ABSTRACT
Introduction and objectives: This is the 2021 annual activity report from the Interventional Cardiology Association of the Spanish Society of Cardiology (ACI-SEC), and the Interventional Working Group of the Spanish Society of Pediatric Cardiology (GTH-SECPCC).
Methods: All Spanish centers with cath lab capabilities and interventional activity in congenital heart diseases were invited to participate. Data were collected online, analyzed by an external company, and ACI-SEC and GTH-SECPCC members.
Results: A total of 16 centers participated—15 public and 1 private—including 34 cath labs with experience in congenital heart diseases, 7 of them (20.5%) exclusively dedicated to pediatric patients. A total of 1094 diagnostic studies (4.5% more than 2020) and 1553 interventional catheterizations (5.8% more than 2020) were registered. The most common procedures were atrial septal defect closure (336 cases), pulmonary branch artery angioplasty (231 cases), and percutaneous closure of the patent ductus arteriosus (228 cases). Interventional procedures were considered successful in 95% of the cases with rates of major procedural complication and in-hospital mortality of 2.7% and 0.2%, respectively.
Conclusions: This is the second Spanish Cardiac Catheterization in Congenital Heart Diseases Registry report. A significant increase of diagnostic and interventional procedures was reported with a special increase of percutaneous valve implantation, ductus arteriosus closure, and aortic angioplasty. Most interventional techniques continue to demonstrate excellent safety and efficacy outcomes.
Keywords: Congenital heart disease Cardiac catheterization Atrial septal defect Percutaneous valve implantation
RESUMEN
Introducción y objetivos: La Asociación de Cardiología Intervencionista de la Sociedad Española de Cardiología (ACI-SEC) y el Grupo de Trabajo de Hemodinámica de la Sociedad Española de Cardiología Pediátrica y Cardiopatías Congénitas (GTH-SECPCC) presentan su informe anual de actividad hemodinámica en cardiopatías congénitas correspondiente al año 2021.
Métodos: Se invitó a participar a los centros españoles con laboratorio de hemodinámica y actividad intervencionista en cardiopatías congénitas. La recogida de datos fue telemática y su análisis lo efectuó una empresa externa junto con miembros de la ACI-SEC y el GTH-SECPCC.
Resultados: Participaron 16 centros (15 públicos y 1 privado) que acumulan 34 salas de hemodinámica con actividad en cardiopatías congénitas, 7 (20,5%) de ellas con dedicación exclusiva a pacientes pediátricos. Se registraron 1.094 estudios diagnósticos (5,1% más que en 2020) y 1.553 cateterismos intervencionistas (6,4% más que en 2020). Las técnicas más frecuentes fueron el cierre de comunicación interauricular (336 casos), la angioplastia de ramas pulmonares (231 casos) y el cierre de ductus (228 casos). Respecto al año anterior se incrementaron significativamente las técnicas de implantación de válvulas percutáneas (29,3%), cierre de ductus (20,6%) y angioplastia aórtica (12,8%). La tasa de éxito en los procedimientos intervencionistas fue del 95%, con una tasa de complicaciones mayores del 2,7% y una mortalidad intrahospitalaria del 0,2%.
Conclusiones: Este trabajo es la segunda publicación del Registro Español de Intervencionismo en Cardiopatías Congénitas. Se ha constatado un aumento significativo de los procedimientos diagnósticos y terapéuticos, destacando el incremento en la implantación de válvulas percutáneas, el cierre de ductus y la angioplastia aórtica. La mayoría de las técnicas intervencionistas siguen demostrando excelentes datos de seguridad y eficacia.
Palabras clave: Cardiopatías congénitas Cateterismo cardiaco Comunicación interauricular Implantación de válvula percutánea
INTRODUCTION
The collaborative effort which was initiated in 2019 by the Interventional Cardiology Association of the Spanish Society of Cardiology and the Interventional Working Group of the Spanish Society of Pediatric Cardiology (GTH-SECPCC) has reactivated and continued the management and improvement of a Spanish registry of interventional procedures in patients with congenital heart diseases of all ages. The previous report that included the activity from 2020 was the first one to be published.1
The current report, analyzed in this article dealing with the activity displayed in 2021, assesses for the very first time, the progression of volume and results of transcatheter procedures to treat congenital heart diseases in our country. It also assesses the implementation of hemodynamic techniques across different age groups. Its publication confirms the collaboration and commitment from both organizations to improve and consolidate it, as well as the dissemination of its outcomes.
