To the Editor,
Transcatheter aortic valve implantation (TAVI) is a therapeutic alternative that has proven safe and effective across different clinical settings. Over the last few years, more and more cases of «emergency TAVI» have been reported.1-2 Currently, this term is often used for those implantation procedures performed during admission due to decompensated heart failure although this concept includes very different situations. The therapeutic option to treat cardiogenic shock should be «emergency TAVI», that is, implantation performed within the first 72 hours after admission.3 This is the case of a patient with severe aortic stenosis who was transferred to our center with signs of cardiogenic shock.
This is the case of a 67-year-old man. The patient was a former smoker and a regular drinker. Initially, he had been admitted to a different center with early signs of heart failure. Arterial pressure at admission was 120/90 mmHg with global congestion and need for low-flow oxygen therapy. Diuretic treatment was started, and the echocardiogram revealed the presence of severe aortic stenosis with left systolic dysfunction. The patient had signs of liver (alanine aminotransferase, aspartate aminotransferase, and bilirubin levels of 1244 u/L, 1808 u/L, and 2 mg/dL, respectively, and normalized international ratio of 2), and renal failure (creatinine levels of 2.01 mg/dL), and arterial lactate levels of 2.8 mmol/L. Cardiac markers were high (N-terminal B-type natriuretic propeptide, and high-sensitivity troponin I levels of 6753 pg/mL, and 468-450 ng/mL, respectively). Given the progressive worsening of the patient, transfer to our center cardiac surgery intensive care unit was decided. After the patient’s arrival, cardiac catheterization was performed with a Swan-Ganz catheter. It revealed:
- – Pulmonary artery and aortic saturation of 56% and 98%, respectively (nasal cannula at 2L).
- – Pressure: right atrium, 16 mmHg; pulmonary artery, 55/35/42 mmHg; pulmonary capillary wedge pressure, 32 mmHg; aorta, 110/80/90 mmHg.
- – Cardiac output (thermodilution): 2.8 L/min.
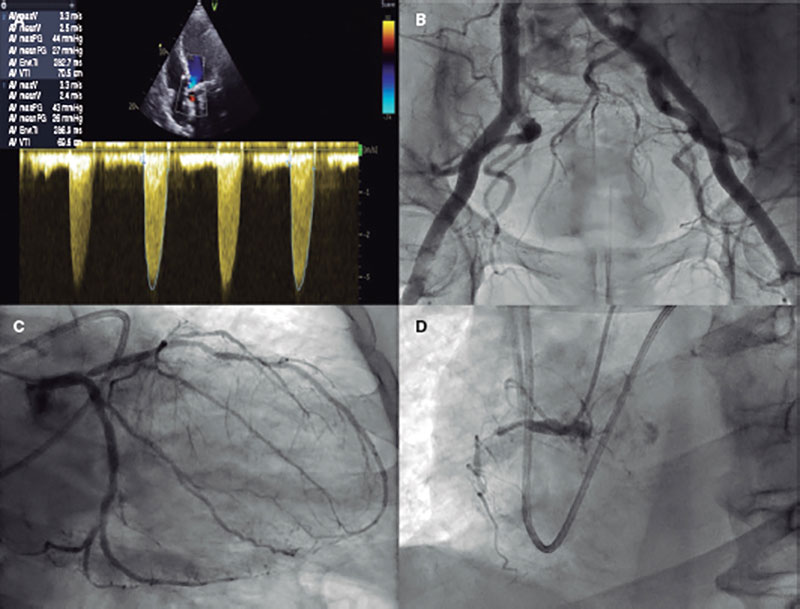
The echocardiogram confirmed the presence of a left ventricular ejection fraction of 10% with moderate mitral regurgitation (video 1 of the supplementary data) and severe aortic stenosis (figure 1A). The levels of arterial lactate upon the patient’s arrival were 3.6 mmol/L. Given the situation of normotensive cardiogenic shock, inotropic treatment with dobutamine (up to 12 mcg/kg/min) was initiated. It improved cardiac index up to 2.2 L/min/m2 and brought lactate levels back to normal within the first 8 hours after admission. A computed axial tomography (that same afternoon) and coronary angiography (the next morning, figure 1B) were performed. The screening results obtained were favorable for transcatheter aortic valve implantation:
- – Tricuspid aortic valve. Coronary artery calcium score, 2100.
- – Aortic annulus: perimeter, 88 mm; area, 556 mm2.
- – Sinus segment: 35 mm x 33 mm x 33 mm.
