CASE PRESENTATION
Prosthetic valve thrombosis (PVT) is a complication associated with a high morbimortality rate. Yet despite anticoagulation, the rate of PVT is between 0.5% and 8%.1 The management of this disease depends on various factors like the size and location of the thrombus, the degree of valvular obstruction or dysfunction, the symptoms at presentation, and the patient’s hemodynamic status. Therapeutic options include surgery and fibrinolysis. Both have given good results, but they are not always effective and are associated with a high risk of complications.
This is the case of a 55-year-old woman with rheumatic myocardiopathy treated with aortic and mitral valve replacement using the bidisco ATS 27 mechanical heart valve (Medtronic ATS Medical, Inc, Plymouth, Minnesota, United States) and Sorin Overline 29 device (Sorin Biomedica Cardio SpA, Saluggia, Italy), respectively. The patient granted consent to publish her case, respecting her right to privacy and the protection of personal data. Two months after surgery the patient was showing signs of dyspnea (New York Heart Association functional class III) and she was diagnosed with obstructive thrombosis of the prosthetic mitral valve. The transesophageal echocardiography (TEE) performed revealed the presence of a mass compatible with a thrombus attached to the atrial side of the valve. Both discs were blocked in an intermediate position causing severe stenosis and mitral regurgitation. The patient was treated with surgery with extraction of the thrombotic material and left atrial appendage occlusion. The transthoracic echocardiography performed after the surgery confirmed the normal movement of the valve. The patient was discharged without symptoms on oral anticoagulation and acetylsalicylic acid (100 mg/day).
Although anticoagulation was kept within the recommended range (INR, 3-3.5), 3 months later the patient was re-admitted with signs of dyspnea (New York Heart Association functional class III). The TEE revealed the presence of an increased mean mitral gradient (18 mmHg). The anterior disc was blocked in the closed position, but the other one moved normal and with no signs of significant mitral regurgitation. The TEE also revealed the presence of a highly mobile, linear, thin mass (less than 1 mm) compatible with a Lambl’s excrescence attached to the atrial side of the valve. Also, there were slightly mobile, echo-dense, and sessile masses (maximum diameter, 4 mm; area, 0.29 cm2) compatible with thrombi and attached to the atrial side of the valve.
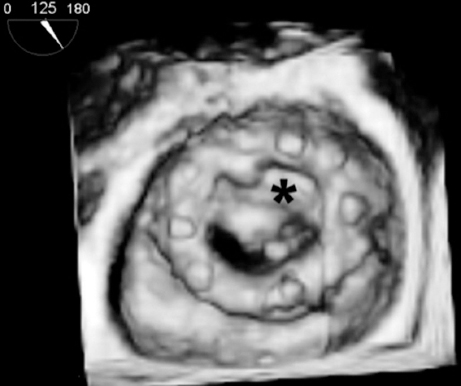
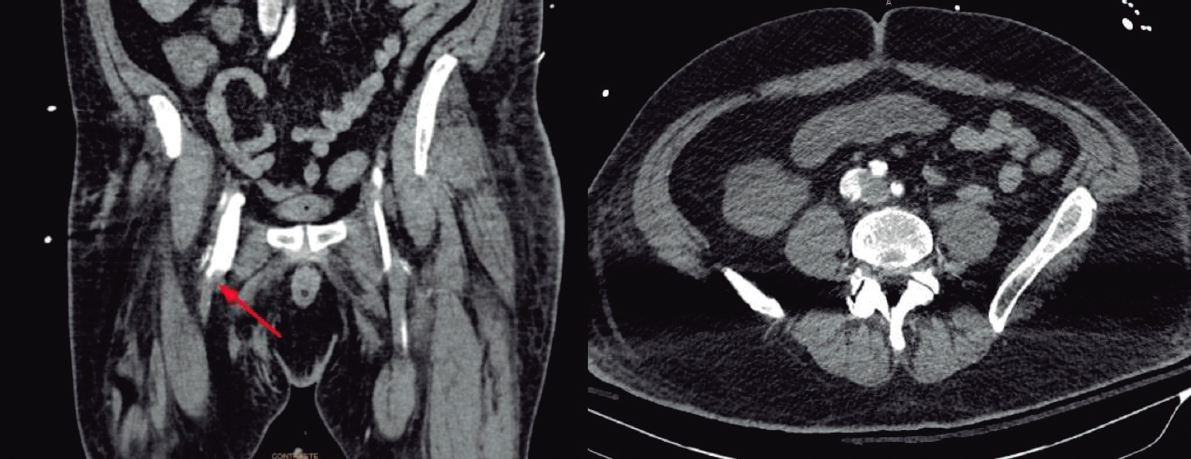
The patient was treated with IV thrombolysis with alteplase followed by 48 hours of IV infusion of unfractionated heparin. The new TEE performed after fibrinolysis revealed the presence of small residual thrombi (maximum diameter, 3 mm; area, 0.17 cm2) and persistent fixation of the anterior disc in the closed position (figure 1).
Figure 1. Mitral valve prior to the intervention with a blocked anterior disc in the close position (asterisk).
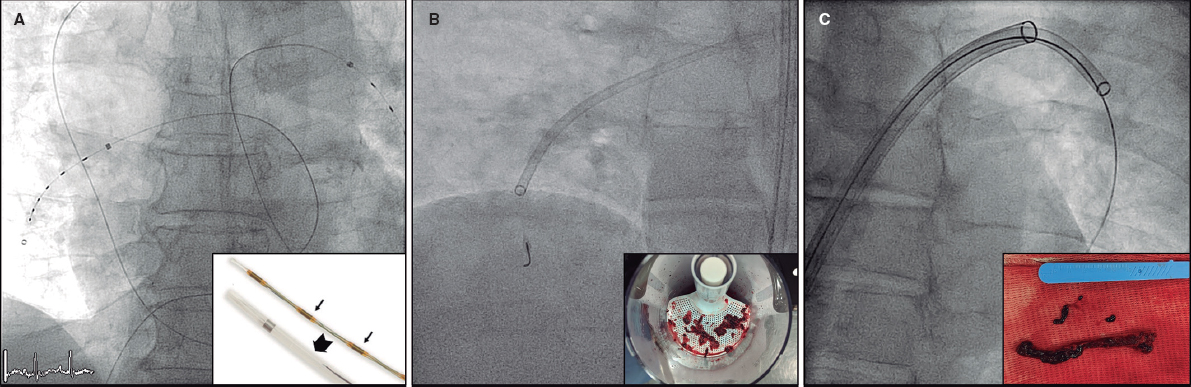
After the failed fibrinolysis attempt and given the high risk for a new surgery, the percutaneous manipulation of the valve was decided as the therapeutic option.
FUNDING
No funding was received for this work.
CONFLICTS OF INTEREST
None declared.
REFERENCES
1. Cáceres-Lóriga FM, Pérez-López H, Santos-Gracia J, Morlans-Hernandez K. Prosthetic heart valve thrombosis:pathogenesis, diagnosis and management. Int J Cardiol. 2006;110:1-6.
Corresponding author: Unidad de Hemodinámica, Servicio de Cardiología, Hospital Universitario La Ribera, Carretera de Corbera km 1, 46600 Alzira, Valencia, Spain.
E-mail address: pomar_fra@gva.es (F. Pomar Domingo).