METHODS
Data presented here come from an online, unaudited, voluntary, and retrospective registry that is updated on a yearly basis. All hospitals already participating in the Registry of Hemodynamics and Interventional Cardiology of the ACI-SEC, and all pediatric hospitals represented in the GTH-SECPCC were asked to participate. The study period goes from January 1, 2021 to December 31, 2021. Data mining was conducted via telematic format accessible for every participant center through the ACI-SEC official website.2
An external company—Tride Madrid, Spain—managed and analyzed the registry results, with help from members of the GTH-SECPCC and the ACI-SEC board of directors. After data cleaning, depuration, and analysis, discordant values or out of tendency at a given center were confirmed with the investigator responsible at such center.
Due to the methodological characteristics of the study, and since it is an activity registry only, it did not require the approval of the corresponding ethics committee, and informed consents were not deemed necessary
RESULTS
Resources and infrastructure
Back in 2021, participation included 16 hospitals, 15 from the public system and 1 private center (annex 1). A total of 34 cath labs with experience the management of congenital heart diseases were included, 7 of which had bi-plane systems, and 14 the possibility to perform rotational angiography. Only 7 (20.8%) were meant for pediatric patients only. Regarding the number of days per month dedicated to performing interventional procedures to treat congenital heart diseases in each center, a median of 7 days (4-18) was reported. In 13 centers (81.2%), 24-hour emergency hemodynamic monitoring was provided for patients with congenital heart disease including patients under 18 years old.
Regarding the amount of medical personnel available, a total of 56 interventional cardiologists with dedication to this activity were included, 27 (52%) and 29 (48%) of whom treated adult and pediatric patients, respectively.
Diagnostic procedures
A total of 1094 diagnostic studies were performed, which is a 5.1% increase in the activity displayed compared to the previous year. Distribution per age rage was: 50 (4.6%) cardiac catheterizations were performed in patients under 1 month old, 117 (10.7%) in patients between 1 month and 1 year, 497 (45.4%) in patients between 1 and 18 years, and 430 (39.3%) in patients over 18 years.
A total of 93 (8.5%) were categorized as emergency procedures. Regarding morbidity, a total of 6 (0.5%) cases of severe complications were reported: 4 vascular and 2 severe hemodynamic instabilities, 1 of which was of anaphylactic etiology. No mortality associated with this type of cardiac catheterizations was reported.
Interventional procedures
A 6.4% increase in the activity reported was seen compared to the previous year: a total of 1553 therapeutic cardiac catheterizations grouped into 13 different categories was reported with the following age distribution: 133 (8.6%) procedures in patients under 1 month, 182 (11.7%) in patients between 1 month and 1 year, 821 (52.9%) in patients between 1 and 18 years, and 417 (26.9%) in patients > 18 years (table 1).
Table 1. Number of interventional procedures performed and distribution by age group
| Variable | Total | Fetal | < 1 month | 1 month to 1 year | 1 to 18 years | > 18 years |
|---|---|---|---|---|---|---|
| Interventional procedures | 1553 | 0 | 133 (8.6) | 182 (11.7) | 821 (52.9) | 417 (26.9) |
| Congenital aortic valvuloplasty | 45 | 0 | 13 (28.9) | 10 (22.2) | 22 (48.9) | 0 |
| Congenital pulmonary valvuloplasty | 104 | 0 | 33 (31.7) | 30 (28.8) | 26 (25.0) | 15 (14.4) |
| Congenital mitral valvuloplasty | 1 | – | 0 | 0 | 1 (100) | 0 |
| Pulmonary angioplasty | 108 | – | 5 (4.6) | 4 (3.7) | 56 (51.9) | 43 (39.8) |
| Pulmonary branch angioplasty | 231 | – | 1 (0.4) | 31 (13.4) | 150 (64.9) | 49 (21.2) |
| Aortic angioplasty | 123 | – | 5 (4.1) | 32 (26.0) | 57 (46.3) | 29 (23.6) |
| Other angioplasties | 119 | – | 15 (12.6) | 18 (15.1) | 51 (42.9) | 35 (29.4) |
| Closure of atrial septal defect/foramen ovale | 336 | – | – | 2 (0.6)a | 161 (47.9) | 173 (51.5) |
