Paclitaxel-DCB Everolimus-DES |
2.80 ± 0.63 | NO | 8 | 8 |
| Xue Yu et al.8 | 2022 | 85 | 85 | Paclitaxel-DCB Everolimus-DES |
2.89 ± 0.33 | NO | 12 | 9 |
| REVELATION9 | 2019 | 60 | 60 | Paclitaxel-DCB Sirolimus and everolimus DES |
3.24 ± 0.50 | NO | 24 | 9 |
| Gobic et al.15 | 2017 | 38 | 37 | Paclitaxel-DCB Sirolimus-DES |
> 2.50 | NO | 6 | 6 |
| Hao et al.16 | 2021 | 38 | 42 | Paclitaxel-DCB NA |
> 2.50 | NO | 12 | 12 |
| Wang et al.14 | 2022 | 92 | 92 | Paclitaxel-DCB Sirolimus-DES |
3.37 ± 0.52 | NO | 12 | 9 |
|
DCB, drug-coated balloon; DES, drug-eluting stent; NA, not available. |
||||||||
Risk of bias
The risk of bias in each study was assessed using the revised Cochrane risk of bias tool (RoB 2.0).11 Three investigators (J. Llau García, S. Huélamo Montoro and J. A. Sorolla Romero) independently assessed 5 domains of bias in RCT: a) randomization process, b) deviations from intended interventions, c) missing outcome data, d) outcome measurement, and e) selection of reported results (table 2 of the supplementary data).
Table 2. Baseline clinical characteristics of included patients
| Study | Age (years) | Male (%) | Diabetes (%) | Smoking (%) | Hypertension (%) | LVEF (%) | Clinical Presentation (CCS/ACS) (%) | Multivessel (%) | Complex lesion (%) |
|---|---|---|---|---|---|---|---|---|---|
| REC-CAGEFREE I7 | 62 | 69.3 | 27.3 | 45 | 60.1 | 60 | 44.9/55.3 | 4.8 | 0 |
| Nishiyama et al.13 | 69 | 73.3 | 41.6 | 60 | 83.3 | NA | 0/100 | NA | 36 |
| Xue Yu et al.8 | 63.3 | 69.3 | 24.1 | 54 | 63.9 | > 40 | 11.1/88.9 | 84 | 44.1 |
| REVELATION9 | 57 | 87 | 10 | 60 | 31 | 57.6 | 0/100 | 71.6 | N/A |
| Gobic et al.15 | 57.4 | 87 | 10 | 49.5 | 33.4 | 50.2 | 0/100 | NA | N/A |
| Hao et al.16 | 57.5 | 78.5 | 31.5 | 29.5 | 24 | 46 | 0/100 | NA | N/A |
| Wang et al.14 | 49.5 | 93.5 | 81.6 | 81.5 | 71.8 | NA | 0/100 | NA | N/A |
|
ACS, acute coronary syndrome; CCS, chronic coronary syndrome; NA, not available. |
|||||||||
Statistical analysis
Odds ratios (OR) and 95% confidence intervals (95%CI) were calculated using the DerSimonian and Laird random-effects model, with the estimate of heterogeneity being obtained from the Mantel-Haenszel method. The presence of heterogeneity among studies was evaluated with the Cochran Q chi-square test, with P ≤ .10 being considered of statistical significance, and using the I2 test to evaluate inconsistency. A value of 0% indicates no observed heterogeneity, and values of ≤ 25%, ≤ 50%, > 50% indicate low, moderate, and high heterogeneity, respectively. Prediction intervals (95%) in addition to conventional 95%CI around ORs were calculated to assess residual uncertainty. Publication bias and the small study effect were assessed for all outcomes, using funnel plots. The presence of publication bias was investigated using Harbord and Egger tests and visual estimation with funnel plots. We performed a sensitivity analysis by removing one study at a time to confirm that the findings, when compared with DES, were not driven by any single study. To account for different lengths of follow-up across studies, another sensitivity analysis was performed using the Poisson regression model with random intervention effects to calculate inverse-variance weighted averages of study-specific log stratified incidence rate ratios (IRRs). Results were displayed as IRRs, which are exponential ratios of the regression model. Additionally, random-effect meta-regression analyses were performed to assess the impact of the following variables on treatment effect with respect to the primary endpoint: eg, percentage of patients with acute coronary syndrome (ACS), percentage of patients with diabetes mellitus, mean reference vessel diameter and follow-up duration. The statistical level of significance was 2-tailed P < .05. Stata version 18.0 (StataCorp LP, College Station, United States), was used for statistical analyses.
RESULTS
Search results
Figure 1 illustrates the PRISMA study search and selection process. A total of 7 RCT were identified and included in this analysis. The main features of included studies are shown in table 1.
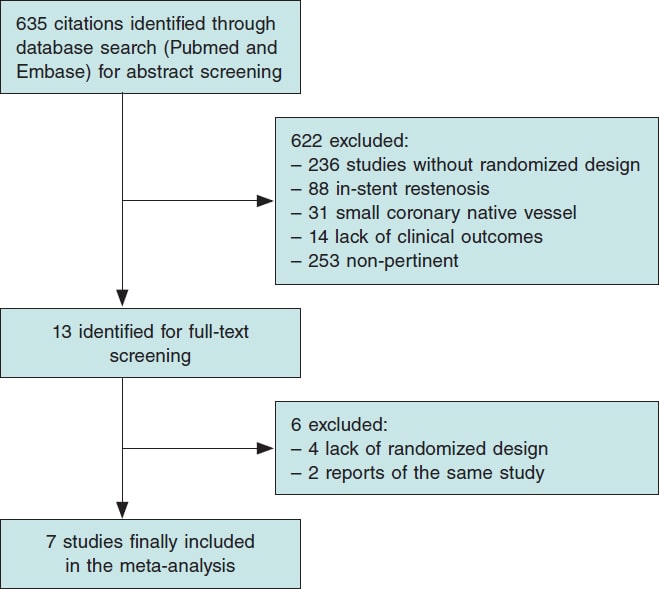
Figure 1. Flow diagram of the search for studies included in the meta-analysis according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Statement.
All studies had a non-inferiority design. A clinical primary endpoint was selected in 1 study,7 and an invasive functional endpoint was selected in another trial,9 while angiographic primary endpoints were prespecified in the remaining studies.8,13-16 The mean clinical and angiographic follow-up were 21.5 months and 8.9 months respectively. A total of 4 studies were conducted in the context of ACS9,14-17 and 1 study in the context of chronic coronary syndrome (CCS).13 Finally, 2 studies enrolled both ACS and CCS patients.7,8 A total of 3 trials enrolled patients treated with second-generation DES (Firebird 2.0 [Microport, China], Xience Xpedition [Abbott Vascular, United States], Orsiro [Biotronik, Germany]),7,9,13 and 2 studies enrolled patients treated with third-generation DES (Biomine [Meril Life Sciences, India], Cordimax [Rientech, China]).14,15 One trial enrolled patients treated with second and third-generation DES (Xience Xpedition [Abbott Vascular, United States], Resolute Integrity, [Medtronic, United States], Firehawk, [MicroPort, China]).8 All studies included patients who underwent paclitaxel-DCB-PCI ([Pantera Lux, Biotronik, Germany],9,14 [SeQuent Please, B Braun, Germany],7,8,13,15 [Bingo DCB, Yinyi Biotech,China]),16 and none with sirolimus-DCB-PCI.
Baseline characteristics
A total of 2961 patients were included, 1476 of whom received DCB and 1485, DES for de novo large vessel CAD. The patients main baseline characteristics are shown in table 2.
Publication bias and asymmetry
Funnel-plot distributions of the pre-specified outcomes indicate absence of publication bias for all the outcomes (figures 1-8 of the supplementary data).
Risk of bias assessment
Table 2 of the supplementary data illustrates the results of the risk of bias assessment with the RoB 2.0 tool. One trial was considered at low overall risk of bias,7 5 raised some concerns8,9,13,14,16 and 1 presented a high overall risk of bias.15
Outcomes
Clinical outcomes
DCB use compared with DES was associated with a similar risk of TLR (OR, 1.21; 95%CI, 0.44-3.30; I2 = 48%), all-cause mortality (OR, 1.56; 95%CI, 0.94- 2.57; I2 = 0%), cardiac death (OR, 1.65; 95%CI, 0.90-3.05; I2 = 0%), MI (OR, 0.97; 95%CI, 0.58-1.61; I2 = 0%) and MACE (OR, 1.19; 95%CI, 0.74-1.90; I2 = 13.5%). However, DCB was associated with a higher risk of TVR (OR, 2.47; 95%CI, 1.52- 4.03; I2 = 0%) (figure 2, figure 3 and figures 9-10 of the supplementary data).