- – Distance between annulus and left main coronary artery: 11 mm; to right coronary artery, 17 mm.
- – Significant lesion to the ostial left anterior descending coronary artery with distal TIMI-grade 3 flow (Thrombolysis in Myocardial Infarction) and no data suggestive of complications. Chronic total coronary occlusion of right coronary artery.
- – Calcified femoral accesses without significant lesions and proper caliber.
Figure 1. A: continuous-wave Doppler echocardiography at aortic valve level. B: femoral angiography. C: significant lesion to the ostial left anterior descending coronary artery with distal TIMI-grade 3 flow and no data suggestive of complications. D: chronic total coronary occlusion of right coronary artery.
When multi-organ failure recovered, and hemodynamic data collected with the Swan-Ganz catheter came back to normal, the heart team recommended «emergency TAVI» given the situation of cardiogenic shock, and management of coronary artery disease was deferred and treated in a second surgical act.
The patient was intubated before the procedure. After predilatation with a 25 mm balloon, a 34 mm Evolut PRO valve (Medtronic, United States) was implanted via left femoral artery in the cusp-overlap view to optimize commissural alignment and minimize damage to the conduction system. Final outcomes were excellent without gradient or residual aortic regurgitation. The patient showed transient left bundle branch block, which is why atrial pacing stress echocardiography was conducted that did not reach the Wenckebach point at 130 beats per minute, which is why the electrocatheter was eventually removed. Left femoral artery was closed with 2 Perclose Proglide sutures as the good results seen on the angiography confirmed (video 2 of the supplementary data). Hemodynamic improvement was immediate. The patient was progressively weaned off dobutamine and extubated early. Prognostic benefit treatment was optimized, and the cardiac magnetic resonance imaging showed a left ventricular ejection fraction of 28% with viability in the entire myocardium. The patient was discharged 2 weeks after admission for close follow-up, and to plan outpatient coronary revascularization.
This case exemplifies the delicate balance between the time when the cause for the shock was corrected and the hemodynamic stabilization and optimization of organ perfusion was achieved. A recent review and meta-analysis found no differences whatsoever between emergency and elective implantation. However, the rate of acute kidney injury was higher3; due to the severity of these patients, the 1-month mortality rate after emergency implantation is twice as high compared to elective implantation (8.8% vs 4.4%). If only patients with cardiogenic shock are considered, the 1-month mortality rate is higher (11.8% up to 33.3%).4-5 In conclusion, we believe that «emergency TAVI» is a therapeutic alternative associated with good clinical outcomes.
FUNDING
None whatsoever.
AUTHORS’ CONTRIBUTIONS
Manuscript drafting: J. García-Carreño, I. Sousa-Casasnovas, J. Martínez-Solano, J. Elízaga-Corrales, F. Fernández-Avilés, and M. Martínez-Sellés. Image and video aquisition: J. García-Carreño, and J. Martínez-Solano. F. Fernández-Avilés, and M. Martínez-Sellés contributed to this article similarly.
CONFLICTS OF INTEREST
None reported.
SUPPLEMENTARY DATA
Vídeo 1. García-Carreño J. DOI: 10.24875/RECICE.M22000336
Vídeo 2. García-Carreño J. DOI: 10.24875/RECICE.M22000336
REFERENCES
1. Kolte D, Khera S, Vemulapalli S, et al. Outcomes Following Urgent/Emergent Transcatheter Aortic Valve Replacement: Inisights From the STS/ACC TVT Registry. JACC Cardiovasc Interv. 2018;11:1175-1185.
2. Elbadawi A, Elgendy IW, Mentias A, et al. Outcomes of urgent versus nonurgent transcatheter aortic valve replacement. Catheter Cardiovasc Interv. 2020;96:189-195.
3. Aparisi A, Santos-Martínez S, Delgado-Arana JR, et al. Resultados del TAVI emergente comparado con el procedimiento electivo: metanálisis. REC Interv Cariol. 2021;3:166-174.
4. Fraccaro C, Tekes RC, Tchétché D, et al. Transcatheter aortic valve implantation (TAVI) in cardiogenic shock: TAVI-shock registry adults. Catheter Cardiovasc Interv. 2020;96:1128-1135.
5. Frerker C, Schewel J, Schlüter M, et al. Emergency transcatheter aortic valve replacement in patients with cardiogenic shock due to acutely decompensated aortic stenosis. Eurointervention. 2016;11:1530-1536.