| Closure of ductus arteriosus | 228 | 19 (8.3)b | 19 (8.3)b | 30 (13.2)b | 157 (68.9) | 3 (1.3) |
| Closure of ventricular septal defect | 27 | – | – | 3 (11.1)a | 18 (66.7) | 6 (22.2) |
| Other occlusions | 80 | – | 1 (1.3) | 8 (10.0) | 55 (68.8) | 16 (20.0) |
| Foreign body removal | 26 | – | 1 (3.8) | 1 (3.8) | 18 (69.2) | 6 (23.1) |
| Atrial septostomy and transseptal puncture | 54 | – | 31 (57.4) | 5 (9.3) | 17 (31.5) | 1 (1.9) |
| Transcatheter aortic valve implantation | 75 | – | – | – | 32 (42.7)c | 43 (57.3) |
a In this case, data were not collected separately < 1 month and 1 month to1 year, which is why the value corresponds to < 1 year. | ||||||
A total of 172 cardiac catheterizations were considered emergency procedures (11.8% of the total). Regarding the number of interventional procedures performed in each center, 4 hospitals (23.5%) reported > 150 cardiac catheterizations, 5 (29.4%) between 75 and 150 procedures while in the remaining 8 (47.1%) < 75 procedures were reported. The overall effectiveness reported from the different interventional techniques used was 95%—> 90% in most of them (table 2). Regarding morbidity and mortality data associated with this type of cardiac catheterizations, a total of 42 serious events (table 3) were reported including 3 deaths. Therefore, the rates of major complications and mortality were 2.7% and 0.2%, respectively. The following were common complications: 15 cases of device embolization, 8 cases of vascular complications, and 7 cases of hemodynamic instability with associated cardiac arrest. Regarding the 3 deaths reported, 1 was due to pulmonary valve implantation, 1 due to an aortic angioplasty performed, and 1 to ductal stent implantation.
Table 2. Efficacy summary reported of all interventional procedures
| Interventional procedure | N | Successful | Ineffective |
|---|---|---|---|
| Congenital aortic valvuloplasty | 45 | 40 (88.9) | 5 (11.1) |
| Congenital pulmonary valvuloplasty | 104 | 95 (91.3) | 9 (8.7) |
| Congenital mitral valvuloplasty | 1 | 1 (100) | 0 |
| Pulmonary angioplasty | 108 | 104 (96.3) | 4 (3.7) |
| Pulmonary branch angioplasty | 231 | 216 (93.5) | 15 (6.5) |
| Aortic angioplasty | 123 | 120 (97.6) | 3 (2.4) |
| Other angioplasties | 119 | 113 (95.0) | 6 (5.0) |
| Closure of atrial septal defect/foramen ovale | 336a (331) | 321 (97.0) | 10 (3.0) |
| Closure of ductus arteriosus | 228 | 223 (97.8) | 5 (2.2) |
| Closure of ventricular septal defect | 27b (22) | 17 (77.3) | 5 (22.7) |
| Other occlusions | 80 | 80 (100) | 0 |
| Foreign body removal | 26 | 23 (88.5) | 3 (11.5) |
| Atrial septostomy and transseptal puncture | 54c (53) | 53 (100) | 0 |
| Transcatheter aortic valve implantation | 75 | 63 (84.0) | 12 (16.0) |
| Total | 1553d (1546) | 1469 (95.0) | 77 (5.0) |
a Percentages estimated on 331 reported. | |||
Table 3. Distribution of major complications and death across the different interventional procedures performed
| Variable | N | Major complications | Death |
|---|---|---|---|
| Congenital aortic valvuloplasty | 45 | 5 (11.1): 1 mitral rupture 1 thrombosis of arterial access 3 cardiac arrests | 0 |
| Congenital pulmonary valvuloplasty | 104 | 4 (3.8): 1 pulmonary perforation requiring emergency surgery 1 thrombosis of arterial access 2 cardiac arrests | 0 |
| Congenital mitral valvuloplasty | 1 | 0 | 0 |
| Pulmonary angioplasty | 108 | 3 (2.8): 2 embolizations (1 requiring surgery) 1 pleural effusion requiring drainage | 0 |
| Pulmonary branch angioplasty | 231 | 4 (1.7): 2 vascular dissections 1 pulmonary hemorrhage 1 ischemia | 0 |
| Aortic angioplasty | 123 | 6 (4.9): 4 vascular dissections 1 cardiac arrest 1 death | 1 |
| Other angioplasties | 119 | 1 death (0.8) | 1 |
| Closure of atrial septal defect/foramen ovale | 336a (331) | 8 (2.4): 3 embolizations requiring surgery 5 embolizations not requiring surgery | 0 |
| Closure of ductus arteriosus | 228 | 2 (0.9): 1 arterial pseudoaneurysm 1 Moderate TR in PTNB | 0 |
| Closure of ventricular septal defect | 27b (22) | 4 (18.2): 1 embolization requiring surgery 1 embolization not requiring surgery 1 atrioventricular block 1 rupture of the device delivery system that required surgery | 0 |