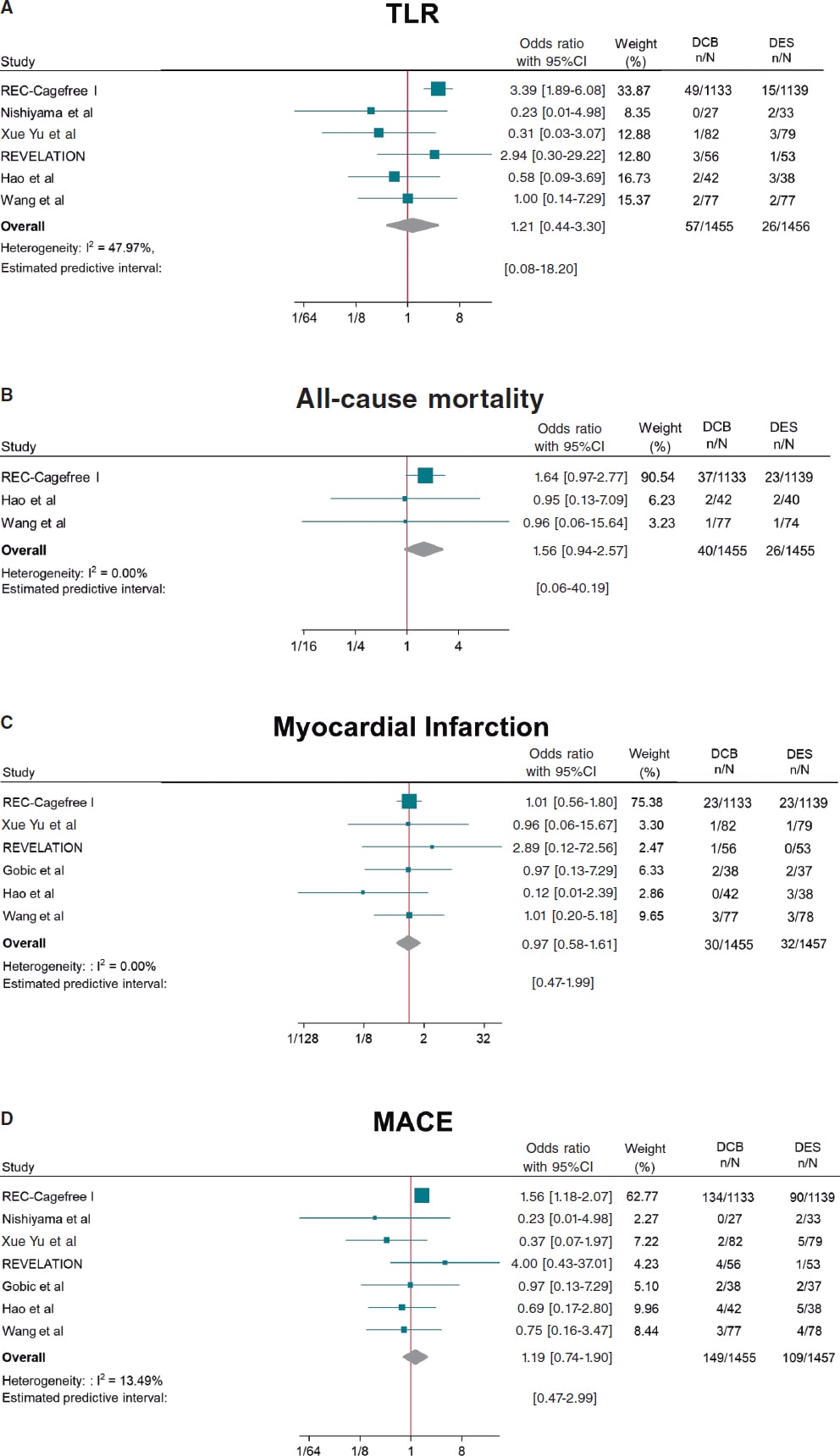
Figure 2. Forest plot reporting trial-specific and summary ORs with 95%CIs for the endpoint of A) target lesion revascularization; B) all-cause mortality; C) myocardial infarction; D) MACE. 95%CI, 95% confidence interval; DCB, drug-coated balloon; DES, drug-eluting stents; MACE, major adverse cardiovascular events; OR, odds ratio. References: REC-Cagefree I.,7 Nishiyama et al.,13 Xue Yu et al.,8 REVELATION,9 Hao et al.,16 Wang et al.,14 and Gobic et al.15
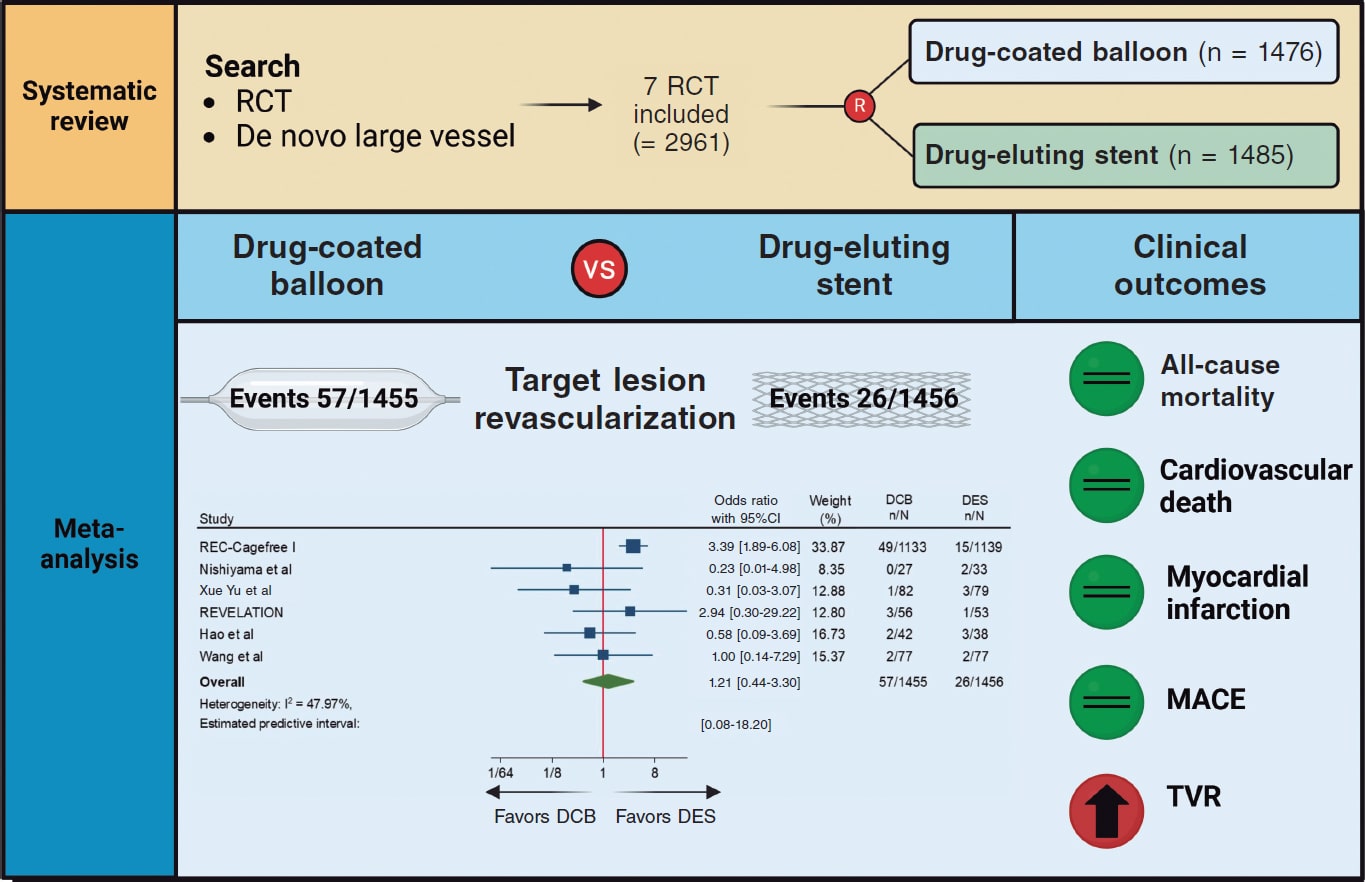
Figure 3. Central Illustration. DCB, drug-coated balloon; DES, drug-eluting stent; RCT, randomized clinical trial; TVR, target vessel revascularization. References: REC-Cagefree I.,7 Nishiyama et al.,13 Xue Yu et al.,8 REVELATION,9 Hao et al.,16 and Wang et al.14
Angiographic outcomes
Compared with DES, DCB use yielded significant smaller MLD (SMD, −0.36; 95%CI, −0.56 to −0.15; I2 = 34.5%) and similar risk of LLL (SMD, −0.35; 95%CI, −0.74 to 0.04; I2 = 81.4%) at follow-up (figure 4).
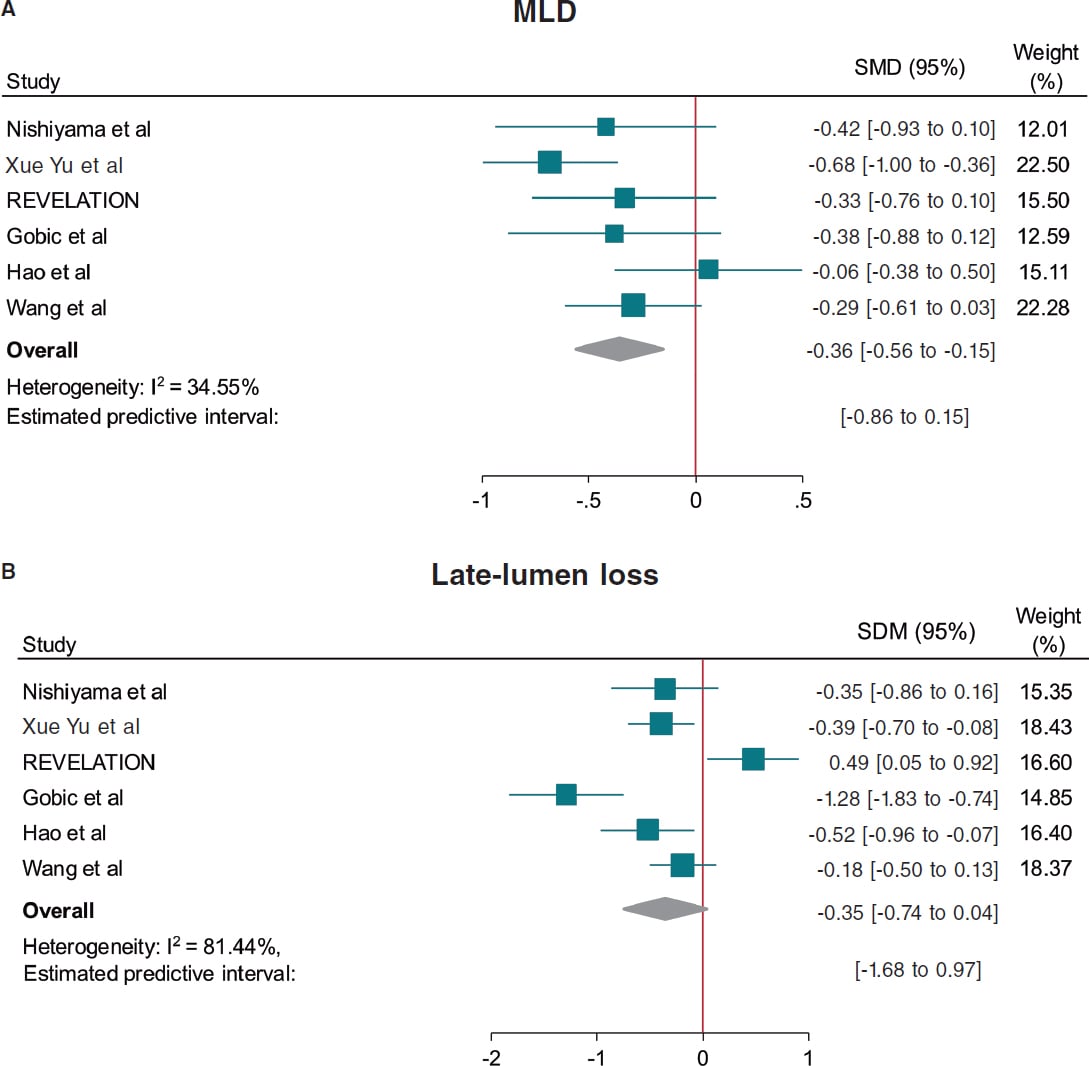
Figure 4. Forest plot reporting trial-specific and summary ORs with 95%CIs for the endpoint of A: minimum lumen diameter, and B: late-lumen loss. 95%CI, 95% confidence interval; DCB, drug-coated balloon; DES, drug-eluting stents; MACE, major adverse cardiovascular events; MLD, minimum lumen diameter; SMD, standardized mean difference; OR, odds ratio. References: Nishiyama et al.,13 Xue Yu et al.,8 REVELATION,9 Gobic et al.,15 Hao et al.,16 and Wang et al.14.
