Aortic pseudoaneurysm is a rare and serious complications after surgical aortic valve replacement. Its appearance in the reimplantation region of coronary arteries has been documented on very few occasions.
This is the case of a 53-year-old man with a Stanford type A acute aortic dissection. The aortic root and ascending aorta were replaced with coronary artery reimplantation (modified Bentall-Bono technique) with favorable early disease progression.
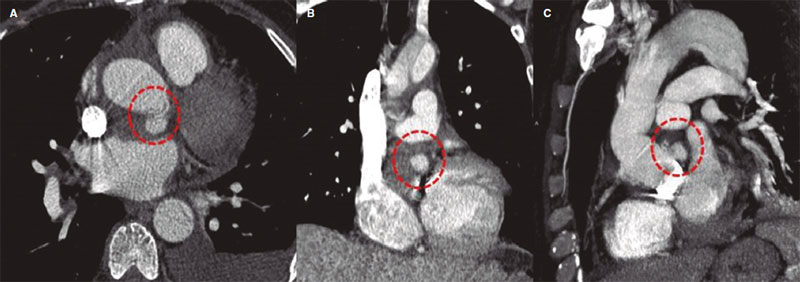
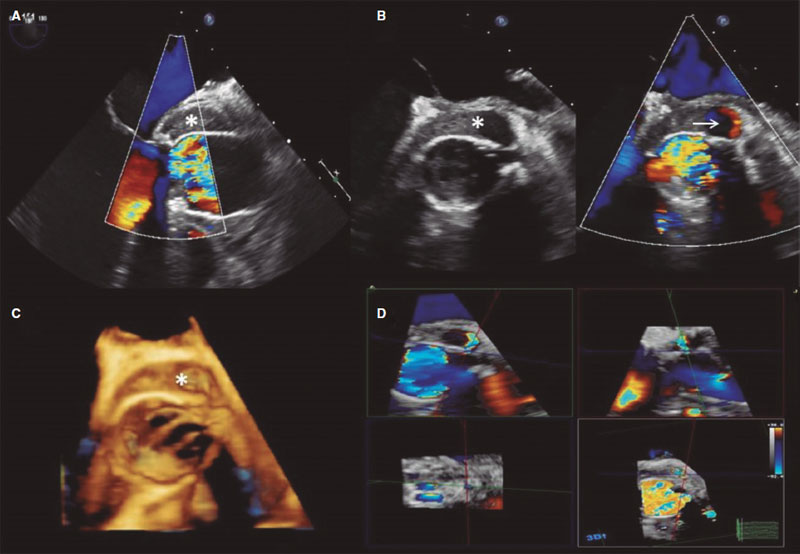
The thoracoabdominal computed tomography scan performed 25 days after surgery to study an incidental renal mass revealed the presence of a 14 mm x 10 mm hyperdense nodular image in the arterial phase of posterior location with respect to the left main coronary artery ostium consistent with a postoperative pseudoaneurysm (figure 1A,C, circle). A 3D transesophageal echocardiography confirmed the presence of a pseudoaneurysm surrounding the aortic root with flow inside stemming from the suture of the left main coronary artery (figure 2A,D, asterisk and arrow).
Figure 1.
Figure 2.
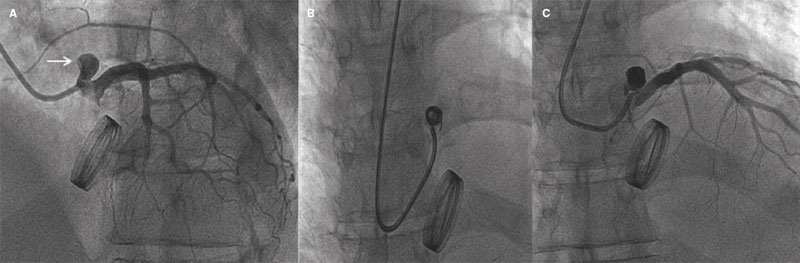
Given the high risk of reintervention, the coronary angiography confirmed the presence of a shunt between the suture of left main coronary artery and the saccular space of pseudoaneurysm (figure 3A, arrow). Selective microcatheterization of this sac was performed (PX SLIM, Penumbra Inc., United States; microcatheter with a minimum inner lumen of 0.025 inch) with insertion of 2 0.020 inch mechanical platinum coils for controlled delivery (Penumbra Coil 400, Penumbra Inc., United States) for a total length of 55 mm. The fistula was closed with good immediate results (figure 3B,C, and videos 1-4 of the supplementary data).
Figure 3.
The 3D transesophageal echocardiography performed 30 days after the procedure revealed a minimum residual flow towards the pseudoaneurysm (video 5 of the supplementary data). The computed tomography scans performed at follow-up showed no residual shunt and good disease progression.
The transcatheter approach is a promising alternative to surgery to treat coronary pseudoaneurysms after Bentall procedure, especially in high-surgical risk patients.
The patient’s informed consent was obtained for publication purposes.
FUNDING
None whatsoever.
AUTHORS’ CONTRIBUTIONS
All the authors have been involved in the process of drafting this manuscript. They all read and approved its final version for publication purposes.
CONFLICTS OF INTEREST
None reported.
SUPPLEMENTARY DATA
Vídeo 1. González Lizarbe S. DOI: 10.24875/RECICE.M23000368
Vídeo 2. González Lizarbe S. DOI: 10.24875/RECICE.M23000368
Vídeo 3. González Lizarbe S. DOI: 10.24875/RECICE.M23000368
Vídeo 4. González Lizarbe S. DOI: 10.24875/RECICE.M23000368
Vídeo 5. González Lizarbe S. DOI: 10.24875/RECICE.M23000368