| Other occlusions | 80 | 1 (1.3): 1 embolization not requiring surgery | 0 |
| Foreign body removal | 26 | 0 | 0 |
| Atrial septostomy and transseptal puncture | 54c (53) | 2 (3.8): 1 severe arrhythmia 1 cardiac arrest | 0 |
| Transcatheter aortic valve implantation | 75 | 6 (8.0): 1 embolization requiring surgery 1 embolization not requiring surgery 1 dissection of pulmonary conduit 1 coronary thrombosis 1 perforation of pulmonary lobar artery 1 death | 1 |
| Total | 1553d (1546) | 42 (2.7) | 3 (0.2) |
a Percentages estimated on 331 reported. | |||
Percutaneous valvuloplasties
A total of 45 aortic valvuloplasties were performed on congenital aortic stenoses; 23 (51.1%) in patients < 1 year, 13 of whom (28.9%) were under 1 month. In 68.8% of the cases, treatment-naïve native valves were dilated.
A total of 104 pulmonary valvuloplasties were reported. Again, the most numerous age range with 63 (60.5%) cases were patients < 1 year, 33 (31.7%) of whom were under 1 month. A total of 78 procedures (75%) were performed on native valves, 5 (4.8%) of which were imperforated. In 3 cases only the implantation of a ductal stent followed the procedure to optimize the pulmonary output.
Finally, only 1 case of successful mitral valvuloplasty on a previously treated valve was reported.
Percutaneous angioplasties
A total of 108 right ventricular outflow tract dilatations were reported, 43 (39.8%) of which were performed in patients > 18 years. The technical and anatomical data of 106 (98.1%) procedures were reported: in 60% and 40% of these both the surgical conduits and native tracts were dilated, respectively. In 69 (65.7%) cardiac catheterizations, angioplasties with stenting were performed. The rest with conventional balloons.
Pulmonary branch angioplasty entailed 231 procedures. The age group with the largest number of dilatations performed was patients between 1 and 18 years with 150 (64.9%) cases. In 206 (89.1%) cardiac catheterizations, the proximal branches were dilated while in the remaining ones peripheral arteries (lobar-segmental) were dilated. Regarding the angioplasty technique used, conventional balloon dilatation was used in 120 (51.9%) cardiac catheterizations, stenting in 106 (45,8%), and cutting balloon dilatation only in 5 (21%).
A total of 123 aortic angioplasties were reported, which is a 12.8% increase compared to the previous year. Also in this category, the age group that accumulated more cases was the 1 to 18 years group with 57 catheterizations (46.3%). A total of 88 procedures (80.7%) were reinterventions, and 35 (19.3%) procedures on native aortas. The anatomic substrate of dilatation was the aortic arch/isthmus in 94.5% of the cases, and the ascending aorta and abdominal aorta only in 5 and 2 cases, respectively. The data reported on the dilatation technique used distributed as follows: conventional balloon angioplasties, 25.2%; uncovered stent implantation, 36%; covered stent implantation, 24.3%; and re-dilatation with previous balloon-expandable stent implantation, 19.5%.
Also, a total of 119 catheterizations grouped under “other angioplasties” category were reported, which is a 30.7% increase with respect to the previous year. The anatomical substrate of angioplasty was reported in 100 cases (84%). In addition, systemic vein dilatations were performed in 22 cases, Fontan procedures in 21, closure of ductus arteriosus in 14, and surgical fistulae in 8. Stenting was associated with 55% of all procedures described.
Shunt closures and other occlusion devices
Same as in the report published in 2020, atrial septal defect closure was the registry most widely performed interventional procedure: 336 cases; 173 (51.5%) of which were performed in patients > 18 years. The defect anatomical substrate had the following distribution: simple atrial septal defect closures (single hole, borders > 5 mm, nonaneurysmal septum) in 123 (36,.6%); complex atrial septal defect closures in 77 (21,7%), and patent foramen ovale in 136 (40.4%). The most widely used imaging modality to guide closure was transesophageal echocardiography in259 (77%) procedures. Intracardiac ultrasound and angiographic measurement with balloon were only used in 12.7% of the cases.