Prediction intervals were consistent with CI for all the outcomes except for TVR and MLD, which included the value of no difference.
Sensitivity analysis
A leave-one-out pooled analysis by iteratively removing one study at a time was performed for all endpoints. Treatment effects were consistent with the main analysis for TLR, all-cause mortality, cardiac death, MI and MLD. The risk of TVR was no longer significantly higher among patients undergoing DCB when removing the CAGEFREE I trial,7 and the risk of LLL was significantly lower among patients undergoing DCB-PCI when removing the REVELATION trial.9 However, an increased risk of MACE was observed among patients undergoing DCB-PCI when removing the study by Xue Yu et al.18 (tables 3-10 of the supplementary data). A sensitivity analysis using estimated IRRs was performed to account for varying follow-up lengths, confirming that our main analysis findings remained unchanged (table 11 of the supplementary data).
Random effect meta-regression analysis found no significant impact of the proportion of patients presenting with ACS (P = .882), diabetes mellitus (P = .641), mean reference vessel diameter (P = .985) and follow-up duration (P = .951) on treatment effect with respect to the primary endpoint.
DISCUSSION
This meta-analysis provides a comprehensive and updated quantitative analysis of available evidence on the comparison of DCB vs DES in de novo large vessel CAD, including data from 2961 patients enrolled in 7 RCT. The main findings of the study are:
a) The use of DCB was associated with a similar risk of clinical events vs DES except for TVR. However, data for this outcome was only available in 3 of the 7 included studies and the increased risk in patients undergoing DCB-PCI was not significant when the CAGEFREE I trial was removed. In addition, prediction intervals were not consistent with the CI. Therefore, the results of this outcome should be interpreted with caution.
b) The effect of DCB on the risk of TLR was not affected by the proportion of patients presenting with ACS or diabetes, as well as the mean reference vessel diameter or follow-up duration as assessed by meta-regression analysis.
c) DCB was associated with lower MLD at angiographic follow-up, but with similar LLL vs DES.
DES are the standard of treatment for patients undergoing PCI. However, complications such as stent thrombosis and in-stent restenosis still occur with rates estimated at 0.7-1% and 5-10% at the 10-year follow-up respectively.19,20 Therefore, in recent years there has been a growing concern for developing strategies to reduce stent-related adverse events. In this context, DCBs have emerged as a potential treatment alternative based on a “leaving nothing behind” strategy. Nevertheless, data of patients presenting with de novo large CAD is scarce and conflicting. The CAGEFREE I is the only available clinically powered RCT that included 2272 patients undergoing de novo non-complex CAD revascularization across 40 centers in China. A strategy of DCB-PCI did not achieve non-inferiority vs DES in terms of device-oriented composite endpoint driven by higher rates of TLR in the DCB-PCI group (3.1% vs 1.2%, P = .002). On the other hand, in single-center RCT conducted by Nishiyama et al. with 60 patients with CCS undergoing elective PCI a trend toward lower rates of TLR in the DCB-PCI group (0% vs 6.1%, P = .193) was shown at the 8-mont follow-up.13 Similarly, in a RCT including 170 patients undergoing PCI for de novo large CAD lower rates of TLR at the 12-month follow-up were found in patients undergoing DCB-PCI (1.6% vs 3.4%, P = .306).14 In our analysis when pooling data from all available RCT, the risk of TLR was similar among patients undergoing DCB-PCI or DES-PCI. Notably, since this result was obtained with a moderate heterogeneity (I2 ≈ 50%), it should be interpreted with caution regarding its general applicability. These findings remained unvaried at the leave-one-out analysis. In addition, prediction intervals were consistent with CI around ORs showing lack of residual uncertainty. Previous studies have shown that in-stent restenosis after DES is not a benign phenomenon, presenting as an ACS in about 70% of the cases, with 5-10% of these resulting in MI.21 We could speculate that the lack of permanent scaffold with DCB vs DES may predispose to a less aggressive pattern of restenosis and not increase the risk of thrombotic vessel closure beyond 3 months when vessel healing after DCB-PCI has occurred.22
Notably, 5 of the 7 studies included in this meta-analysis enrolled patients presenting with ACS. A total of 34% of the patients included in the CAGEFREE study presented with ACS, with 16% being STEMI cases.7 Four other studies only included STEMI patients.7,9,14-16 Although the performance of DCB in the STEMI scenario is unknown, its use in clinical practice is increasing.23 Culprit lesion plaques in STEMI patients are usually soft and adequate plaque modification can be easily achieved through DCB-PCI (< 30% residual stenosis and low grade of dissection).23 Moreover, the ruptured lipid rich plaque can potentially be an ideal reservoir for effective paclitaxel uptake.24 On the other hand, DCBs carry specific risks for STEMI patients, such as acute recoil and culprit lesion closure, because they don’t provide vessel scaffolding.
In our study, the proportion of patients presenting with ACS had no impact on treatment effects on the meta-regression analysis. Nevertheless, further RCT with adequate sample size are needed to obtain more solid evidence in this field. Of note, complex lesions (eg, severe calcification and bifurcations with planned two-stent technique) were excluded from the studies that included patients presenting with CCS.7,8 Therefore, our findings might not be generalized to this population.
The better angiographic surrogate outcomes with DES-PCI vs DCB-PCI found in our meta-analysis after pooling data from 6 studies can be explained by the absence of a metal scaffold to expand the vessel lumen and the acute recoil following balloon angioplasty. This justifies the lower MLD achieved after DCB-PCI vs DES-PCI. While our analysis did not show significant differences regarding LLL during follow-up, the value of LLL was lower among patients undergoing DCB-PCI when excluding the REVELATION trial.9,17 This study showed extremely low LLL in both DCB and DES groups vs other available evidence from RCT.15,16 The presence of positive vessel remodeling with a late lumen enlargement after the use of DCB evaluated by intracoronary imaging modalities has been evidenced in multiple studies, and seems to be associated with small vessel disease, fibrous and layered plaques and a post-PCI medial dissection arc > 90°.25,26,27 However, evidence of this phenomenon in patients with large vessel CAD is less known.22 It should, therefore, be noted that all studies in this meta-analysis used paclitaxel-DCB. While the evidence comparing sirolimus and paclitaxel-DCB is scarce, 2 recent RCT have shown better angiographic results with the lipophilic component. In the first one, with 121 patients with the novo small vessel CAD, sirolimus-DCB failed to achieve non-inferiority for net-lumen gain at 6 months.28 In the second study, with 70 patients, the 2 devices showed similar results of LLL at 6 months, although patients treated with paclitaxel-DCB had more frequent late luminal enlargement.29 Due to the small sample size and although there is not enough evidence to evaluate differences across clinical endpoints, we cannot assume that there is a class effect across all DCBs. There are larger ongoing RCT to evaluate the outcomes of sirolimus DCB vs DES in large vessels that will provide evidence in this field.30,31
Limitations
The results of our investigation should be interpreted in light of some limitations. First, this is a study-level meta-analysis providing average treatment effects. The lack of patient-level data from the included studies prevents us from assessing the impact of baseline clinical, angiographic and procedural characteristics on treatment effects. Second, minor differences in definition were present for some endpoints (eg, MACE), limiting the reliability of effect estimates. Third, one study which accounted for approximately 75% of all patients included did not included angiographic follow-up,7 thus limiting the evaluation of DCB and DES on angiographic outcomes. Fourth, the clinical follow-up varied from 6 to 24 months. Ideally, outcomes such as TLR should be compared at uniform follow-up across studies (eg, at 1 year), which was not consistently possible in the current analysis. Nonetheless, these differences in follow-up duration were accounted with the IRRs, as detailed in the Methods section. However, longer follow-ups are needed to establish the safety and efficacy profile of DCB vs DES throughout time. Fifth, the definition of large vessel is inconsistent across trials, which might be a source of bias. Finally, the limited number of studies and patients, and the small event rate for some endpoints, such as all-cause mortality may reduce the power for detecting significant differences across groups.
CONCLUSIONS
This meta-analysis provides the most updated quantitative evidence on the use of DCB vs DES for the treatment of de novo large vessel CAD in both CCS and ACS. DCB-PCI is associated with similar TLR and LLL at mid-term follow-up representing an appealing treatment option for patients with large vessel CAD.
FUNDING
None declared.
ETHICAL CONSIDERATIONS
Ethics approval was deemed unnecesary for this meta-analysis as all data were collected and synthesized from previous studies. Additionally, no informed consent was required as there were no patients involved in our work. The meta-analysis of RCT was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses 2009 guidelines. We confirm that sex/gender biases have been taken into consideration.
STATEMENT ON THE USE OF ARTIFICIAL INTELLIGENCE
No artificial intelligence has been used in the preparation of this article.
AUTHORS’ CONTRIBUTIONS
J. Llau García, S. Huelamo Montoro and J.A. Sorolla Romero participated in literature research and study selection. J.A. Sorolla Romero, L. Novelli and J. Sanz Sánchez contributed to the conception, design, drafting and revision of the article. P. Rubio, J.L. Díez Gil, L. Martínez-Dolz, I.J. Amat Santos, B. Cortese, F. Alfonso, and H.M. Garcia-Garcia contributed to the critical revision of the intellectual content of the article.