Closure of ductus arteriosus experienced a 20.6% increase compared to the previous year with 189 cardiac catheterizations. The group of patients from 1 to 18 years amounted to 68.9% of all procedures performed while the group of premature patients reached 8.3% (19 cases). Antegrade venous access was the route of choice in 60% of all closures. Occluders were used in 82.4% of the cases reported while controlled delivery coil systems were used in the remaining cases.
In this registry, closure of ventricular septal defect represented 27 cases only, which was a 32.4% drop in the number of cases compared to 2020. A total of 77.8% of all procedures were performed in patients under 18 years. Distribution based on the anatomical typology was: perimembranous in 18 cases (66.6%), postoperative in 7 (25.9%), and muscular in 2 (7.4%). In 55.5% of the cases occluders were used, and controlled delivery coil systems in the remaining ones (44.5%). All devices were implanted transcatheterly.
Within the “other occlusion procedures” category, a total of 106 catheterizations were performed with a 24.5% drop in the volume of procedures performed compared to the previous year. Data on the type of occlusion used were reported in 76 (95%) cases like closure of systemic-to-pulmonary artery collateral vessels in 46 (60,5%), closure of venous collaterals in 10 (13.1%), closure of surgical fistulae in 7 (9.2%), and closure of coronary fistulae in 6 (7.8%). The most widely used materials were occluders (37.5%) followed by coil systems (25%), and particles (16.2%).
Atrial septostomy
In this category a total of 54 procedures were reported, which is a 20.6% drop compared to the previous year. Regarding imaging guidance, the echocardiography was used in 21% of the cases, fluoroscopy guidancein 34.6%, and both techniques combined in 44.2%. A total of 32 (56.1%) procedures were balloon atrial septostomies (Rashkind procedure). Also, 13 procedures were reported with radiofrequency assisted septal perforation, 9 with needle perforation, and 10 with septal stenting.
Transcatheter aortic valve implantation
A total of 75 procedures were reported, which is a 29.3% increase compared to 202. Up to 43 (57.3 %) cardiac catheterizations were performed in patients over 18 years old. Transcatheter implantation was the rule in all the cases. A total of 63 valves were implanted in the pulmonary position, 10 in the tricuspid position, and 2 in the mitral position.
DISCUSSION
2021 can be considered the year we came back from the COVID-19 pandemic. In this year’s report, the Spanish Registry of Hemodynamic and Interventional Cardiology Activity confirms this recovery compared to 2020. It is especially interesting to see the increased number of structural heart and congenital procedures performed among the adult population reaching all-time maximum levels of activity.3,4
This tendency that demonstrates activity has come back can also be seen in this year’s report thanks to comparison with the data available from the 2019-2021 Spanish Cardiac Catheterization in Congenital Heart Diseases Registry (figure 1). It shows a 6.4% overall increase of most interventional procedures performed, especially those associated with closure of ductus arteriosus, transcatheter aortic valve implantation, and aortic angioplasty.
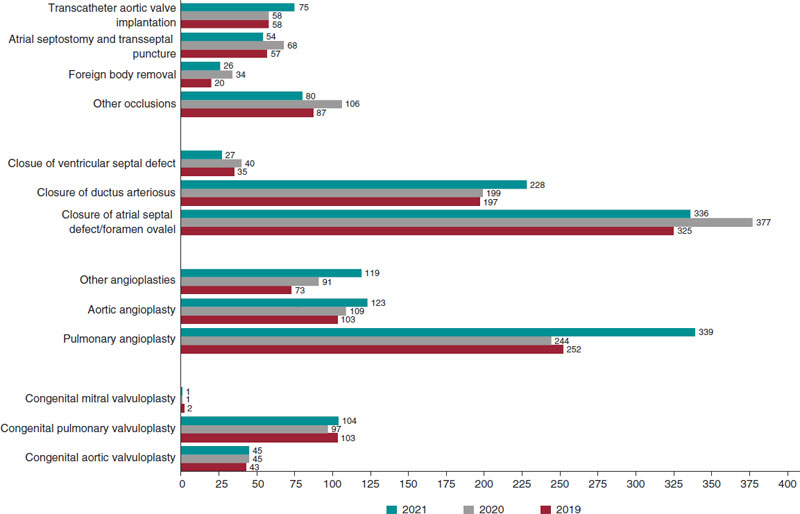
Figure 1. Comparison of the number of interventional procedures performed back in 2019, 2020, and 2021.
Diagnostic catheterization also increased its volume up to 5.1% reaching 1094 procedures performed, which is a 41.3% of the overall cardiac catheterizations reported by the registry. These data confirm the relevance of these procedures in the management of patients with congenital heart disease across all age ranges despite the evolution of imaging modalities.
The overall number of interventional procedures reported was 1553. A total of 73.2% were performed in patients < 18 years old, which shows the predominance of pediatric activity in this registry. However, 2 techniques accumulated the highest percentage of cases in the segment of patients > 18 years: the closure of atrial septal defect (51.5%), and transcatheter aortic valve implantation (57.3%). The analysis of data from the 2021 Spanish Registry of Hemodynamic and Interventional Cardiology Activity reveals, once again, the limitation of this report to show the true volume of interventional activity displayed in adult patients with congenital heart disease. Some techniques like the closure of atrial septal defect, the closure of ductus arteriosus or transcatheter pulmonary valve implantation are still underestimated.4 Conversely, the scarce fetal interventional activity displayed in Spain can be seen in the lack of cases reported despite evidence of its true value and effectiveness in certain prenatal settings of aortic stenosis, pulmonary atresia with intact ventricular septum or hypoplastic left heart syndrome.5
The overall data and results of the different interventional techniques available show efficacy and mortality rates of 95% and 0.2%, respectively with just 3 deaths associated with these procedures. These data are very similar to those reported the year before and still consistent with those expected according to different international studies.6-8 The rate of serious adverse events, however, has increased significantly (2.7%) with up to 42 major complications compared to the 2% reported back in 2020. Embolizations of different materials still gather the largest number of events reported (19% of the total). Still, they have not gone up as opposed to vascular complications and episodes of hemodynamic instability with associated cardiac arrest that have increased. The improved registry data collection and depuration process could partly explain this increased morbidity reported. Still, it will be interesting to see its evolution in future reports.
Some changes introduced in the registry design have also improved information on some interventional techniques. The “pulmonary angioplasty” has split into 2 separate categories: a category including angioplasties of pulmonary conduits or right ventricular native tracts, and a category including pulmonary branch dilatations. Therefore, the overall increase of cases has been very significant (71%). However, this methodological change does not allow any comparisons with previous years. Also, it has allowed us to know new technical details associated with these procedures: the anatomical concentration of most angioplasties on the proximal segments of pulmonary arteries (89.9%) could explain the scarce use of cutting balloons in this category since it would be more suitable to treat resistant peripheral stenoses rather than conventional dilatations.9 Within aortic angioplasties, the brand-new reporting of data on the anatomical setting of dilatations allowed to confirm that angioplasties of ascending or abdominal aorta are extremely rare, most cases being dilatations of aortic arch or isthmus (94.5%).
Regarding valvuloplasties, their volume has remained almost unchanged compared to the previous year being most of them performed in patients < 1 year. In aortic valvuloplasty, the high rate of serious events reported (11.1%) is surprising although with no associated mortality, as well as the 89.9% efficacy rate that also worsens a little bit the previous results confirming its status as a high-risk technique, especially in the neonatal setting. Nonetheless, its role as therapeutic option vs repair surgery is still strong and consistent with the medical literature available to this date.10
The closure of atrial septal defect is again the interventional procedure most widely used according to the registry, although with a slight 10% drop compared to the previous year. The use of intracardiac ultrasound and balloon measurements as support techniques of closure procedures is still scarce. The development of new devices confirms the strength of this technique while the arrival of new materials could reduce potential morbidities in the mid- and the long-term.11,12
The closure of ductus arteriosus has increased its volume by 20% being very significant the increased number of cases reported in premature patients (8.3% of the total). Therefore, the margin for growth of this technique in this group of pediatric patients seems evident. In the meantime, other studies are being published on the strength of this procedure compared to the surgical closure option.13 We should mention that this is one of the techniques with better efficacy results and lower rates of complications, which reveals the maturity of its implantation in our country.