CONFLICTS OF INTEREST
F. Alfonso is an associate editor of REC: Interventional Cardiology; the journal’s editorial procedure to ensure impartial handling of the manuscript has been followed. The authors declared no relevant relationships with the contents of this paper.
WHAT IS KNOWN ABOUT THE TOPIC?
- DCB are a well-established treatment for patients with small-vessel CAD.
- Available published evidence of patients with de novo large vessel CAD is scarce and shows conflicting results.
WHAT DOES THIS STUDY ADD?
- In this meta-analysis including data from 2961 patients enrolled in 7 RCT, DCB showed similar risk of clinical events at follow-up vs DES in the treatment of de novo large vessel CAD.
- The use of DCB might be considered as an alternative option to DES in patients undergoing PCI for non-complex de novo large vessel CAD.
REFERENCES
1. Neumann FJ, Sousa-Uva M, Ahlsson A, et al. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40:87-165.
2. Lawton JS, Tamis-Holland JE, Bangalore S, et al. 2021 ACC/AHA/SCAI Guideline for Coronary Artery Revascularization:Executive Summary:A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145:e4-e17.
3. Kong MG, Han JK, Kang JH, et al. Clinical outcomes of long stenting in the drug-eluting stent era:patient-level pooled analysis from the GRAND-DES registry. EuroIntervention J Eur Collab Work Group Interv Cardiol Eur Soc Cardiol. 2021;16:1318-1325.
4. Kawai T, Watanabe T, Yamada T, et al. Coronary vasomotion after treatment with drug-coated balloons or drug-eluting stents:a prospective, open-label, single-centre randomised trial. EuroIntervention. 2022;18:e140?e148.
5. Jeger RV, Eccleshall S, Wan Ahmad WA, et al. Drug-Coated Balloons for Coronary Artery Disease:Third Report of the International DCB Consensus Group. JACC Cardiovasc Interv. 2020;13:1391-1402.
6. Sanz Sánchez J, Chiarito M, Cortese B, et al. Drug-Coated balloons vs drug-eluting stents for the treatment of small coronary artery disease:A meta-analysis of randomized trials. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv. 2021;98:66-75.
7. Gao C, He X, Ouyang F, et al. Drug-coated balloon angioplasty with rescue stenting versus intended stenting for the treatment of patients with de novo coronary artery lesions (REC-CAGEFREE I):an open-label, randomised, non-inferiority trial. Lancet Lond Engl. 2024;404:1040-1050.
8. Yu X, Wang X, Ji F, et al. A Non-inferiority, Randomized Clinical Trial Comparing Paclitaxel-Coated Balloon Versus New-Generation Drug-Eluting Stents on Angiographic Outcomes for Coronary De Novo Lesions. Cardiovasc Drugs Ther. 2022;36:655-664.
9. Vos NS, Fagel ND, Amoroso G, et al. Paclitaxel-Coated Balloon Angioplasty Versus Drug-Eluting Stent in Acute Myocardial Infarction:The REVELATION Randomized Trial. JACC Cardiovasc Interv. 2019;12:1691-1699.
10. Gobbi C, Giangiacomi F, Merinopoulos I, et al. Drug coated balloon angioplasty for de novo coronary lesions in large vessels:a systematic review and meta-analysis. Sci Rep. 2025;15:4921.
11. Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses:the PRISMA statement. BMJ. 2009;339:b2535.
12. Sanz-Sánchez J, Chiarito M, Gill GS, et al. Small Vessel Coronary Artery Disease:Rationale for Standardized Definition and Critical Appraisal of the Literature. J Soc Cardiovasc Angiogr Interv. 2022;1:100403.
13. Nishiyama N, Komatsu T, Kuroyanagi T, et al. Clinical value of drug-coated balloon angioplasty for de novo lesions in patients with coronary artery disease. Int J Cardiol. 2016;222:113-118.
14. Wang Z, Yin Y, Li J, et al. New Ultrasound-Controlled Paclitaxel Releasing Balloon vs. Asymmetric Drug-Eluting Stent in Primary ST-Segment Elevation Myocardial Infarction-A Prospective Randomized Trial. Circ J Off J Jpn Circ Soc. 2022;86:642-650.
15. Gobic´D, Tomulic´V, Lulic´D, et al. Drug-Coated Balloon Versus Drug-Eluting Stent in Primary Percutaneous Coronary Intervention:A Feasibility Study. Am J Med Sci. 2017;354:553-560.
16. Hao X, Huang D, Wang Z, Zhang J, Liu H, Lu Y. Study on the safety and effectiveness of drug-coated balloons in patients with acute myocardial infarction. J Cardiothorac Surg. 2021;16:178.
17. Niehe SR, Vos NS, Van Der Schaaf RJ, et al. Two-Year Clinical Outcomes of the REVELATION Study:Sustained Safety and Feasibility of Paclitaxel-Coated Balloon Angioplasty Versus Drug-Eluting Stent in Acute Myocardial Infarction. J Invasive Cardiol. 2022;34:E39-E42.
18. Xue W, Ma J, Yu X, et al. Analysis of the incidence and influencing factors associated with binary restenosis of target lesions after drug-coated balloon angioplasty for patients with in-stent restenosis. BMC Cardiovasc Disord. 2022;22:493.
19. Coughlan JJ, Maeng M, Räber L, et al. Ten-year patterns of stent thrombosis after percutaneous coronary intervention with new- versus early-generation drug-eluting stents:insights from the DECADE cooperation. Rev Esp Cardiol. 2022;75:894-902.
20. Madhavan MV, Redfors B, Ali ZA, Prasad M, et al. Long-Term Outcomes After Revascularization for Stable Ischemic Heart Disease:An Individual Patient-Level Pooled Analysis of 19 Randomized Coronary Stent Trials. Circ Cardiovasc Interv.2020;13:e008565.
21. Buchanan KD, Torguson R, Rogers T, et al. In-Stent Restenosis of Drug-Eluting Stents Compared With a Matched Group of Patients With De Novo Coronary Artery Stenosis. Am J Cardiol. 2018;121:1512-1518.
22. Antonio Sorolla Romero J, Calderón AT, Tschischke JPV, Luis Díez Gil J, Garcia-Garcia HM, Sánchez JS. Coronary plaque modification and impact on the microcirculation territory after drug-coated balloon angioplasty:the PLAMI study. Rev Esp Cardiol. 2025;78:481-482.
23. Merinopoulos I, Gunawardena T, Corballis N, et al. Assessment of Paclitaxel Drug-Coated Balloon Only Angioplasty in STEMI. JACC Cardiovasc Interv. 2023;16:771-779.
24. Maranhão RC, Tavares ER, Padoveze AF, Valduga CJ, Rodrigues DG, Pereira MD. Paclitaxel associated with cholesterol-rich nanoemulsions promotes atherosclerosis regression in the rabbit. Atherosclerosis. 2008;197:959-966.
25. Kleber FX, Schulz A, Waliszewski M, et al. Local paclitaxel induces late lumen enlargement in coronary arteries after balloon angioplasty. Clin Res Cardiol Off J Ger Card Soc. 2015;104:217-225.
26. Alfonso F, Rivero F. Late lumen enlargement after drug-coated balloon therapy:turning foes into friends. EuroIntervention J Eur Collab Work Group Interv Cardiol Eur Soc Cardiol. 2024;20:523-525.
27. Yamamoto T, Sawada T, Uzu K, Takaya T, Kawai H, Yasaka Y. Possible mechanism of late lumen enlargement after treatment for de novo coronary lesions with drug-coated balloon. Int J Cardiol. 2020;321:30-37.
28. Ninomiya K, Serruys PW, Colombo A, et al. A Prospective Randomized Trial Comparing Sirolimus-Coated Balloon With Paclitaxel-Coated Balloon in De Novo Small Vessels. JACC Cardiovasc Interv. 2023;16:2884-2896.
29. Ahmad WAW, Nuruddin AA, Abdul KMASK, et al. Treatment of Coronary De Novo Lesions by a Sirolimus- or Paclitaxel-Coated Balloon. JACC Cardiovasc Interv. 2022;15:770-779.
30. Spaulding C, Krackhardt F, Bogaerts K, et al. Comparing a strategy of sirolimus-eluting balloon treatment to drug-eluting stent implantation in de novo coronary lesions in all-comers:Design and rationale of the SELUTION DeNovo Trial. Am Heart J. 2023;258:77-84.
31. Greco A, Sciahbasi A, Abizaid A, et al. Sirolimus-coated balloon versus everolimus-eluting stent in de novo coronary artery disease:Rationale and design of the TRANSFORM II randomized clinical trial. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv. 2022;100:544-552.
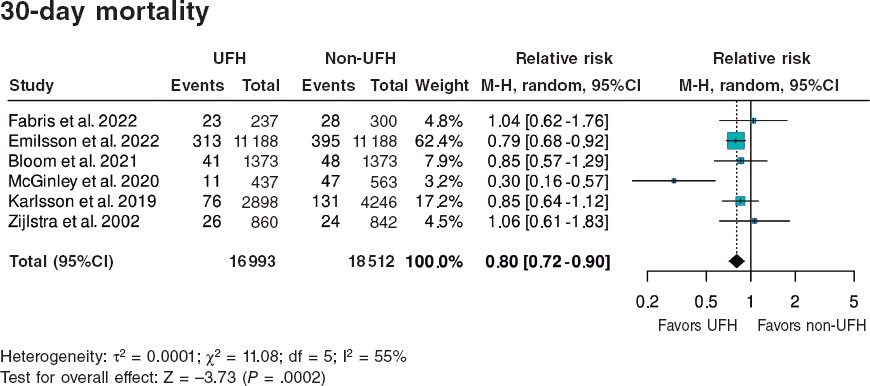
ABSTRACT
Introduction and objectives: The early administration of unfractionated heparin (UFH) for ST-segment elevation myocardial infarction (STEMI) is still a matter of discussion, and clinical practice guidelines leave the timing of administration prior to angioplasty at the physician’s discretion.
Methods: We conducted a systematic search across PubMed/Cochrane databases for studies comparing pre-treatment with UFH with a comparative untreated group (non-UFH) of patients with STEMI undergoing primary angioplasty and including TIMI flow and 30-day mortality targets from June 2024 through September 2024. We conducted a randomized meta-analysis and assessed the risk of publication bias to detect asymmetry in the included studies.