Same as in former reports, the least effective technique reported (77.3%) is the closure of ventricular septal defect that still has a high rate of complications (18%) whose volume keeps dropping significantly. These data confirm its technical difficulty and scarce implantation in our setting. However, the introduction of new closure devices like the adoption of a few technical modifications to the traditional approach could be a paradigm shift supported by recent reports from Spanish interventional working groups.14,15
Another technique that is expanding significantly is transcatheter aortic valve implantation; however, its increase (29%) is almost exclusively associated, with patients > 18 years. The data reported on its efficacy (84%) and rate of complications (8%) reflect how this technique has grown in our setting with the corresponding learning curve. Regarding the anatomical substrate of implantation, the tricuspid position has reached a significant 13% overall, being implantations in the mitral position exceptionally rare. The availability of new clinically validated valves16 is still improving transcatheter treatment options for patients with a dysfunctional right ventricular outflow tract (the group that benefited the most from this procedure).
Limitations
The deficient estimate of interventional procedures in patients > 18 years can be considered the main weakness of this registry. The number of participant centers, though representative of the pediatric activity displayed, is still scarce and does not show the actual activity displayed to treat congenital heart disease in the adult population in our country. Fixing this limitation will be the main goal of future registries.
From the methodological standpoint, the parameters of success of certain interventional procedures were not reported, thus assuming the uniformity of criterion of all participants. Furthermore, the scarce information collected on certain techniques like transcatheter aortic valve implantation can diminish the impact of the results obtained. The wider use of this procedure and the addition of new procedures of special interest —like interventional procedures of congenital aortic valve disease— should be considered in future iterations of the registry.
CONCLUSIONS
A significant increase in the activity displayed in both cardiac catheterizations and most interventional procedures was reported throughout 2021. A significant increase was seen in the use of procedures like transcatheter aortic valve implantation, closure of ductus arteriosus, and aortic angioplasty. Diagnostic catheterization still plays a key role in the management of patients with congenital heart disease across all age ranges. The safety and efficacy results of most interventional techniques are similar to those reported by the best international registries.
Participation in this registry of a larger number of centers with interventional activity in congenital heart disease will help us achieve a more realistic approach to its true dimension in the years to come.
FUNDING
None whatsoever.
AUTHORS’ CONTRIBUTIONS
All authors contributed substantially to data mining, and the manuscript critical review process. F. Ballesteros Tejerizo, F. Coserría Sánchez, and X. Freixa also designed and drafted the manuscript.
CONFLICTS OF INTEREST
S. Ojeda Pineda is an associate editor of REC: Interventional Cardiology; the journal’s editorial procedure to ensure the impartial handling of the manuscript has been followed. The remaining authors declared no conflicts of interest whatsoever.
WHAT IS KNOWN ABOUT THE TOPIC?
- Cardiac catheterization is the cornerstone in the management of patients with congenital heart disease.
- Numerous interventional techniques available that apply in this field across all age ranges from fetal to the adult age.
- Knowledge on the degree of implantation of all these techniques in our country and the results reported is still limited.
- The availability of a national registry of pediatric transcatheter procedures and adult congenital procedures is essential for patients, families, and health professionals involved.
WHAT DOES THIS STUDY ADD?
- A significant increase of activity was reported during 2021 being transcatheter aortic valve implantation, closure of ductus arteriosus, and aortic angioplasty the techniques that have grown the most.
- Procedures most performed are the closure of atrial septal defect, angioplasty of pulmonary branches, and the closure of ductus arteriosus.
- Data on the safety and efficacy profile of most techniques are consistent with the results published in the medical literature available to this date.
- Device embolization leads the list of complications associated with the procedures described. Also, vascular complications, and episodes of hemodynamic instability have increased with associated cardiac arrests during cardiac catheterization.
ANNEX 1
Centers participating in the Spanish Cardiac Catheterization in Congenital Heart Diseases Registry (in alphabetical order)
| Complexo Hospitalario Universitario, A Coruña, Spain |
| Hospital Clínico Universitario de Valladolid, Valladolid, Spain |
| Hospital Regional Universitario de Málaga (Materno-Infantil), Málaga, Spain |
| Hospital Universitario de Cruces, Barakaldo, Bizkaia, Spain |
| Hospital Universitario 12 de Octubre (Instituto Pediátrico del Corazón), Madrid, Spain |
| Hospital Universitario Gregorio Marañón, Madrid, Spain |
| Hospital Universitario La Paz, Madrid, Spain |
| Hospital Universitario y Politécnico La Fe, Valencia, Spain |
| Hospital Universitario Ramón y Cajal, Madrid, Spain |
| Hospital Universitario Reina Sofía, Córdoba, Spain |
| Hospital Universitario Son Espases, Palma de Mallorca, Spain |
| Hospital Universitario Vall d’Hebron, Barcelona, Spain |
| Hospital Universitario Virgen de la Arrixaca, Murcia, Spain |
| Hospital Universitario Virgen de las Nieves, Granada, Spain |
| Hospital Universitario Virgen del Rocío, Sevilla, Spain |
| Hospital Vithas 9 de Octubre, Valencia, Spain |
REFERENCES
1. Ballesteros Tejerizo F, Coserría Sánchez F, Romaguera R, et al. Registro español de intervencionismo en cardiopatías congénitas. Primer informe oficial de la ACI-SEC y el GTH-SECPCC (2020). REC Interv Cardiol. 2022;4:173-180.
2. Asociación de Cardiología Intervencionista de la Sociedad Española de Cardiología. Registro de Actividad ACI-SEC. Available at: http://www.registroactividadacisec.es. Accessed 21 Jun 2022.
3. Romaguera R, Ojeda S, Cruz-González I, et al. Registro Español de Hemodinámica y Cardiología Intervencionista. XXX Informe Oficial de la Asociación de Cardiología Intervencionista de la Sociedad Española de Cardiología (1990-2020) en el año de la pandemia de la COVID-19. Rev Esp Cardiol. 2021;74:1096-1106.
4. Freixa X, Jurado-Román A, Cid B, et al. Registro español de hemodinámica y cardiología intervencionista. XXXI Informe oficial de la Asociación de Cardiología Intervencionista de la Sociedad Española de Cardiología (1990-2021). Rev Esp Cardiol. 2022;75:1040-1049.
5. Friedman KG, Tworetzky W. Fetal cardiac interventions: Where do we stand? Arch Cardiovasc Dis. 2020;113:121-128.
6. Kevin D, Wei Du, Fleming GA, et al. Validation and refinement of the catheterization RISK score for pediatrics (CRISP score): An analysis from the congenital cardiac interventional study consortium. Catheter Cardiovasc Interv. 2019;93:97-104.
7. Taggart NW, Du W, Forbes TJ, et al. A Model for Assessment of Catheterization Risk in Adults With Congenital Heart Disease. Am J Cardiol. 2019;123:1527-1531.
8. Quinn BP, Ye M, Gauvreau K, et al. Procedural Risk in Congenital Cardiac Catheterization (PREDIC3T). J Am Heart Assoc. 2022;11:e022832.
9. Holzer R, Gauvreau K, Kreutzer J, et al . Balloon Angioplasty and Stenting of Branch Pulmonary Arteries. Adverse Events and Procedural Characteristics: Results of a Multi-Institutional Registry. Circ Cardiovasc Interv. 2011;4:287-296.
10. Thu Saung M, McCracken C, Sachdeva R, Petit CJ. Outcomes Following Balloon Aortic Valvuloplasty Versus Surgical Valvotomy in Congenital Aortic Valve Stenosis: A Meta-Analysis. J Invasive Cardiol 2019;31:E133-E142.
11. Jalal Z, Hascoët S, Gronier C, et al. Long-Term Outcomes After Percutaneous Closure of Ostium Secundum Atrial Septal Defect in the Young. JACC Cardiov Interv. 2018;11:795-804.
12. Li Y, Xie Y, Li B, et al. Initial Clinical Experience with the Biodegradable AbsnowTM Device for Percutaneous Closure of Atrial Septal Defect: A 3-Year Follow-Up. J Interv Cardiol. 2021;2021:6369493.
13. Sathanandam S, Gutfinger D, Morray B, et al. Consensus Guidelines for the Prevention and Management of Periprocedural Complications of Transcatheter Patent Ductus Arteriosus Closure with the Amplatzer Piccolo Occluder in Extremely Low Birth Weight Infants. Pediatr Cardiol. 2021;42:1258-1274.
14. álvarez-Fuente M, Carrasco JI, Insa B, et al. Cierre percutáneo de comunicación interventricular con el dispositivo KONAR-MF. REC Interv Cardiol. 2022;4:181-185.
15. Rasines Rodríguez A, Aristoy Zabaleta MM, Abelleira Pardeiro C, et al. Cierre percutáneo de comunicaciones interventriculares perimembranosas por vía retrógrada. Cambio de paradigma. REC Interv Cardiol. 2023;5:73-75.
16. Morgan G, Prachasilchai P, Promphan W, et al. Medium-term results of percutaneous pulmonary valve implantation using the Venus P-valve: international experience. EuroIntervention. 2019;14:1363-1370.
* Corresponding author.
E-mail address: fernandoballe@gmail.com (F. Ballesteros Tejerizo).