Results: We included a total of 7 studies published from 2002 through 2022 (6 retrospective trials and 1 substudy of a randomized trial) for a total of 36 831 patients: 17 751 in the UFH pre-treatment group and 19 080 in the non-UFH control group. A total of 6202 patients (31.6%) on UFH had TIMI grade-II/III flow vs 5106 (23.0%) on non-NFH while 490 (3.9%) on UFH died within 30 days vs 673 (5.1%) on non-NFH. Meta-analysis demonstrated a higher probability of TIMI grade-II/III flow (HR, 1.35; 95%CI, 1.25-1.45; P < .0001) and a lower 30-day mortality rate in patients on UFH pretreatment (HR, 0.80; 95%CI, 0.72-0.90; P = .0002), with no differences being reported in bleeding complications (HR, 0.87; 95%CI, 0.72-1.05; P = .150).
Conclusions: Meta-analysis of studies shows that pretreatment with UFH in STEMI patients undergoing primary angioplasty is associated with a higher probability of TIMI grade-II/III flow and a lower risk of early mortality.
Meta-analysis registered in PROSPERO (CRD420250655362).
Keywords: Meta-analysis. Unfractionated heparin. ST-segment elevation myocardial infarction. Prognosis. Pre-treatment. Acute myocardial infarction.
RESUMEN
Introducción y objetivos: La administración temprana de heparina no fraccionada (HNF) en el infarto agudo de miocardio con elevación del segmento ST (IAMCEST) está sujeta a controversia, por lo que las guías de práctica clínica dejan a criterio médico el momento de su administración antes de la angioplastia.
Métodos: Entre junio y septiembre de 2024 se realizó una búsqueda sistemática en PubMed y Cochrane de estudios que comparasen el pretratamiento con HNF con un grupo control no tratado (no-HNF) en pacientes con IAMCEST tratados con angioplastia primaria e incluyesen los objetivos de flujo TIMI y la mortalidad a 30 días. Se llevó a cabo un metanálisis aleatorizado, en el que se evaluó el riesgo de sesgo de publicación para detectar asimetría en los estudios incluidos.
Resultados: Se incluyeron 7 estudios publicados entre 2002 y 2022, de los cuales 6 eran retrospectivos y 1 subestudio de un ensayo aleatorizado, con 36.831 pacientes: 17.751 el grupo de pretratamiento con HNF y 19.080 el grupo control no-HNF. Un total de 6.202 (31,6%) con HNF tuvieron flujo TIMI II/III, frente a 5.106 (23,0%) de los no-HNF, y 490 (3,9%) con HNF fallecieron en 30 días, frente a 673 (5,1%) de los no-HNF. El metanálisis demostró mayor probabilidad de flujo TIMI II/III (HR = 1,35; IC95%, 1,25-1,45; p < 0,0001) y menor mortalidad en los pacientes que recibieron pretratamiento con HNF (HR = 0,80; IC95%, 0,72-0,90; p = 0,0002), sin diferencias en complicaciones hemorrágicas (HR = 0,87; IC95%, 0,72-1,05; p = 0,150).
Conclusiones: El metanálisis muestra que el pretratamiento con HNF en pacientes con IAMCEST y angioplastia primaria se asocia a una mayor probabilidad de flujo TIMI II/III y un menor riesgo de mortalidad precoz.
Metanálisis registrado en PROSPERO (CRD420250655362).
Palabras clave: Metanálisis. Heparina no fraccionada. Infarto con elevación del segmento ST. Pronóstico. Pretratamiento. Infarto agudo de miocardio.
Abbreviations
PCI: percutaneous coronary intervention. STEMI: ST-segment elevation myocardial infarction. TIMI: Thrombolysis in Myocardial Infarction. UFH: unfractionated heparin.
INTRODUCTION
The implementation of STEMI Code protocols, involving emergency and cardiology services, has led to improved care for ST-segment elevation myocardial infarction (STEMI) and lower morbidity and mortality rates.1 Correct diagnosis of STEMI, pretreatment with antiplatelet agents, and the organization of rapid and direct transfer to a center with an PCI-capable center for primary angioplasty are quality standards in the management of STEMI.1
Parenteral anticoagulation is generally recommended in acute coronary syndrome at the time of diagnosis.1 In STEMI, the use of unfractionated heparin (UFH) during primary angioplasty is recommended to prevent coronary thrombosis and device-related complications, but its use should be discontinued after the procedure.2
The precise role of UFH pretreatment at the time of first medical contact for patients diagnosed with STEMI remains to be fully defined. The 2023 clinical practice guidelines of the European Society of Cardiology1 allow attending physicians to decide when to administer UFH during treatment, as there is no solid evidence supporting its early use. This flexibility is based on the absence of conclusive data on the benefits of UFH at this stage of treatment.1,3
The most recent data published on the implementation of STEMI Code protocols and care networks in Spain reveal heterogeneity in response times and transport among the different autonomous communities (AC).4,5 This heterogeneity is also observed in the administration of anticoagulant and antiplatelet pretreatment across the 17 AC. A review of STEMI Code protocols as of December 2024 shows that in 6 of the 17 (35.3%) AC, pretreatment with UFH is recommended, representing coverage for 43.1% of the Spanish population (table 1 of the supplementary data). All AC, except for one, include dual antiplatelet therapy as pretreatment at the first medical contact in their protocols. Differences in the standardization of UFH use in STEMI Code protocols reflect the lack of evidence and concrete recommendations on this topic.
Table 1. Demographic data of populations and characteristics of the selected studies
| Study | Design | Country | n | n (%) | Age, years | Concomitant antiplatelets, drug, and dosis | Male sex | Door-to-balloon time | UFH dosis | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | ||||
| Fabris et al. (2022)10 | Retrospective | Italy | 537 | 237 (44.1%) | 300 (55.9%) | 66.0 ± 12.5 | 67.0 ± 12.0 | ASA: 237, 250 mg (100%) Ticagrelor: 237, 280 mg (100%) | ASA: 300, 250 mg (100%) PCI-capable center: UFH + ticagrelor or prasugrel or clopidogrel | 176 (74.3%) | 226 (75.3%) | 77 | 74 | 70 IU/kg | 70 IU/kg |
| Emilsson et al. (2022)6 | Retrospective | Sweden | 22 376 | 11 188 (50.0%) | 11 188 (50.0%) | 67.0 ± 12.0 | 67.0 ± 12.0 | ASA: 226, NR (2%) Clopidogrel: 221, NR (22%) Ticagrelor: 4642, NR (41%), Prasugrel: 574, NR (5.1%) | ASA: 170, NR (1.5%) Clopidogrel: 28, NR (0.3%) Ticagrelor: 4486, N (40%) Prasugrel: 608, NR (5.4%) | 7877 (70%) | 7992 (71%) | 276 ± 244 | 290 ± 270 | NR | NR |
| Bloom et al. (2021)7 | Retrospective | Australia | 2746 | 1373 (50.0%) | 1373 (50.0%) | 63.0 ± 12.4 | 63.2 ± 12.7 | ASA: 1327, NR (96.6%) Ticagrelor: 944, NR (68.8%) | ASA: 1326, NR (96.6%) Ticagrelor: 975, NR (70.9%) | 1099 (80.0%) | 1081 (78.7%) | 48 ± 23 | 64 ± 47 | 4000 + 1000 IU/h in ambulance | 4000 IU |
| McGinley et al. (2020)8 | Retrospective | Scotland | 1000 | 437 (43.7%) | 563 (56.3%) | 63.7 ± NR | 63.7 ± NR | ASA: 437, NR (100%) Clopidogrel: 437, NR (100%) | ASA: NR Clopidogrel: NR | 304 (69.6%) | 390 (69.3%) | NR | NR | 5000 IU | 5000 IU |
| Karlsson et al. (2019)11 | Subanálisis de ensayo clínico aleatorizado | Sweden | 7144 | 2898 (40.6%) | 4246 (59.4%) | 66.0 ± 11.5 | 66.0 ± 11.6 | ASA: 2817, NR (97.2%), Clopidogrel: 1662, NR (57.4%), Ticagrelor: 731, NR (25.2%) Prasugrel: 243, NR (8.4%) | ASA: 3636, NR (85.6%) Clopidogrel: 2489, NR (58.6%) Ticagrelor: 578, NR (13.6%) Prasugrel: 338, NR (8%) | 2169 (74.8%) | 3177 (74.8%) | 185 (125–320) | 181 (118–327) | NR | NR |
| Giralt et al. (2015)9 | Retrospective | Spain | 1326 | 758 (57.2%) | 568 (42.8%) | 61.3 ± 12.8 | 63.4 ± 12.8 | ASA: 744, NR (98.2%) Clopidogrel: 742, NR (97.9%) | ASA: 531, NR (93.5%) Clopidogrel: 503, NR (88.6%) | 618 (81.5%) | 434 (76.4%) | 107 (86–133) | 105 (83–140) | 5000 IU | 5000 IU |
| Zijlstra et al. (2002)12 | Retrospective | The Netherlands | 1702 | 860 (50.5%) | 842 (49.5%) | 59.0 ± 11.0 | 61.0 ± 11.0 | ASA: 860, NR (100%) | ASA: 842, NR (100%) | 696 (80.9%) | 665 (79.0%) | 81 ± 43 | 26 ± 39 | NR | NR |
|
ASA, acetylsalicylic acid; IU, international units; NR, not reported; UFH, unfractionated heparin. |
|||||||||||||||
The aim of this study is to perform a systematic review and meta-analysis of existing studies on UFH pretreatment in the context of primary angioplasty as a reperfusion treatment for STEMI in terms of TIMI (Thrombolysis in Myocardial Infarction) grade 2-3 flow at the start of the procedure and early 30-day in-hospital mortality.
The meta-analysis follows PRISMA guidelines to ensure transparency and quality (table 2 of the supplementary data).
Table 2. Events from the studies
| Study | n | n (%) | Open artery: TIMI grade 2-3 flow | Major bleeding | 30-day mortality | ||||
|---|---|---|---|---|---|---|---|---|---|
| UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | UFH | Non-UFH | ||
| Fabris et al. (2022)10 | 537 | 237 (44.1%) | 300 (55.9%) | 113 (47.7%) | 87 (29.0%) | 5 (2.1%) | 6 (2.0%) | 23 (9.7%) | 28 (9.3%) |
| Emilsson et al. (2022)6 | 22 376 | 11 188 (50.0%) | 11 188 (50.0%) | 4233 (37.8%) | 3263 (29.2%) | 199 (17.8%) | 199 (17.8%) | 313 (2.8%) | 395 (3.5%) |
| Bloom et al. (2021)7 | 2746 | 1373 (50.0%) | 1373 (50.0%) | 178 (13.0%) | 128 (9.3%) | 19 (1.4%) | 26 (1.9%) | 41 (3.0%) | 48 (3.5%) |
| McGinley et al. (2020)8 | 1000 | 437 (43.7%) | 563 (56.3%) | 111 (25.4%) | 136 (24.2%) | 6 (1.4%) | 5 (0.9%) | 11 (2.5%) | 47 (8.3%) |
| Karlsson et al. (2019)11 | 7144 | 2898 (40.6%) | 4246 (59.4%) | 1075 (37.1%) | 1204 (28.3%) | 47 (1.6%) | 92 (2.2%) | 76 (2.6%) | 131 (3.1%) |
| Giralt et al. (2015)9 | 1326 | 758 (57.2%) | 568 (42.8%) | 229 (30.2%) | 120 (21.1%) | 9 (1.2%) | 6 (1.1%) | NR | NR |
| Zijlstra et al. (2002)12 | 1702 | 860 (50.5%) | 842 (49.5%) | 263 (30.6%) | 168 (20.0%) | 43 (5.0%) | 59 (7.0%) | 26 (3.0%) | 24 (2.9%) |
| Total | 36 831 | 17 751 (48.0%) | 19 080 (51.9%) | 6202 (31.6%) | 5106 (23.0%) | 328 (4.3%) | 393 (4.7%) | 490 (3.9%) | 673 (5.1%) |
|
NR, not reported; TIMI: Thrombolysis in Myocardial Infarction; UFH, unfractionated heparin. |
|||||||||
METHODS
Literature search
We conducted a systematic search of scientific literature across Medline-PubMed and the Cochrane Controlled Register of Trials (CENTRAL) from May through September 2024. We accessed several observational studies and clinical trials comparing UFH pretreatment in the ambulance vs no pretreatment in patients diagnosed with STEMI treated with primary angioplasty. A lower date limit was set to 2002, and no language restrictions were applied. Studies were selected if they included information on initial TIMI grade flow, 30-day early mortality, and major bleeding complications. In the article by Emilsson et al.6 data from the propensity score cohort, which provides better adjustment, were used, and the same population was used in the study by Bloom et al.7. The references of the selected studies were analyzed to obtain additional articles via cross-referencing. Both the search and article selection methodology are shown in figure 1.

Figure 1. Flowchart of the literature search. STEMI, ST-segment elevation myocardial infarction.
The PRISMA guidelines were followed (table 2 of the supplementary data), and the meta-analysis was registered in PROSPERO (CRD420250655362).
Inclusion criteria
We included observational, retrospective, and clinical trials analyzing the use of UFH as pretreatment in patients diagnosed with STEMI, administered at the first medical contact, in the ambulance or at a non-PCI-capable center prior to arrival at the destination hospital where the percutaneous coronary intervention (PCI) would be performed along with a control group of patients without UFH pretreatment. Moreover, studies had to provide information on initial TIMI grade flow, the 30-day mortality rate, and major bleeding complications. Only studies with a population of at least 500 individuals were included.
Exclusion criteria
We excluded repeated series from the same group, studies prior to 2002, those on pretreatment with anticoagulants other than UFH, studies without a control comparator group, or those that included patients diagnosed with non-ST-segment elevation acute coronary syndrome, angina, or another cardiac event different from STEMI. Studies with less than 500 individuals were also excluded.
Selection of publications
The article search was conducted across Medline-PubMed and CENTRAL databases using the following terms: “preclinical,” “cardiac,” “heparin,” “analysis, early,” “unfractionated,” “STEMI,” “prehospital,” and “pretreatment.” A total of 275 relevant articles were identified, from which, after initial exclusion based on inclusion and exclusion criteria, 16 were selected, and 7 finally remained6-12 (6 of them conducted in European populations and 1 in Australia.7) All were observational and retrospective studies, except for the one conducted by Karlsson et al.11, which is a subanalysis of a randomized clinical trial.
Primary and secondary endpoints
The primary endpoint was to analyze the association of UFH pretreatment with the presence of initial TIMI grade 2-3 flow in the infarct-related artery on diagnostic coronary angiography, prior to the start of PCI, in patients for whom PCI was indicated. The secondary endpoints were to analyze the association of UFH pretreatment with 30-day mortality in STEMI patients with an indication for PCI, and the presence of major bleeding complications13 (clinically significant bleeding events, such as bleeding requiring medical intervention or blood transfusion, or resulting in a significant hemoglobin decrease).
Data collection and management
Abstracts and methods sections of selected publications were systematically reviewed to ensure they met the inclusion criteria. Disagreements were resolved by consensus. Measures were taken to avoid duplication of articles.
Risk of bias
The risk of bias in the studies included in the meta-analysis was assessed using a combination of robust statistical approaches and widely recognized visual methods. The Harbord test (table 3 of the supplementary data), specifically designed to detect publication bias in meta-analyses reporting risk ratios (RR), was used. Additionally, funnel plots were analyzed, allowing a visual assessment of asymmetry in the distribution of study effects. The funnel plots for each variable are included in figures 1-3 of the supplementary data.
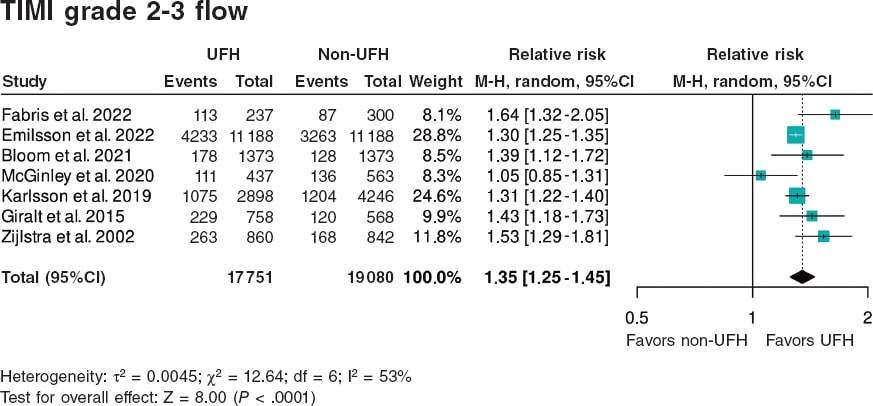
Figura 2. Forest plot of the prevalence of TIMI grade 2-3 flow. References cited in this figure: Fabris et al.10, Emilsson et. al.6, Bloom et al.7, McGinley et al.8, Karlsson et al.11, Giralt et al.9, and Zijlstra et al.12. 95%C, 95% confidence interval; M-H, Mantel-Haenszel’s method; UFH, unfractionated heparin.
In this meta-analysis, the variables of interest include TIMI grade 2-3 flow, 30-day mortality, and major bleeding. Furthermore, their potential bias was analyzed using the above-mentioned statistical procedures.
Statistical analysis
For statistical analysis, version 4.2.1 of R was used, using the metabin function from the meta package to synthesize the results of studies comparing UFH pretreatment vs UFH administered in the cath lab. Binary event data and totals for each group were analyzed using the RR model, with the inverse variance method, which weights studies based on precision, giving more weight to those with lower variance. A forest plot was generated using a random-effects model; the graph shows point estimates and corresponding 95% confidence intervals (95%CI) for each individual study, along with an overall RR estimate. The graph design followed the RevMan format, with customized labels indicating the groups of interest (UFH and non-UFH) and direction of effects (favors UFH and favors non-UFH), improving clinical interpretation. Heterogeneity analysis included calculation of the I2 value, which quantifies the proportion of variability among studies not attributable to chance, due to observed heterogeneity. As indicated by the τ2 value from the Harbord test analysis (table 3 of the supplementary data), the random-effects model is most appropriate in this situation.
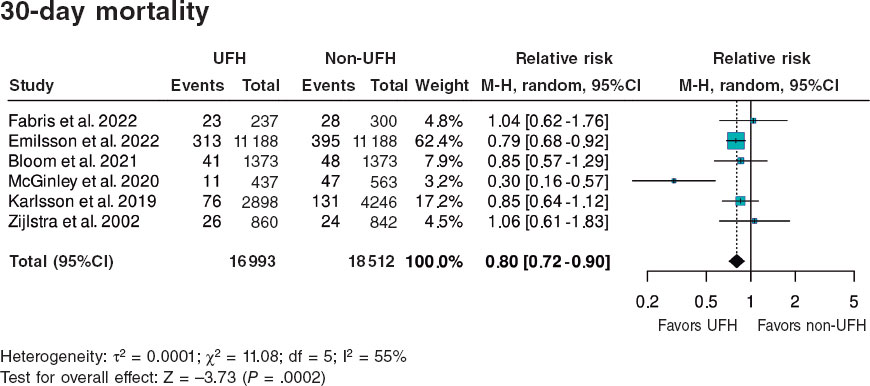
Figure 3. Forest plot of the prevalence of 30-day mortality. References cited in this figure: Fabris et al.,10 Emilsson et al.,6 Bloom et al.,7 McGinley et al.,8 Karlsson et al.,11 Giralt et al.,9 and Zijlstra et al.12. 95%C, 95% confidence interval; M-H, Mantel-Haenszel’s method; UFH, unfractionated heparin.
RESULTS
A total of 36 831 patients were included, of whom 17 751 (48.2%) received pretreatment with UFH and 19 080 (51.8%) did not, the latter representing the control group for comparison. Of note, data from the article by Emilsson et al.6 were obtained from the propensity score-matched cohort, which provides better adjustment; therefore, the study population was 22 376 rather than 41 631 patients. Additionally, this adjusted cohort was used in the study by Bloom et al.7 with 2746 instead of 4720 patients. The data shown in table 1 correspond to the propensity score-matched cohort and include a summary of the demographics and characteristics of each study. A substantial portion of the population was male (70–80% of the total), with mean ages ranging from 60 to 67 years. Only 5 of the 7 studies reported the UFH dose, which ranged from 4000 to 5000 IU.
Primary endpoint
A total of 6202 (31.6%) patients pretreated with UFH achieved TIMI grade 2-3 flow vs 5106 (23.0%) from the non-pretreated group (table 2).
The meta-analysis of data from the 7 studies6-12 demonstrated a significant increase in the likelihood of TIMI grade 2-3 flow, with a hazard ratio (HR) of 1.35 (95%CI, 1.25–1.45; P < .0001) (figure 2). Although all studies showed statistically significant differences, except for the one by McGinley et al.8, heterogeneity in the magnitude of association was high (I2 = 53%).
Secondary endpoints
A total of 490 (3.9%) patients pretreated with UFH died within 30 days vs 673 (5.1%) from the non-pretreated group (table 2). The meta-analysis of data from the 7 included studies6-12 showed a reduction in 30-day mortality in patients who received pretreatment with UFH (HR, 0.80; 95%CI, 0.72–0.90; P = .0002) vs those who did not. Two studies showed a significantly lower mortality rate in the UFH group individually, including the one with the largest sample size6 (65.8% of patients included in the meta-analysis). Heterogeneity in the magnitude of association was high (I2 = 55%) (figure 3).
Regarding the association between UFH pretreatment and the rate of hemorrhagic complications, there were no significant associations in the meta-analysis of the 7 studies6-12 (HR, 0.87; 95%CI, 0.72–1.05; P = .1502). None of the studies showed a significant association, either beneficial or harmful, regarding bleeding complications. Heterogeneity among the studies was low (I2 = 0%) (figure 4).
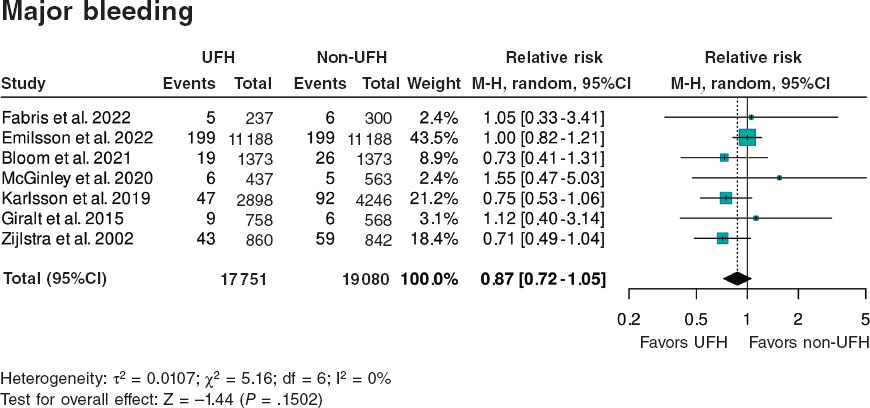
Figure 4. Forest plot of the prevalence of major bleeding. References cited in this figure: Fabris et al.,10 Emilsson et al.,6 Bloom et al.,7 McGinley et al.,8 Karlsson et al.,11 Giralt et al.,9 and Zijlstra et al.12. 95%C, 95% confidence interval; M-H, Mantel-Haenszel’s method; UFH, unfractionated heparin.
DISCUSSION
This meta-analysis demonstrates that for STEMI patients, administering UFH as pretreatment at the point of first medical contact is more beneficial than doing so at the PCI-capable center.
The observed benefit consists of a higher percentage of initial TIMI grade 2-3 flow (absolute increase of 8.6% and relative increase od 37.4%) and a lower 30-day mortality rate (absolute reduction of 1.2% and relative reduction of 23.5%). While most studies individually indicated a benefit of UFH pretreatment for open arteries, only 2 of the 7 studies primarily supported a mortality benefit. In terms of safety, pretreatment at first medical contact had a neutral effect on the risk of bleeding complications, and results were homogeneous across all 7 studies.
A recently published meta-analysis of 14 studies14 with different inclusion criteria and endpoints, incorporated studies on UFH and on a mix of other anticoagulants, such as low molecular weight heparin (enoxaparin), bivalirudin, and fondaparinux, along with additional events like cardiogenic shock, in-hospital mortality, and 1-year mortality. Both analyses showed consistent results on the benefit of pretreatment on open artery rates and early mortality, although they differed in the rate of bleeding complication. The referenced meta-analysis14 found a beneficial association between pretreatment with UFH or fractionated heparin in the reduction of bleeding complications. Moreover, the meta-analysis also analyzed the impact of pretreatment on the percentage of patients with cardiogenic shock, showing a positive association between pretreatment with UFH or fractionated heparin and this outcome. Of note, the heterogeneity in design, timing, and concomitant antiplatelet therapy among the studies included in the 2 meta-analyses. Notably, a small observational study conducted in Spain reported benefits from UFH pretreatment.15
Arguments for and against UFH pretreatment in STEMI
UFH is inexpensive, accessible, administered intravenously, and widely used in health care centers and ambulances. UFH is a necessary drug to prevent arterial and catheter thrombosis during PCI.
Beyond the potentially beneficial effects on open artery rates demonstrated in the meta-analysis, the use of UFH as pretreatment at the first medical contact does not seem to influence PCI per se. The rate of arterial puncture-related complications in anticoagulated patients is low when radial access is used; according to recent studies on the STEMI Code in Spain, 90% of angioplasties in STEMI patients are performed via radial access.4,5 There is still no information available on the potential impact of pretreatment on thrombus burden, no-reflow, ST-segment resolution, or infarct size, and no current studies have been designed to address these specific issues3 (table 4 of the supplementary data).
Clinical practice guidelines do not make definitive recommendations either due to the absence of adequately randomized trials evaluating the value of UFH pretreatment—not because there is evidence of no effect.1,3
In some patients misdiagnosed with STEMI (eg, those with aortic syndrome, pericarditis, myocarditis, NSTEMI, transient ST-segment elevation, Takotsubo syndrome, pulmonary embolism, pneumothorax, thoracic or esophageal disease, or musculoskeletal chest pain), pretreatment with UFH and antiplatelets may be harmful.
Notably, recent studies on the STEMI Code in Spain4-5 report that in 16.6% of all STEMI Code activations, the diagnosis of STEMI could not be confirmed, and in 3.6% of cases, no angioplasty was performed.
These misdiagnoses were not analyzed in the included meta-analyses. The design of the studies, most of which were retrospective, complicates the identification of risks associated with UFH use in these contexts. Theoretically, UFH pretreatment might be more beneficial in patients with recent thrombus formation, shorter times from symptom onset to first medical contact, and longer transfers to the PCI-capable center. However, in this meta-analysis, the review of study characteristics does not allow conclusions in this regard. There was no evident relationship between time metrics and the use of UFH pretreatment and the rates of open arteries or short-term mortality.
Need for randomized clinical trials
Clinical practice guidelines have become key reference documents for organizing health care delivery.1,2 These guidelines, developed by international experts who thoroughly review the scientific evidence to support their recommendations, are not always implemented in the routine clinical practice. One example, relevant to our field, is the use of antiplatelet pretreatment at the first medical contact. One year after the publication of the European Society of Cardiology guidelines on the management of acute coronary syndrome,1 which assigned a class IIb recommendation and level B evidence to dual antiplatelet therapy (DAPT) in STEMI, nearly all hospitals in Spain continued to administer DAPT at the first medical contact (table 1 of the supplementary data).
The current recommendation against antiplatelet pretreatment, similarly to the indication on pretreatment with UFH, is based on the absence of evidence demonstrating a benefit from DAPT and concerns on the potential bleeding risk associated with the use of long half-life antiplatelet agents in patients who may require emergency revascularization surgery.16-18 However, the need for emergency surgery is extremely rare in STEMI cases. Implementation of the clinical practice guidelines and reducing pretreatment to a single antiplatelet agent has been adopted in other European countries with preliminary positive results (EuroPCR 2024 presentation).19 In countries such as Denmark and Germany, and certain regions of Italy, STEMI care protocols include the administration of a single antiplatelet agent (acetylsalicylic acid) along with UFH.20 Despite the absence of a clear recommendation regarding UFH in the guidelines, it can be inferred that protocol developers trust in the theoretically beneficial effect of UFH, complementing antiplatelet therapy at the time of the first medical contact.
Study limitations
This study has inherent limitations related to its design. Observational studies, especially retrospective ones, are susceptible to various biases, including selection and confounding, as well as uncontrolled factors that may affect internal validity. However, several measures were taken to mitigate these biases and provide a robust interpretation of the findings, including a detailed sensitivity analysis to assess result consistency. Moreover, heterogeneity was explored using the Harbord test, which yielded high p-values for publication bias, indicating no significant evidence of such bias influencing our results. Despite this, heterogeneity remains an inherent challenge in meta-analyses that include observational studies with varying designs and quality. This variability was documented using measures such as τ2 and considered in interpreting the findings.
Despite these limitations, the results remain valuable and should be interpreted with caution.
Another limitation is the heterogeneity in the number of patients included in the selected studies, the times for care and transfer, the doses of UFH administered, the definition of hemorrhagic complications, and the concomitant antiplatelet regimens used, all of which may have introduced bias.
CONCLUSIONS
The meta-analysis of retrospective studies and one clinical trial shows that pretreatment with UFH in patients with STEMI undergoing a primary angioplasty is associated with an increase in the initial TIMI grade 2-3 flow and a lower early mortality rate (figure 5).
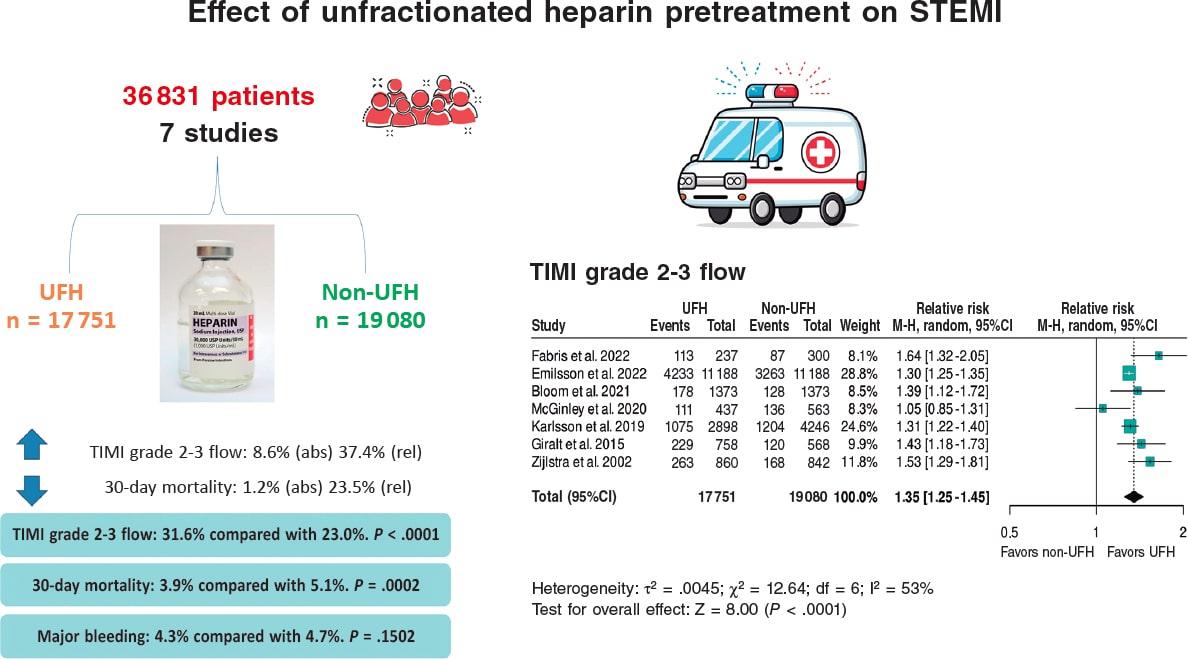
Figura 5. Effect of unfractionated heparin pretreatment in patients with ST-segment elevation myocardial infarction (STEMI). Forest plot of the prevalence of TIMI grade 2-3 flow. References cited in this figure: Fabris et al.10, Emilsson et al.6, Bloom et al.7, McGinley et al.8, Karlsson et al.11, Giralt et al.9, and Zijlstra et al.12. 95% CI: 95% confidence interval, M-H: Mantel-Haenszel’s method, UFH: unfractionated heparin.
Specifically designed clinical trials are needed to establish the impact of early UFH administration, and current clinical practice guidelines should provide clearer recommendations on the optimal timing of UFH pretreatment in STEMI patients.
FUNDING
This work was funded by CIBERCV CB16/11/00385.
ETHICAL CONSIDERATIONS
Ethical considerations are not applicable to a meta-analysis, as no direct clinical data from individuals are collected and therefore ethics committee evaluation is deemed unnecessary. A subgroup analysis by sex was not performed because it would result in a loss of statistical power, and both women and men were represented. There is no prior evidence or data suggesting that men and women respond differently to IV heparin anticoagulant treatment.
STATEMENT ON THE USE OF ARTIFICIAL INTELLIGENCE
Artificial intelligence was not used.
AUTHORS’ CONTRIBUTIONS
M. Roldán Medina and A. Riquelme Pérez equally contributed to various phases of the study: study conception and design, data acquisition, analysis, and interpretation. Additionally, M. Roldán Medina contributed to drafting the original manuscript and editing and reviewing the final version, while A. Riquelme López was responsible for the final revision of the article.
R. López-Palop and P. Carrillo contributed to data acquisition, analysis, and interpretation, and to the final text review and editing. J. Lacunza participated in data acquisition, analysis, and interpretation. R. Valdesuso contributed to data acquisition, analysis, and interpretation.
J. García de Lara was involved in data acquisition, analysis, interpretation, and final text review and editing. J. Hurtado-Martínez contributed to data acquisition, analysis, and interpretation. J.M. Durán contributed to data acquisition, analysis, and interpretation. E. Pinar-Bermúdez participated in data acquisition, analysis, and interpretation. J.R. Gimeno and D. Pascual-
CONFLICTS OF INTEREST
None declared.
ACKNOWLEDGMENTS
The authors would like to thank all colleagues from the Cardiology Department at Hospital Virgen de la Arrixaca, IMIB, and Universidad de Murcia whose collaboration made this study possible.
WHAT IS KNOWN ABOUT THE TOPIC?
- The early administration of unfractionated heparin (UFH) in ST-segment elevation myocardial infarction (STEMI) is controversial. Current clinical practice guidelines leave the timing of its administration before primary angioplasty to the physician’s discretion and do not provide clear recommendations on UFH pretreatment in STEMI patients prior to their arrival at the PCI-capable center.
WHAT DOES THIS STUDY ADD?
- Our meta-analysis and systematic review of studies on the safety and efficacy profile of UFH pretreatment in STEMI patients, compared with control patients who did not receive such pretreatment, demonstrates that pretreatment with UFH was associated with an increased TIMI grade 2-3 flow, a lower 30-day mortality rate, and fewer major bleeding events.
REFERENCES
1. Byrne RA, Rossello X, Coughlan JJ, et al. 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J Acute Cardiovasc Care. 2024;13:55-161. Erratum in:Eur Heart J Acute Cardiovasc Care. 2024;13:455
2. Lawton JS, Tamis-Holland JE, Sripal Bangalore, et al. 2021 ACC/AHA/SCAI Guideline for Coronary Artery Revascularization.J Am Coll Cardiol. 2022;79:197-215.
3. Collet J, Zeitouni M. Heparin pretreatment in STEMI:is earlier always better?EuroIntervention. 2022;18:697-699.
4. Rodríguez-Leor O, Cid-Álvarez AB, Moreno R, et al. Regional differences in STEMI care in Spain. Data from the ACI-SEC Infarction Code Registry. REC Interv Cardiol. 2023;5:118-128.
5. Rodríguez-Leor O, Cid-Álvarez AB, Pérez de Prado A, et al. Analysis of the management of ST-segment elevation myocardial infarction in Spain. Results from the ACI-SEC Infarction Code Registry. Rev Esp Cardiol. 2022;75:669-680.
6. Emilsson O, Bergman S, Mohammad M, et al. Pretreatment with heparin in patients with ST-segment elevation myocardial infarction:a report from the Swedish Coronary Angiography and Angioplasty Registry (SCAAR). EuroIntervention. 2022;18:709-718.
7. Bloom J, Andrew E, Nehme Z, et al. Pre-hospital heparin use for ST-elevation myocardial infarction is safe and improves angiographic outcomes. Eur Heart J Acute Cardiovasc Care. 2021;10:1140-1147.
8. McGinley C, Mordi I, Kell P, et al. Prehospital Administration of Unfractionated Heparin in ST-Segment Elevation Myocardial Infarction Is Associated With Improved Long-Term Survival. J Cardiovasc Pharmacol. 2020;76:159-163.
9. Giralt T, Carrillo X, Rodriguez-Leor O, et al. Time-dependent effects of unfractionated heparin in patients with ST-elevation myocardial infarction transferred for primary angioplasty. Int J Cardiol. 2015;198:70,-74.
10. Fabris E, Menzio S, Gregorio C, et al. Effect of prehospital treatment in STEMI patients undergoing primary PCI. Catheter Cardiovasc Interv. 2022;99:1500-1508.
11. Karlsson S, Andell P, Mohammad M, et al. Editor's Choice —Heparin pre-treatment in patients with ST-segment elevation myocardial infarction and the risk of intracoronary thrombus and total vessel occlusion. Insights from the TASTE trial. Eur Heart J Acute Cardiovasc Care. 2019;8:15-23.
12. Zijlstra F, Ernst N, de BoerMJ, et al. Influence of prehospital administration of aspirin and heparin on initial patency of the infarct-related artery in patients with acute ST elevation myocardial infarction. J Am Coll Cardiol. 2002;39:1733-1737.
13. Mehran R, Rao S, Bhatt D, et al. Standardized bleeding definitions for cardiovascular clinical trials:a consensus report from the Bleeding Academic Research Consortium. Circulation. 2011;123:2736-2747.
14. Costa G, Resende B, Oliveiros B, Gonçalves L, Teixeira R. Heparin pretreatment in ST segment elevation myocardial infarction:a systematic review and meta-analysis. Coron Artery Dis. 2025;36:28-38.
15. Ariza A, Ferreiro JL, Sánchez-Salado JC, Lorente V, Gómez-Hospital JA, Cequier A. Early Anticoagulation May Improve Preprocedural Patency of the Infarct-related Artery in Primary Percutaneous Coronary Intervention. Rev Esp Cardiol. 2013;66:148-150.
16. Koul S, Smith J, Götberg M, et al. No Benefit of Ticagrelor Pretreatment Compared With Treatment During Percutaneous Coronary Intervention in Patients With ST-Segment-Elevation Myocardial Infarction Undergoing Primary Percutaneous Coronary Intervention. Circ Cardiovasc Interv. 2018;11:e005528.
17. Russo RG, Wikler D, Rahimi K, Danaei G. Self-Administration of Aspirin After Chest Pain for the Prevention of Premature Cardiovascular Mortality in the United States:A Population-Based Analysis. J Am Heart Assoc. 2024;13:e032778.
18. Chen ZM, Jiang LX, Chen YP, et al. Addition of clopidogrel to aspirin in 45 852 patients with acute myocardial infarction:randomised placebo-controlled trial. Lancet. 2005;366:1607-1621.
19. Siller J, Angiolillo D, De Luca L, Rymer J, Thim T, Zeymer U. Real-world practice adoption of latest guidelines for the acute management of ACS patients. En:Paris 2024. EuroPCR Course 2024. 35th edition;2024 May 21-24;Paris, France. Available at:https://www.pcronline.com/Courses/EuroPCR. Consulted 1 Mar 2025.
20. De Luca L, Maggioni A, Cavallini C, et al. Clinical profile and management of patients with acute myocardial infarction admitted to cardiac care units:The EYESHOT-2 registry. Int J Cardiol. 2025;418:132601.
- Angiography-derived index versus fractional flow reserve for intermediate coronary lesions: a meta-analysis review
- Functional assessment in acute coronary syndrome: a systematic review of acute versus staged interventions
- Prognostic value of global plaque volume calculated from the 3D reconstruction of the coronary tree in patients without significant coronary artery disease. A multicenter study
- Long-term prognostic impact of the left anterior descending coronary artery as the STEMI-related culprit vessel: subanalysis of the EXAMINATION-EXTEND trial
Interviews
An interview with Bruno Scheller
aServicio de Cardiología, Hospital Universitario de La Princesa, Instituto de Investigación Sanitaria de La Princesa (IIS-IP), Universidad Autónoma de Madrid, Spain
bCentro de Investigación Biomédica en Red de Enfermedades Cardiovasculares (CIBERCV), Instituto de Salud Carlos III, Madrid, Spain












